University Blood Grouping Analysis: Tube Technique for ABO and Rh
VerifiedAdded on 2022/08/10
|11
|3312
|416
Practical Assignment
AI Summary
This assignment details the application of the tube technique for determining ABO and Rh blood groups of a patient (ZK) and his five siblings, in preparation for a potential renal transplant. The process involves mixing red blood cells with antibodies, incubating, centrifuging, and assessing for agglutination to identify the presence of A, B, and RhD antigens. Results showed ZK having A (α, β) RhD (+) blood type, sibling 1 as AB (Ø) RhD (-), sibling 2 as A (β) RhD (+), sibling 3 as O (α, β) RhD (+), sibling 4 as A (β) RhD (+), and sibling 5 as AB (Ø) RhD (+). The findings are discussed in relation to blood transfusion and renal transplantation, highlighting the importance of matching blood groups. The assignment also acknowledges limitations, such as potential human error and the subjectivity in agglutination scoring, while concluding that siblings 2 and 3 are suitable donors for ZK based on their blood group compatibility, successfully fulfilling the experiment's objective.

Running head: IMMUNOLOGICAL ANALYSIS
TUBE
TECHNIQUE:
DETERMINATIO
N OF ABO AND
Rh BLOOD
GROUPING FOR
ZK AND FIVE
SIBLINGS
Name of the Student
Name of the University
Author note
TUBE
TECHNIQUE:
DETERMINATIO
N OF ABO AND
Rh BLOOD
GROUPING FOR
ZK AND FIVE
SIBLINGS
Name of the Student
Name of the University
Author note
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

1
IMMUNOLOGICAL ANALYSIS
Abstract
Tube-technique is a technique used in determining blood grouping. ZK needs renal
transplantation, and his blood type needs to match with anyone his 5 siblings for
transplantation. Donor Red blood cell (RBC) was mixed with antibody and was then
incubated for a time of about five to ten minutes at normal temperature. Tubes were then
centrifuged for 15 sec on 1000rpm. Tubes were assessed for agglutination reaction, and it was
scored depending on the degree of agglutination reaction ranging from +4 to +1. Samples
without any agglutination reaction were marked as ‘Neg’ signifying negative. The result
showed that the ZK has A (α, β) RhD (+) blood type, sibling 1 have AB (Ø) RhD (-), sibling
two A (β) RhD (+), sibling three O (α, β) RhD (+), sibling four A (β) RhD (+) and sibling
five as AB (Ø) RhD (+). Successful determination of ABO cell and serum was done with
tube technique with minor limitation as it can include human miscalculation.
IMMUNOLOGICAL ANALYSIS
Abstract
Tube-technique is a technique used in determining blood grouping. ZK needs renal
transplantation, and his blood type needs to match with anyone his 5 siblings for
transplantation. Donor Red blood cell (RBC) was mixed with antibody and was then
incubated for a time of about five to ten minutes at normal temperature. Tubes were then
centrifuged for 15 sec on 1000rpm. Tubes were assessed for agglutination reaction, and it was
scored depending on the degree of agglutination reaction ranging from +4 to +1. Samples
without any agglutination reaction were marked as ‘Neg’ signifying negative. The result
showed that the ZK has A (α, β) RhD (+) blood type, sibling 1 have AB (Ø) RhD (-), sibling
two A (β) RhD (+), sibling three O (α, β) RhD (+), sibling four A (β) RhD (+) and sibling
five as AB (Ø) RhD (+). Successful determination of ABO cell and serum was done with
tube technique with minor limitation as it can include human miscalculation.

2
IMMUNOLOGICAL ANALYSIS
Introduction
Blood transfusion is defined as the transferral of products of blood or blood from one
individual to another. It is mainly used to replace products of blood or blood cells that are
absent due to surgery, severe blood flow or to increase the blood count in a patient with
anaemia (Alemu and Mama 2016). The transfusion is related to blood grouping. The blood
groups in human are ABO and RhD. If the transfusion is done with ABO-incompatible blood,
it causes severe fatal reactions. RhD is extremely immunogenic and ca lead to cell
haemolysis (Albánez et al. 2016). Blood transfusion has a role in renal transplantation. In
case of renal transplantation, the blood group for both the recipient and donor should match.
The experiment discussed below was conducted with samples from patient ZK is 33 years old
undergoing kidney transplantation from his siblings. There were five potential donors (S1-
S5). The patient and the siblings ABO group of blood and RhD kind must match so that
transplantation can be conducted. In this research, the tube technique was chosen for blood
typing analysis.
The main aim of the experimentation is to gain knowledge about blood grouping by
the use of tube technique to analyse the ABO and RhD typing for the patient and donor
blood.
Method and Material
Material
Shared one among four: One bottle of 10 ml Anti-A, a single container of 10 ml of
Anti-B, and a single container of 10 ml Anti-D. One bottle of 3 percent blood suspension of
‘A’ group red blood cells and one container of 3 percent blood suspension of B group blood.
Samples of the tests distributed between two: 3 percent suspension of blood sample of ZK,
serum sample for ZK, patient ZK and student identification number were used for patient
identification. Five 3 percent donor red blood suspension were labelled as S1 to S5. Each
suspension and student number used as a distinctive donor identifier. Equipment used in the
experiment were plastic Pasteur pipettes, LP4 test tubes for the collection of serum, in
addition, red blood cell group testing, one test-tube rack plus marker pen.
