Cardiac Nursing Report: Analysis of Modules 1-4 Content
VerifiedAdded on 2022/09/28
|11
|2592
|40
Report
AI Summary
This report provides an overview of cardiac nursing, encompassing four modules. Module 1 details the anatomy and physiology of the human heart, including its chambers, blood vessels, and valves. Module 2 examines various antiarrhythmic drug classes, their mechanisms of action, side effects, and indications for use. Module 3 focuses on transcutaneous pacing, outlining its indications, contraindications, nursing precautions, and potential complications. Module 4 discusses hypovolemic shock, its causes, symptoms, and nursing care services. The report integrates relevant references to support the information and provide a comprehensive understanding of key cardiac nursing concepts.

1
Running Head: Cardiac Nursing
Cardiac Nursing
Name
Institutional Affiliation
Running Head: Cardiac Nursing
Cardiac Nursing
Name
Institutional Affiliation
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

2
Cardiac Nursing
CARDIAC NURSING
URL Link
https://vucollaborate.vu.edu.au/d2l/eP/presentations/presentation_preview_popup.d2l?
presId=1291026
Module 1
The human heart is an organ within the body that pumps blood throughout the body and
this ensures that there is enough oxygen supply and nutrients to the body tissues. Moreover, it is
essential in doing away with carbon dioxide and other waste within the body. The human heart
has four chambers and these include the two upper chambers and the two lower chambers. The
human heart consist of specific blood vessels. The blood vessels include the arteries which are
known to carry blood which is oxygenated from the heart to the body tissues. The heart is made
up of several capillaries that are known to be within the blood vessels considered to be thin and
are responsible for making connection between the arteries and the veins. Moreover, they have
thin walls that enable them to allow movement of nutrients, oxygen, and carbon dioxide together
with the other wastes that exist within our organ cells (Willis, 2016).
Furthermore, veins are also found in the human heart, and they are responsible for taking
the blood back to the heart, and the blood is known to have low oxygen content. They contain the
waste products that are supposed to be removed from the body. The heart contains a superior
vena cava that transports blood from the head or even the arms to the heart. The heart various
muscles, especially at the on the walls of the heart. The strong muscular walls of the heart are
known to contract to allow blood to be pumped to the rest of the organs within the body. There
are coronary arteries that are responsible for providing blood rich in oxygen to the heart muscle.
Cardiac Nursing
CARDIAC NURSING
URL Link
https://vucollaborate.vu.edu.au/d2l/eP/presentations/presentation_preview_popup.d2l?
presId=1291026
Module 1
The human heart is an organ within the body that pumps blood throughout the body and
this ensures that there is enough oxygen supply and nutrients to the body tissues. Moreover, it is
essential in doing away with carbon dioxide and other waste within the body. The human heart
has four chambers and these include the two upper chambers and the two lower chambers. The
human heart consist of specific blood vessels. The blood vessels include the arteries which are
known to carry blood which is oxygenated from the heart to the body tissues. The heart is made
up of several capillaries that are known to be within the blood vessels considered to be thin and
are responsible for making connection between the arteries and the veins. Moreover, they have
thin walls that enable them to allow movement of nutrients, oxygen, and carbon dioxide together
with the other wastes that exist within our organ cells (Willis, 2016).
Furthermore, veins are also found in the human heart, and they are responsible for taking
the blood back to the heart, and the blood is known to have low oxygen content. They contain the
waste products that are supposed to be removed from the body. The heart contains a superior
vena cava that transports blood from the head or even the arms to the heart. The heart various
muscles, especially at the on the walls of the heart. The strong muscular walls of the heart are
known to contract to allow blood to be pumped to the rest of the organs within the body. There
are coronary arteries that are responsible for providing blood rich in oxygen to the heart muscle.

3
Cardiac Nursing
Furthermore, the heart is known to be four-chambered, whereby it is dived into the left
and even the right side using the muscular wall known as the septum. Moreover, this is according
to "The Works of William Harvey" in the topic "The heart and soul of change". Furthermore,
both sides are further divided into two chambers. The top chamber is known as the atria, which is
responsible for receiving the blood that comes from the veins (Hubble, 2016). The bottom
chambers are known as the ventricles, and they are responsible for pumping blood to the arteries.
Furthermore, both the chambers are known to work together by contracting and even relaxing to
pump blood out of the heart. Moreover, the heart is made up of four valves, including the
tricuspid valve, pulmonic valve, Mitral valve and the Aortic valve.
Blood goes ahead to move from the right atrium straight to the right ventricle, and this
takes place through the tricuspid valve. The tricuspid valve closes when the ventricle gets
occupied. When the ventricle contracts, the blood is transported to the pulmonary artery before
going to the lungs using the pulmonic valve. Moreover, the blood is oxygenated before being
transported back to the left atrium as it passes through the pulmonary veins. Blood flows to the
left ventricle by the time the atrium contracts. When the ventricle contracts, the blood moves
from the heart straight to the body.
Module 2
Cardiac Nursing
Furthermore, the heart is known to be four-chambered, whereby it is dived into the left
and even the right side using the muscular wall known as the septum. Moreover, this is according
to "The Works of William Harvey" in the topic "The heart and soul of change". Furthermore,
both sides are further divided into two chambers. The top chamber is known as the atria, which is
responsible for receiving the blood that comes from the veins (Hubble, 2016). The bottom
chambers are known as the ventricles, and they are responsible for pumping blood to the arteries.
Furthermore, both the chambers are known to work together by contracting and even relaxing to
pump blood out of the heart. Moreover, the heart is made up of four valves, including the
tricuspid valve, pulmonic valve, Mitral valve and the Aortic valve.