Method
Student 1 had set patient ZK’s and his sibling one and two ABO cell, serum as well as
RhD typing. Student two had set sibling three, four and five ABO cell and RhD typing and
IMMUNOLOGICAL ANALYSIS
Introduction
Blood transfusion is defined as the transferral of products of blood or blood from one
individual to another. It is mainly used to replace products of blood or blood cells that are
absent due to surgery, severe blood flow or to increase the blood count in a patient with
anaemia (Alemu and Mama 2016). The transfusion is related to blood grouping. The blood
groups in human are ABO and RhD. If the transfusion is done with ABO-incompatible blood,
it causes severe fatal reactions. RhD is extremely immunogenic and ca lead to cell
haemolysis (Albánez et al. 2016). Blood transfusion has a role in renal transplantation. In
case of renal transplantation, the blood group for both the recipient and donor should match.
The experiment discussed below was conducted with samples from patient ZK is 33 years old
undergoing kidney transplantation from his siblings. There were five potential donors (S1-
S5). The patient and the siblings ABO group of blood and RhD kind must match so that
transplantation can be conducted. In this research, the tube technique was chosen for blood
typing analysis.
The main aim of the experimentation is to gain knowledge about blood grouping by
the use of tube technique to analyse the ABO and RhD typing for the patient and donor
blood.
Method and Material
Material
Shared one among four: One bottle of 10 ml Anti-A, a single container of 10 ml of
Anti-B, and a single container of 10 ml Anti-D. One bottle of 3 percent blood suspension of
‘A’ group red blood cells and one container of 3 percent blood suspension of B group blood.
Samples of the tests distributed between two: 3 percent suspension of blood sample of ZK,
serum sample for ZK, patient ZK and student identification number were used for patient
identification. Five 3 percent donor red blood suspension were labelled as S1 to S5. Each
suspension and student number used as a distinctive donor identifier. Equipment used in the
experiment were plastic Pasteur pipettes, LP4 test tubes for the collection of serum, in
addition, red blood cell group testing, one test-tube rack plus marker pen.
Method
Student 1 had set patient ZK’s and his sibling one and two ABO cell, serum as well as
RhD typing. Student two had set sibling three, four and five ABO cell and RhD typing and
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

3
IMMUNOLOGICAL ANALYSIS
serum typing. The first step includes cell grouping, followed by serum grouping and
agglutination scoring.
Cell Grouping
LP4 test tubes were marked with university id number for student alongside with the
component existing in it such as anti-A, anti-B and anti-D whereas the test tubes for sibling
samples were marked with sibling number as well as student’s identification number along
with the reagent present in sibling blood. All these test-tubes were put in the stand of the test
tube. One single drip of the applicable component was added into each test-tube with the help
of Pasteur pipette. Donor RBC sample was suspended to make sure that homogeneity is
maintained. The moment the sample from the donor was placed inside the tube; it reaches the
base of the tube. A single drop of the cell suspension added into the tube and shook gentle for
conglomerating the mixture. The incubation time of the test tube was for five to ten minutes
at normal temperature and was centrifuged for fifteen secs at 1000 rpm. The serum was set
during the time of incubation.
Serum grouping
Patient and each sibling tubes were marked in place of their serum group B and A. In
every tube, two droplets of ZK or sibling plasma was put into each tube. A single drop of
reagent cells was also added into the marked tube. Cells and serum were mixed and was
incubated for 15 min at room temperature and was then centrifuged at a speed of 1000rpm for
the time of about 15 seconds. The cells were suspended and were then each sample were
checked under a microscope to note if there was any agglutination. All the results were noted
down in the worksheet. Results were interpreted at the end.
Scoring of Agglutination
Neg: means no agglutination; 1+: slight agglutinates; 2+: Slighter agglutinates,
nonetheless certainly noticeable properly, 3+: Robust agglutination observed, two-third huge
agglutinates; 4+: highly robust agglutination, not any free cells, single agglutination.
IMMUNOLOGICAL ANALYSIS
serum typing. The first step includes cell grouping, followed by serum grouping and
agglutination scoring.
Cell Grouping
LP4 test tubes were marked with university id number for student alongside with the
component existing in it such as anti-A, anti-B and anti-D whereas the test tubes for sibling
samples were marked with sibling number as well as student’s identification number along
with the reagent present in sibling blood. All these test-tubes were put in the stand of the test
tube. One single drip of the applicable component was added into each test-tube with the help
of Pasteur pipette. Donor RBC sample was suspended to make sure that homogeneity is
maintained. The moment the sample from the donor was placed inside the tube; it reaches the
base of the tube. A single drop of the cell suspension added into the tube and shook gentle for
conglomerating the mixture. The incubation time of the test tube was for five to ten minutes
at normal temperature and was centrifuged for fifteen secs at 1000 rpm. The serum was set
during the time of incubation.