Blood goes ahead to move from the right atrium straight to the right ventricle, and this
takes place through the tricuspid valve. The tricuspid valve closes when the ventricle gets
occupied. When the ventricle contracts, the blood is transported to the pulmonary artery before
going to the lungs using the pulmonic valve. Moreover, the blood is oxygenated before being
transported back to the left atrium as it passes through the pulmonary veins. Blood flows to the
left ventricle by the time the atrium contracts. When the ventricle contracts, the blood moves
from the heart straight to the body.
Module 2
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide
4
Cardiac Nursing
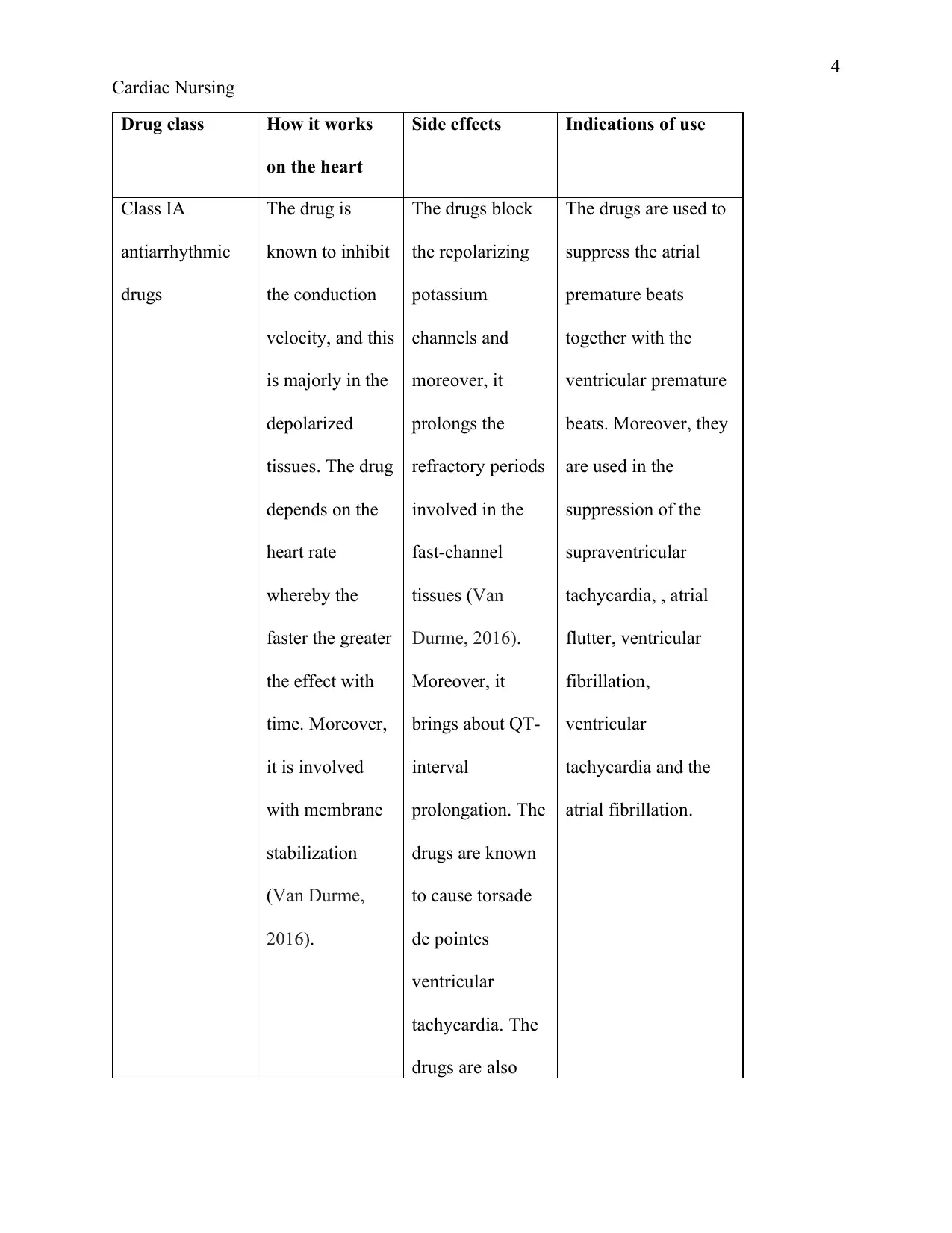
Drug class How it works
on the heart
Side effects Indications of use
Class IA
antiarrhythmic
drugs
The drug is
known to inhibit
the conduction
velocity, and this
is majorly in the
depolarized
tissues. The drug
depends on the
heart rate
whereby the
faster the greater
the effect with
time. Moreover,
it is involved
with membrane
stabilization
(Van Durme,
2016).
The drugs block
the repolarizing
potassium
channels and
moreover, it
prolongs the
refractory periods
involved in the
fast-channel
tissues (Van
Durme, 2016).
Moreover, it
brings about QT-
interval
prolongation. The
drugs are known
to cause torsade
de pointes
ventricular
tachycardia. The
drugs are also
The drugs are used to
suppress the atrial
premature beats
together with the
ventricular premature
beats. Moreover, they
are used in the
suppression of the
supraventricular
tachycardia, , atrial
flutter, ventricular
fibrillation,
ventricular
tachycardia and the
atrial fibrillation.
Cardiac Nursing
Drug class How it works
on the heart
Side effects Indications of use
Class IA
antiarrhythmic
drugs
The drug is
known to inhibit
the conduction
velocity, and this
is majorly in the
depolarized
tissues. The drug
depends on the
heart rate
whereby the
faster the greater
the effect with
time. Moreover,
it is involved
with membrane
stabilization
(Van Durme,
2016).
The drugs block
the repolarizing
potassium
channels and
moreover, it
prolongs the
refractory periods
involved in the
fast-channel
tissues (Van
Durme, 2016).