Serum grouping
Patient and each sibling tubes were marked in place of their serum group B and A. In
every tube, two droplets of ZK or sibling plasma was put into each tube. A single drop of
reagent cells was also added into the marked tube. Cells and serum were mixed and was
incubated for 15 min at room temperature and was then centrifuged at a speed of 1000rpm for
the time of about 15 seconds. The cells were suspended and were then each sample were
checked under a microscope to note if there was any agglutination. All the results were noted
down in the worksheet. Results were interpreted at the end.
Scoring of Agglutination
Neg: means no agglutination; 1+: slight agglutinates; 2+: Slighter agglutinates,
nonetheless certainly noticeable properly, 3+: Robust agglutination observed, two-third huge
agglutinates; 4+: highly robust agglutination, not any free cells, single agglutination.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser
4
IMMUNOLOGICAL ANALYSIS
Results
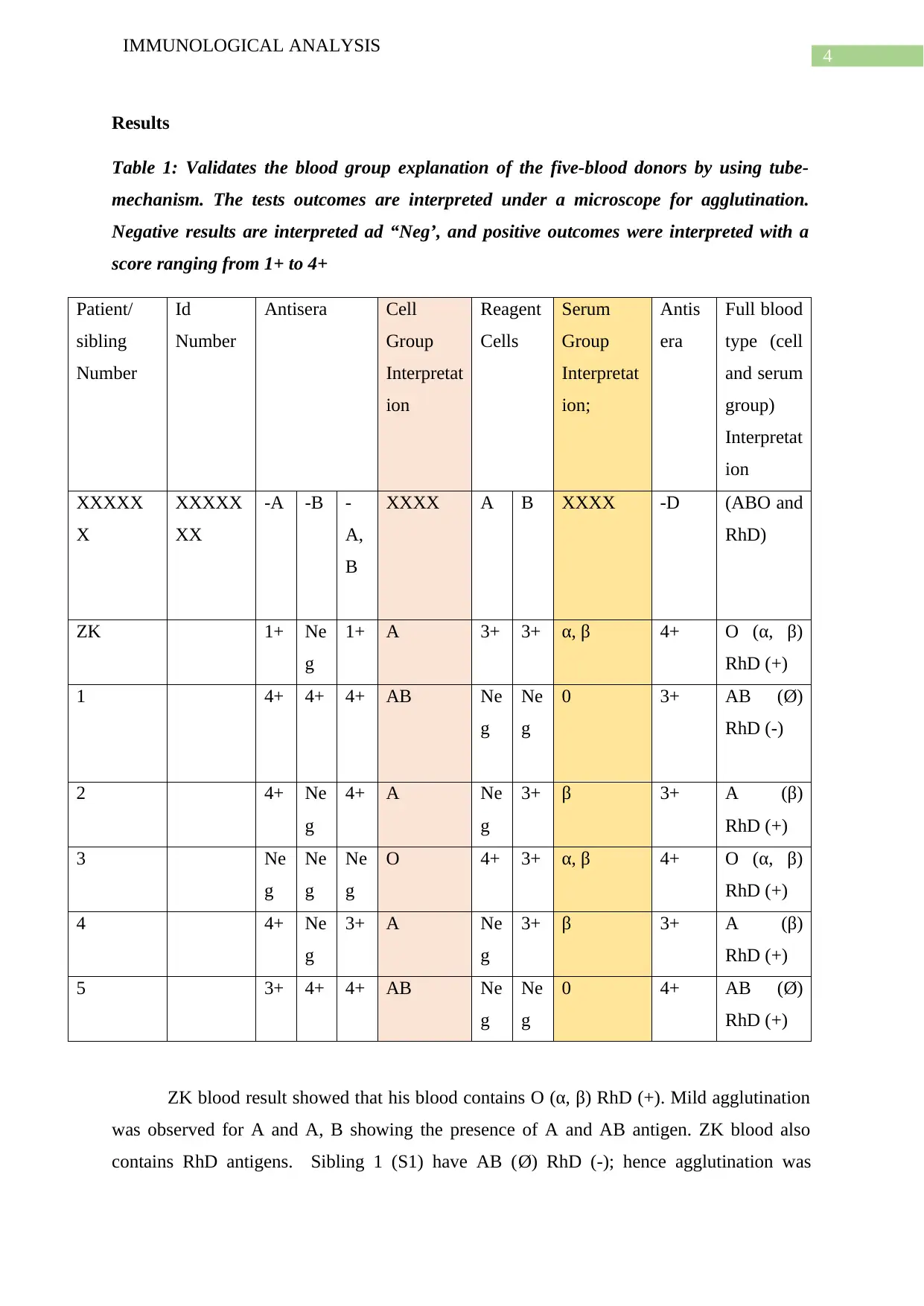
Table 1: Validates the blood group explanation of the five-blood donors by using tube-
mechanism. The tests outcomes are interpreted under a microscope for agglutination.