Moreover, it
brings about QT-
interval
prolongation. The
drugs are known
to cause torsade
de pointes
ventricular
tachycardia. The
drugs are also
The drugs are used to
suppress the atrial
premature beats
together with the
ventricular premature
beats. Moreover, they
are used in the
suppression of the
supraventricular
tachycardia, , atrial
flutter, ventricular
fibrillation,
ventricular
tachycardia and the
atrial fibrillation.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser
5
Cardiac Nursing
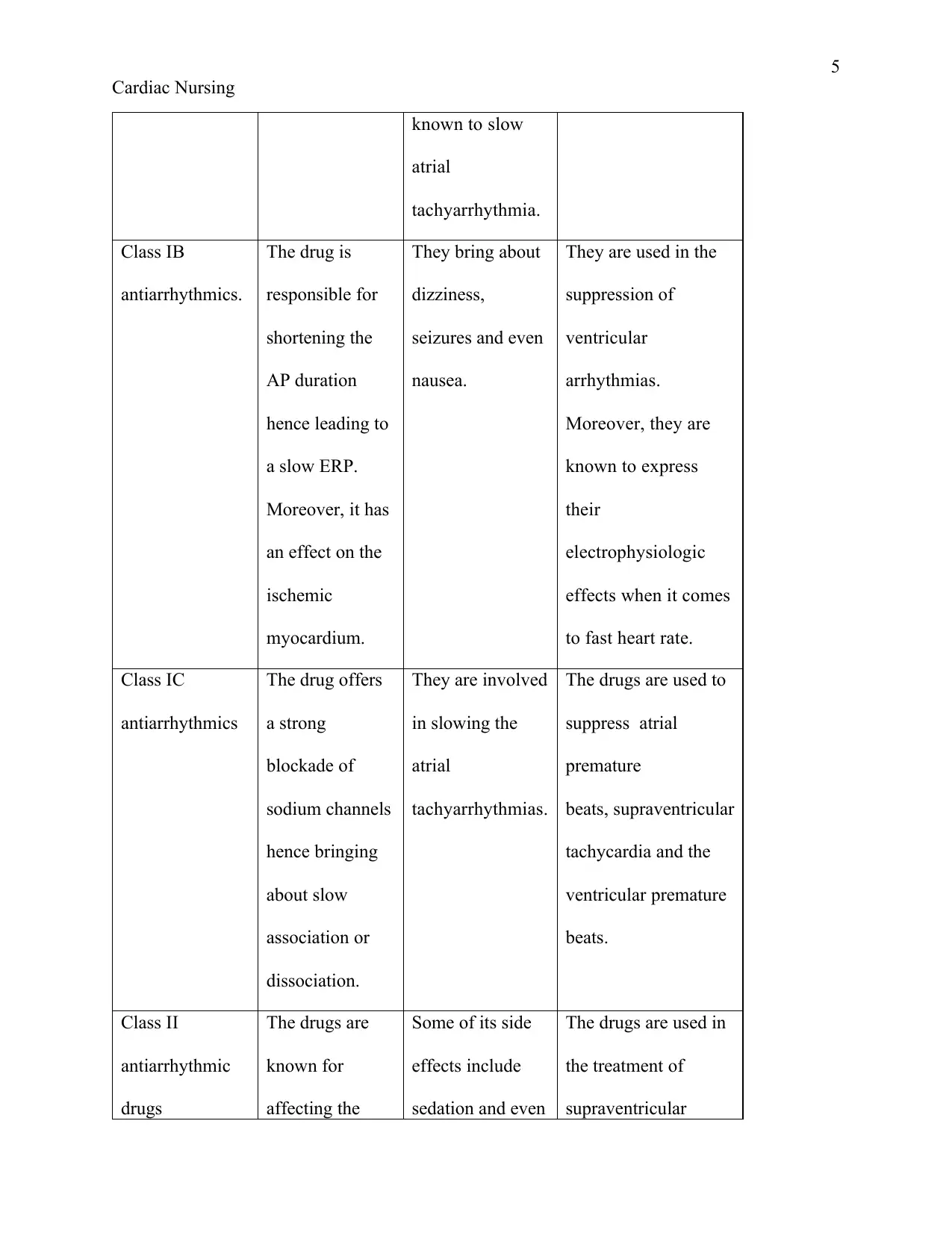
known to slow
atrial
tachyarrhythmia.