Negative results are interpreted ad “Neg’, and positive outcomes were interpreted with a
score ranging from 1+ to 4+
Patient/
sibling
Number
Id
Number
Antisera Cell
Group
Interpretat
ion
Reagent
Cells
Serum
Group
Interpretat
ion;
Antis
era
Full blood
type (cell
and serum
group)
Interpretat
ion
XXXXX
X
XXXXX
XX
-A -B -
A,
B
XXXX A B XXXX -D (ABO and
RhD)
ZK 1+ Ne
g
1+ A 3+ 3+ α, β 4+ O (α, β)
RhD (+)
1 4+ 4+ 4+ AB Ne
g
Ne
g
0 3+ AB (Ø)
RhD (-)
2 4+ Ne
g
4+ A Ne
g
3+ β 3+ A (β)
RhD (+)
3 Ne
g
Ne
g
Ne
g
O 4+ 3+ α, β 4+ O (α, β)
RhD (+)
4 4+ Ne
g
3+ A Ne
g
3+ β 3+ A (β)
RhD (+)
5 3+ 4+ 4+ AB Ne
g
Ne
g
0 4+ AB (Ø)
RhD (+)
ZK blood result showed that his blood contains O (α, β) RhD (+). Mild agglutination
was observed for A and A, B showing the presence of A and AB antigen. ZK blood also
contains RhD antigens. Sibling 1 (S1) have AB (Ø) RhD (-); hence agglutination was
IMMUNOLOGICAL ANALYSIS
Results
Table 1: Validates the blood group explanation of the five-blood donors by using tube-
mechanism. The tests outcomes are interpreted under a microscope for agglutination.
Negative results are interpreted ad “Neg’, and positive outcomes were interpreted with a
score ranging from 1+ to 4+
Patient/
sibling
Number
Id
Number
Antisera Cell
Group
Interpretat
ion
Reagent
Cells
Serum
Group
Interpretat
ion;
Antis
era
Full blood
type (cell
and serum
group)
Interpretat
ion
XXXXX
X
XXXXX
XX
-A -B -
A,
B
XXXX A B XXXX -D (ABO and
RhD)
ZK 1+ Ne
g
1+ A 3+ 3+ α, β 4+ O (α, β)
RhD (+)
1 4+ 4+ 4+ AB Ne
g
Ne
g
0 3+ AB (Ø)
RhD (-)
2 4+ Ne
g
4+ A Ne
g
3+ β 3+ A (β)
RhD (+)
3 Ne
g
Ne
g
Ne
g
O 4+ 3+ α, β 4+ O (α, β)
RhD (+)
4 4+ Ne
g
3+ A Ne
g
3+ β 3+ A (β)
RhD (+)
5 3+ 4+ 4+ AB Ne
g
Ne
g
0 4+ AB (Ø)
RhD (+)
ZK blood result showed that his blood contains O (α, β) RhD (+). Mild agglutination
was observed for A and A, B showing the presence of A and AB antigen. ZK blood also
contains RhD antigens. Sibling 1 (S1) have AB (Ø) RhD (-); hence agglutination was

5
IMMUNOLOGICAL ANALYSIS
observed got A, B and AB and RhD is absent. In the case of sibling 2, have A (β) RhD (+)
high robust agglutination was observed for A and AB and have RhD positive. Sibling 3 show
blood typing as O (α, β) RhD (+), as there was no agglutination for A, B and AB and the
typing is RhD positive. Sibling 4 blood typing result showed A (β) RhD (+) as there is robust
agglutination for both A and AB however there was no agglutination for B and RhD was
positive. Sibling 5 has no antibody, and agglutination was observed in both A, B and AB
antigens with RhD positive; therefore, the blood typing result is AB (Ø) RhD (+).
Discussion and conclusion
In the case of ZK, very mild agglutination was observed for A and AB but no
agglutination in case of B. As per the data, the blood group for ZK was O (α, β) RhD (+). It
might be due to human error or as his blood does not have any antigens that mild
agglutination observed, as ZK’s blood group is O (α, β) RhD (+), so it is assumed that his
blood would not have any antibody. Serum grouping was done, and agglutination reaction
was observed against α as well as for β that means both α, β antibodies are present (Belsito,
Magnussen and Napoli 2017). RhD analysis proved that RhD is present as there was an
agglutination reaction implying the presence of RhD antigens. Hence ZK has A (α, β) RhD
(+).
In the case of S1, A, B antigens are present; therefore, agglutinations were observed
for A, B and AB type. Therefore, it is predicted that S1 have AB blood group. Serum
grouping was done, and agglutination reaction was observed against α as well as for β
showing both α, β antibodies are showed no agglutination. It means α and β antibodies are
absent. RhD analysis proved that RhD is absent as there was no agglutination reaction
implying the presence of RhD antigens (Butt et al. 2018). Hence, S1 have AB (Ø) RhD (-). In
the case of S2, A antigens are present; therefore, agglutinations were observed for A, and AB
type; however, there was no agglutination for B antigen. Therefore, it is predicted that S2 has
A blood group. Serum grouping was done, and agglutination reaction was observed against α
as well as for β; α showed no agglutination, whereas β showed agglutination (Chen et al.
2016). It means α is absent and β antibody is present. RhD analysis proved that RhD is
present as there was an agglutination reaction implying the presence of RhD antigens. Hence,
S2 have A (β) RhD (+). S3 demonstrated the absence of antigen A, B, and AB as no
agglutination was observed. Agglutination was observed for both α, β and RhD reaction
showed positive agglutination. Therefore, the blood typing for S3 is O (α, β) RhD (+). S4
IMMUNOLOGICAL ANALYSIS
observed got A, B and AB and RhD is absent. In the case of sibling 2, have A (β) RhD (+)
high robust agglutination was observed for A and AB and have RhD positive. Sibling 3 show
blood typing as O (α, β) RhD (+), as there was no agglutination for A, B and AB and the
typing is RhD positive. Sibling 4 blood typing result showed A (β) RhD (+) as there is robust
agglutination for both A and AB however there was no agglutination for B and RhD was
positive. Sibling 5 has no antibody, and agglutination was observed in both A, B and AB
antigens with RhD positive; therefore, the blood typing result is AB (Ø) RhD (+).
Discussion and conclusion
In the case of ZK, very mild agglutination was observed for A and AB but no
agglutination in case of B. As per the data, the blood group for ZK was O (α, β) RhD (+). It
might be due to human error or as his blood does not have any antigens that mild
agglutination observed, as ZK’s blood group is O (α, β) RhD (+), so it is assumed that his
blood would not have any antibody. Serum grouping was done, and agglutination reaction
was observed against α as well as for β that means both α, β antibodies are present (Belsito,
Magnussen and Napoli 2017). RhD analysis proved that RhD is present as there was an
agglutination reaction implying the presence of RhD antigens. Hence ZK has A (α, β) RhD
(+).
In the case of S1, A, B antigens are present; therefore, agglutinations were observed
for A, B and AB type. Therefore, it is predicted that S1 have AB blood group. Serum
grouping was done, and agglutination reaction was observed against α as well as for β
showing both α, β antibodies are showed no agglutination. It means α and β antibodies are
absent. RhD analysis proved that RhD is absent as there was no agglutination reaction
implying the presence of RhD antigens (Butt et al. 2018). Hence, S1 have AB (Ø) RhD (-). In
the case of S2, A antigens are present; therefore, agglutinations were observed for A, and AB
type; however, there was no agglutination for B antigen. Therefore, it is predicted that S2 has
A blood group. Serum grouping was done, and agglutination reaction was observed against α
as well as for β; α showed no agglutination, whereas β showed agglutination (Chen et al.
2016). It means α is absent and β antibody is present. RhD analysis proved that RhD is
present as there was an agglutination reaction implying the presence of RhD antigens. Hence,
S2 have A (β) RhD (+). S3 demonstrated the absence of antigen A, B, and AB as no
agglutination was observed. Agglutination was observed for both α, β and RhD reaction
showed positive agglutination. Therefore, the blood typing for S3 is O (α, β) RhD (+). S4
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

6
IMMUNOLOGICAL ANALYSIS
showed a positive agglutination reaction for antigen A and AB; however, B antigen showed
no coagulation. In the case of antibody, α negative reaction is shown, but β antibody showed
positive agglutination reaction (Cooling 2015). RhD analysis showed agglutination stating
that the type of blood for S4 is A (β) RhD (+). S5 have shown positive reaction for all A, B
and AB antigens; however, both the antibody showed a negative reaction in case of
agglutination. Even the RhD showed agglutination. Hence, the blood type for S5 is AB (Ø)
RhD (+).
Tube technique used helped in successful analysis of the identification of blood type,
yet this technique has some limitations as it is time-taking and antibody reagents can be
costly (Cozzi et al. 2017). Limitations for this experiment consists of human error such
wrong volume or adding samples/ reagents in wrong test tubes. This might give wrong
agglutination result. Reading of the agglutination score is subjective as it might vary from
person to person. It is confirmed that ZK’s kidney transplantation is possible only with
Sibling 2 and 3 (Selleng et al. 2017). The purpose of this experiment was fulfilled
successfully for ZK as well as for his siblings by the use of tube technique. This technique is
used as a substitute process for tube technique.
IMMUNOLOGICAL ANALYSIS
showed a positive agglutination reaction for antigen A and AB; however, B antigen showed
no coagulation. In the case of antibody, α negative reaction is shown, but β antibody showed
positive agglutination reaction (Cooling 2015). RhD analysis showed agglutination stating
that the type of blood for S4 is A (β) RhD (+). S5 have shown positive reaction for all A, B
and AB antigens; however, both the antibody showed a negative reaction in case of
agglutination. Even the RhD showed agglutination. Hence, the blood type for S5 is AB (Ø)
RhD (+).
Tube technique used helped in successful analysis of the identification of blood type,
yet this technique has some limitations as it is time-taking and antibody reagents can be
costly (Cozzi et al. 2017). Limitations for this experiment consists of human error such
wrong volume or adding samples/ reagents in wrong test tubes. This might give wrong
agglutination result. Reading of the agglutination score is subjective as it might vary from
person to person. It is confirmed that ZK’s kidney transplantation is possible only with
Sibling 2 and 3 (Selleng et al. 2017). The purpose of this experiment was fulfilled
successfully for ZK as well as for his siblings by the use of tube technique. This technique is
used as a substitute process for tube technique.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser
7
IMMUNOLOGICAL ANALYSIS
Interpretation
First answer
Sibling 3 is a full match with ZK blood group. ‘O’ is the universal donor and RhD
antigens and α, β serum antibodies are present for both ZK and sibling 3. On other, hand both
their blood groups match as they share blood group O (α, β) RhD (+). Hence, sibling 3 is
suitable for kidney transplantation with ZK.