Class IB
antiarrhythmics.
The drug is
responsible for
shortening the
AP duration
hence leading to
a slow ERP.
Moreover, it has
an effect on the
ischemic
myocardium.
They bring about
dizziness,
seizures and even
nausea.
They are used in the
suppression of
ventricular
arrhythmias.
Moreover, they are
known to express
their
electrophysiologic
effects when it comes
to fast heart rate.
Class IC
antiarrhythmics
The drug offers
a strong
blockade of
sodium channels
hence bringing
about slow
association or
dissociation.
They are involved
in slowing the
atrial
tachyarrhythmias.
The drugs are used to
suppress atrial
premature
beats, supraventricular
tachycardia and the
ventricular premature
beats.
Class II
antiarrhythmic
drugs
The drugs are
known for
affecting the
Some of its side
effects include
sedation and even
The drugs are used in
the treatment of
supraventricular
Cardiac Nursing
known to slow
atrial
tachyarrhythmia.
Class IB
antiarrhythmics.
The drug is
responsible for
shortening the
AP duration
hence leading to
a slow ERP.
Moreover, it has
an effect on the
ischemic
myocardium.
They bring about
dizziness,
seizures and even
nausea.
They are used in the
suppression of
ventricular
arrhythmias.
Moreover, they are
known to express
their
electrophysiologic
effects when it comes
to fast heart rate.
Class IC
antiarrhythmics
The drug offers
a strong
blockade of
sodium channels
hence bringing
about slow
association or
dissociation.
They are involved
in slowing the
atrial
tachyarrhythmias.
The drugs are used to
suppress atrial
premature
beats, supraventricular
tachycardia and the
ventricular premature
beats.
Class II
antiarrhythmic
drugs
The drugs are
known for
affecting the
Some of its side
effects include