Second answer
Patient
Blood Donor blood type
ZK
blood
type
Sibling 1 Sibling 2 Sibling 3 Sibling 4 Sibling 5
O (α, β)
RhD
(+)
AB (Ø) RhD
(-) A (β) RhD (+) O (α, β) RhD
(+) A (β) RhD (+) AB (Ø) RhD
(+)
Positive Positive Negative Positive Positive
Transplantation
not possible
Transplantation
not possible
Transplantatio
n possible
Transplantation
not possible
Transplantation
not possible
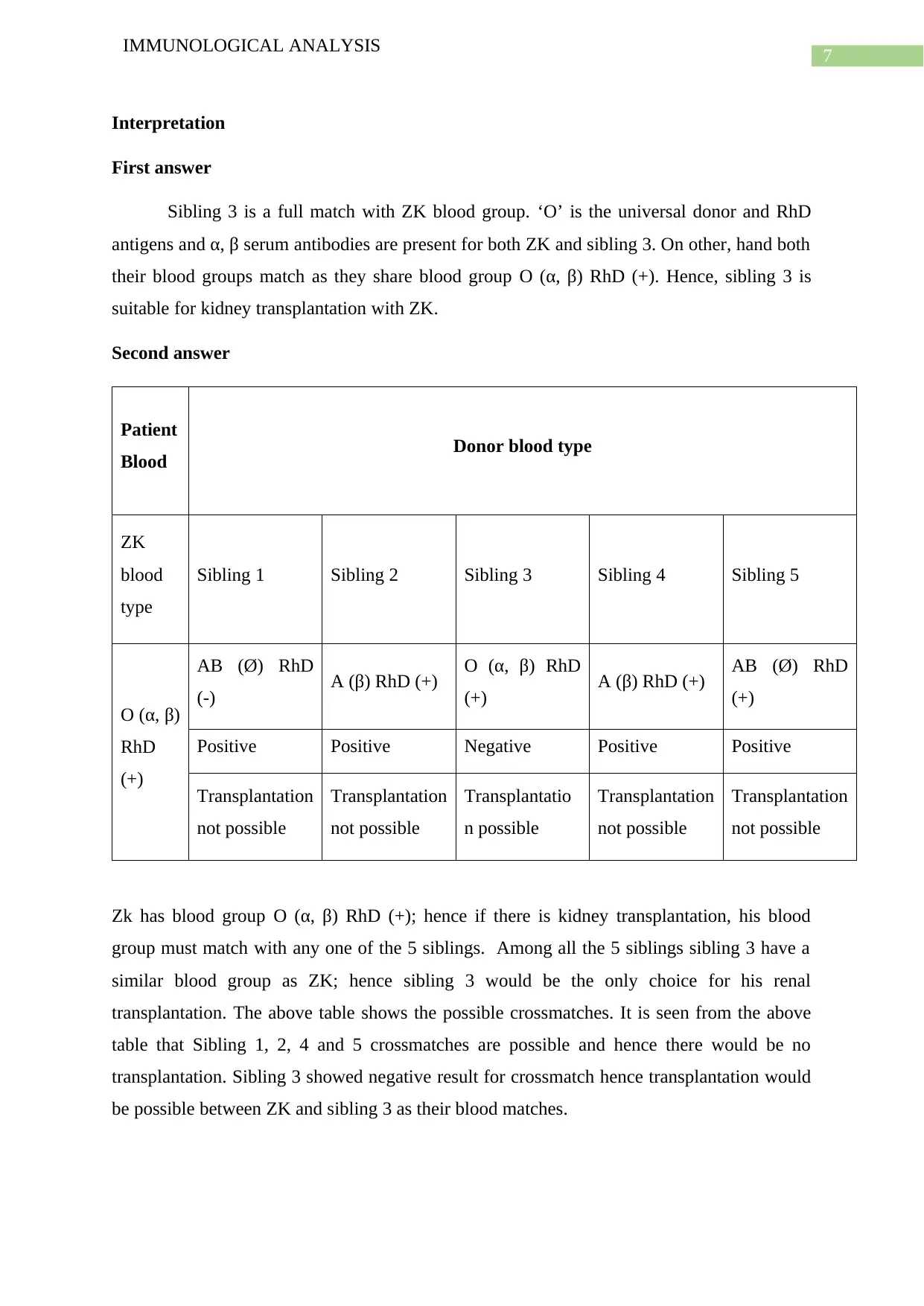
Zk has blood group O (α, β) RhD (+); hence if there is kidney transplantation, his blood
group must match with any one of the 5 siblings. Among all the 5 siblings sibling 3 have a
similar blood group as ZK; hence sibling 3 would be the only choice for his renal
transplantation. The above table shows the possible crossmatches. It is seen from the above
table that Sibling 1, 2, 4 and 5 crossmatches are possible and hence there would be no
transplantation. Sibling 3 showed negative result for crossmatch hence transplantation would
be possible between ZK and sibling 3 as their blood matches.
IMMUNOLOGICAL ANALYSIS
Interpretation
First answer
Sibling 3 is a full match with ZK blood group. ‘O’ is the universal donor and RhD
antigens and α, β serum antibodies are present for both ZK and sibling 3. On other, hand both
their blood groups match as they share blood group O (α, β) RhD (+). Hence, sibling 3 is
suitable for kidney transplantation with ZK.
Second answer
Patient
Blood Donor blood type
ZK
blood
type
Sibling 1 Sibling 2 Sibling 3 Sibling 4 Sibling 5
O (α, β)
RhD
(+)
AB (Ø) RhD
(-) A (β) RhD (+) O (α, β) RhD
(+) A (β) RhD (+) AB (Ø) RhD
(+)
Positive Positive Negative Positive Positive
Transplantation
not possible
Transplantation
not possible
Transplantatio
n possible
Transplantation
not possible
Transplantation
not possible
Zk has blood group O (α, β) RhD (+); hence if there is kidney transplantation, his blood
group must match with any one of the 5 siblings. Among all the 5 siblings sibling 3 have a
similar blood group as ZK; hence sibling 3 would be the only choice for his renal
transplantation. The above table shows the possible crossmatches. It is seen from the above
table that Sibling 1, 2, 4 and 5 crossmatches are possible and hence there would be no
transplantation. Sibling 3 showed negative result for crossmatch hence transplantation would
be possible between ZK and sibling 3 as their blood matches.

8
IMMUNOLOGICAL ANALYSIS
Third answer
Parent 1
Possible genotype for the parent: AB
The possible phenotype of the parent: AB
Parent 2
The possible genotype of parent: AA, AO
The possible phenotype of the parent: A
In case ZK and his 5 siblings the blood group observed are A, AB and O. Hence, it is
assumed that their parents would have A and AB blood group. Hence the blood group for
kids would be A, AB, O and A. The offspring would receive one from father and one from
mother.
Fourth answer
Blood transfusions among incompatible blood groups such as A, B, O and AB can
cause an immune response. It causes a serious transfusion response. The immune system
would attack the blood cells that are donated, as it is incompatible causing them to rupture.
Blood must be screened properly before transfusion. ABO-incompatible transfusion causes
acute haemolytic transfusion reaction (AHTR) develops, destroying intravascular RBCs
through a reaction between antigen and antibody of donor antigens and recipients prevailing
antibodies. The antigen-antibody reaction causes haemolysis (Lowe 2019). This is life-
threatening when RBC agglutinates it might lead to stroke. Cytokine causes the issue of IL-1,
AB A
A AB O A
IMMUNOLOGICAL ANALYSIS
Third answer
Parent 1
Possible genotype for the parent: AB
The possible phenotype of the parent: AB
Parent 2
The possible genotype of parent: AA, AO
The possible phenotype of the parent: A
In case ZK and his 5 siblings the blood group observed are A, AB and O. Hence, it is
assumed that their parents would have A and AB blood group. Hence the blood group for
kids would be A, AB, O and A. The offspring would receive one from father and one from
mother.
Fourth answer
Blood transfusions among incompatible blood groups such as A, B, O and AB can
cause an immune response. It causes a serious transfusion response. The immune system
would attack the blood cells that are donated, as it is incompatible causing them to rupture.
Blood must be screened properly before transfusion. ABO-incompatible transfusion causes
acute haemolytic transfusion reaction (AHTR) develops, destroying intravascular RBCs
through a reaction between antigen and antibody of donor antigens and recipients prevailing
antibodies. The antigen-antibody reaction causes haemolysis (Lowe 2019). This is life-
threatening when RBC agglutinates it might lead to stroke. Cytokine causes the issue of IL-1,
AB A
A AB O A
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

9
IMMUNOLOGICAL ANALYSIS
IL_6 and TNF enhancing RBC haemolysis leading to hypotension and fever as well as
activation of neutrophil and endothelial damage (Meo et al. 2016). ABO incompatibility
causes reactions after a few days of transfusion. If incompatible blood is transfused, then the
initial symptoms include chills and fever. Due to incompatible transfusion haemolytic
transfusion reaction occurs that causes some serious complications. It leads to some allergic
reactions inside the body and starts destroying the blood cells causing destruction of the
immune system in the body of the individual (Alemu and Mama 2016).
Therefore, from the above interpretation, it can be concluded that transplantations can
only be possible with similar blood groups and only between genetically linked individual
such as parents or siblings. ZK suffering from renal disorder is required to undergo renal
transplantation, and sibling 3 would be his only choice in the process.
IMMUNOLOGICAL ANALYSIS
IL_6 and TNF enhancing RBC haemolysis leading to hypotension and fever as well as
activation of neutrophil and endothelial damage (Meo et al. 2016). ABO incompatibility
causes reactions after a few days of transfusion. If incompatible blood is transfused, then the
initial symptoms include chills and fever. Due to incompatible transfusion haemolytic
transfusion reaction occurs that causes some serious complications. It leads to some allergic
reactions inside the body and starts destroying the blood cells causing destruction of the
immune system in the body of the individual (Alemu and Mama 2016).
Therefore, from the above interpretation, it can be concluded that transplantations can
only be possible with similar blood groups and only between genetically linked individual
such as parents or siblings. ZK suffering from renal disorder is required to undergo renal
transplantation, and sibling 3 would be his only choice in the process.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

10
IMMUNOLOGICAL ANALYSIS
References
Albánez, S., Ogiwara, K., Michels, A., Hopman, W., Grabell, J., James, P. and Lillicrap, D.,
2016. Aging and ABO blood type influence von Willebrand factor and factor VIII levels
through interrelated mechanisms. Journal of Thrombosis and Haemostasis, 14(5), pp.953-
963.
Alemu, G. and Mama, M., 2016. Assessing ABO/Rh blood group frequency and association
with asymptomatic malaria among blood donors attending Arba Minch blood bank, South
Ethiopia. Malaria research and treatment, 2016.
Belsito, A., Magnussen, K. and Napoli, C., 2017. Emerging strategies of blood group
genotyping for patients with hemoglobinopathies. Transfusion and Apheresis Science, 56(2),
pp.206-213.
Butt, S.J., Malik, S., Malik, H. and Butt, A.J., 2018. ABO and Rhesus Blood Grouping in
Voluntary Blood Donors and its gender association. Pak J Med Health Sci, 12(1), pp.268-
271.
Chen, Z., Yang, S.H., Xu, H. and Li, J.J., 2016. ABO blood group system and the coronary
artery disease: an updated systematic review and meta-analysis. Scientific reports, 6(1), pp.1-
11.
Cooling, L., 2015. Blood groups in infection and host susceptibility. Clinical microbiology
reviews, 28(3), pp.801-870.
Cozzi, G.D., Levinson, R.T., Toole, H., Snyder, M.R., Deng, A., Crispens, M.A., Khabele, D.
and Beeghly-Fadiel, A., 2017. Blood type, ABO genetic variants, and ovarian cancer
survival. PloS one, 12(4).
Lowe, G.D. ed., 2019. Clinical blood rheology (Vol. 2). Crc Press.
Meo, S.A., Rouq, F.A., Suraya, F. and Zaidi, S.Z., 2016. Association of ABO and Rh blood
groups with type 2 diabetes mellitus. Eur Rev Med Pharmacol Sci, 20(2), pp.237-42.
Selleng, K., Jenichen, G., Denker, K., Selleng, S., Müllejans, B. and Greinacher, A., 2017.
Emergency transfusion of patients with unknown blood type with blood group O Rhesus D
positive red blood cell concentrates: a prospective, single-centre, observational study. The
Lancet Haematology, 4(5), pp.e218-e224.
IMMUNOLOGICAL ANALYSIS
References
Albánez, S., Ogiwara, K., Michels, A., Hopman, W., Grabell, J., James, P. and Lillicrap, D.,
2016. Aging and ABO blood type influence von Willebrand factor and factor VIII levels
through interrelated mechanisms. Journal of Thrombosis and Haemostasis, 14(5), pp.953-
963.
Alemu, G. and Mama, M., 2016. Assessing ABO/Rh blood group frequency and association
with asymptomatic malaria among blood donors attending Arba Minch blood bank, South
Ethiopia. Malaria research and treatment, 2016.
Belsito, A., Magnussen, K. and Napoli, C., 2017. Emerging strategies of blood group
genotyping for patients with hemoglobinopathies. Transfusion and Apheresis Science, 56(2),
pp.206-213.
Butt, S.J., Malik, S., Malik, H. and Butt, A.J., 2018. ABO and Rhesus Blood Grouping in
Voluntary Blood Donors and its gender association. Pak J Med Health Sci, 12(1), pp.268-
271.
Chen, Z., Yang, S.H., Xu, H. and Li, J.J., 2016. ABO blood group system and the coronary
artery disease: an updated systematic review and meta-analysis. Scientific reports, 6(1), pp.1-
11.
Cooling, L., 2015. Blood groups in infection and host susceptibility. Clinical microbiology
reviews, 28(3), pp.801-870.
Cozzi, G.D., Levinson, R.T., Toole, H., Snyder, M.R., Deng, A., Crispens, M.A., Khabele, D.
and Beeghly-Fadiel, A., 2017. Blood type, ABO genetic variants, and ovarian cancer
survival. PloS one, 12(4).
Lowe, G.D. ed., 2019. Clinical blood rheology (Vol. 2). Crc Press.
Meo, S.A., Rouq, F.A., Suraya, F. and Zaidi, S.Z., 2016. Association of ABO and Rh blood
groups with type 2 diabetes mellitus. Eur Rev Med Pharmacol Sci, 20(2), pp.237-42.
Selleng, K., Jenichen, G., Denker, K., Selleng, S., Müllejans, B. and Greinacher, A., 2017.
Emergency transfusion of patients with unknown blood type with blood group O Rhesus D
positive red blood cell concentrates: a prospective, single-centre, observational study. The
Lancet Haematology, 4(5), pp.e218-e224.
1 out of 11
Your All-in-One AI-Powered Toolkit for Academic Success.
+13062052269
info@desklib.com
Available 24*7 on WhatsApp / Email
![[object Object]](/_next/static/media/star-bottom.7253800d.svg)
Unlock your academic potential
Copyright © 2020–2026 A2Z Services. All Rights Reserved. Developed and managed by ZUCOL.