sedation and even
The drugs are used in
the treatment of
supraventricular
6
Cardiac Nursing
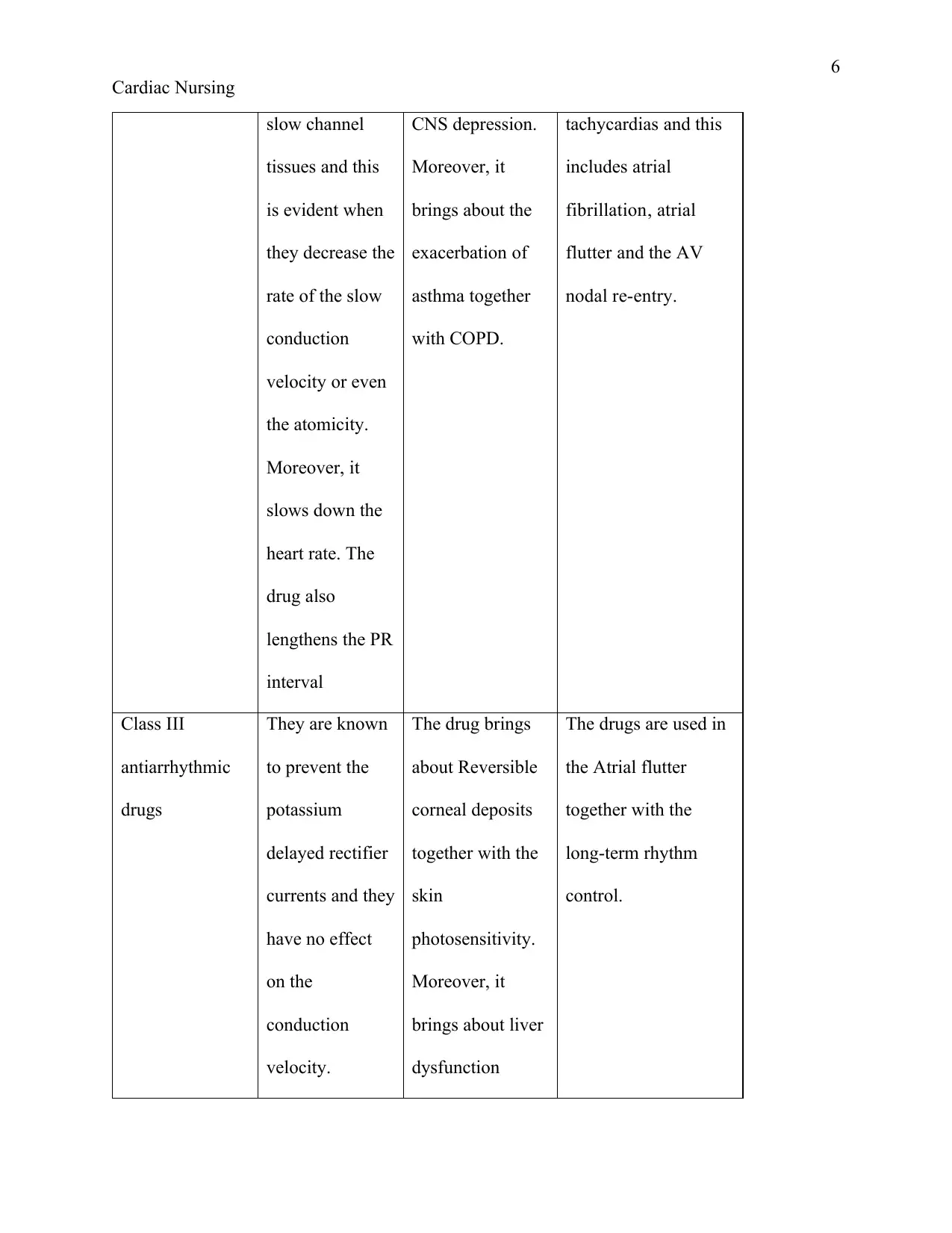
slow channel
tissues and this
is evident when
they decrease the
rate of the slow
conduction
velocity or even
the atomicity.
Moreover, it
slows down the
heart rate. The
drug also
lengthens the PR
interval
CNS depression.
Moreover, it
brings about the
exacerbation of
asthma together
with COPD.
tachycardias and this
includes atrial
fibrillation, atrial
flutter and the AV
nodal re-entry.
Class III
antiarrhythmic
drugs
They are known
to prevent the
potassium
delayed rectifier
currents and they
have no effect
on the
conduction
velocity.
The drug brings
about Reversible
corneal deposits
together with the
skin
photosensitivity.
Moreover, it
brings about liver
dysfunction
The drugs are used in
the Atrial flutter
together with the
long-term rhythm
control.
Cardiac Nursing
slow channel
tissues and this
is evident when
they decrease the
rate of the slow
conduction
velocity or even
the atomicity.
Moreover, it
slows down the
heart rate. The
drug also
lengthens the PR
interval
CNS depression.
Moreover, it
brings about the
exacerbation of
asthma together
with COPD.
tachycardias and this
includes atrial
fibrillation, atrial
flutter and the AV
nodal re-entry.
Class III
antiarrhythmic
drugs
They are known
to prevent the
potassium
delayed rectifier
currents and they
have no effect
on the
conduction
velocity.
The drug brings
about Reversible
corneal deposits
together with the
skin
photosensitivity.
Moreover, it
brings about liver
dysfunction
The drugs are used in
the Atrial flutter
together with the
long-term rhythm
control.
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide
7
Cardiac Nursing
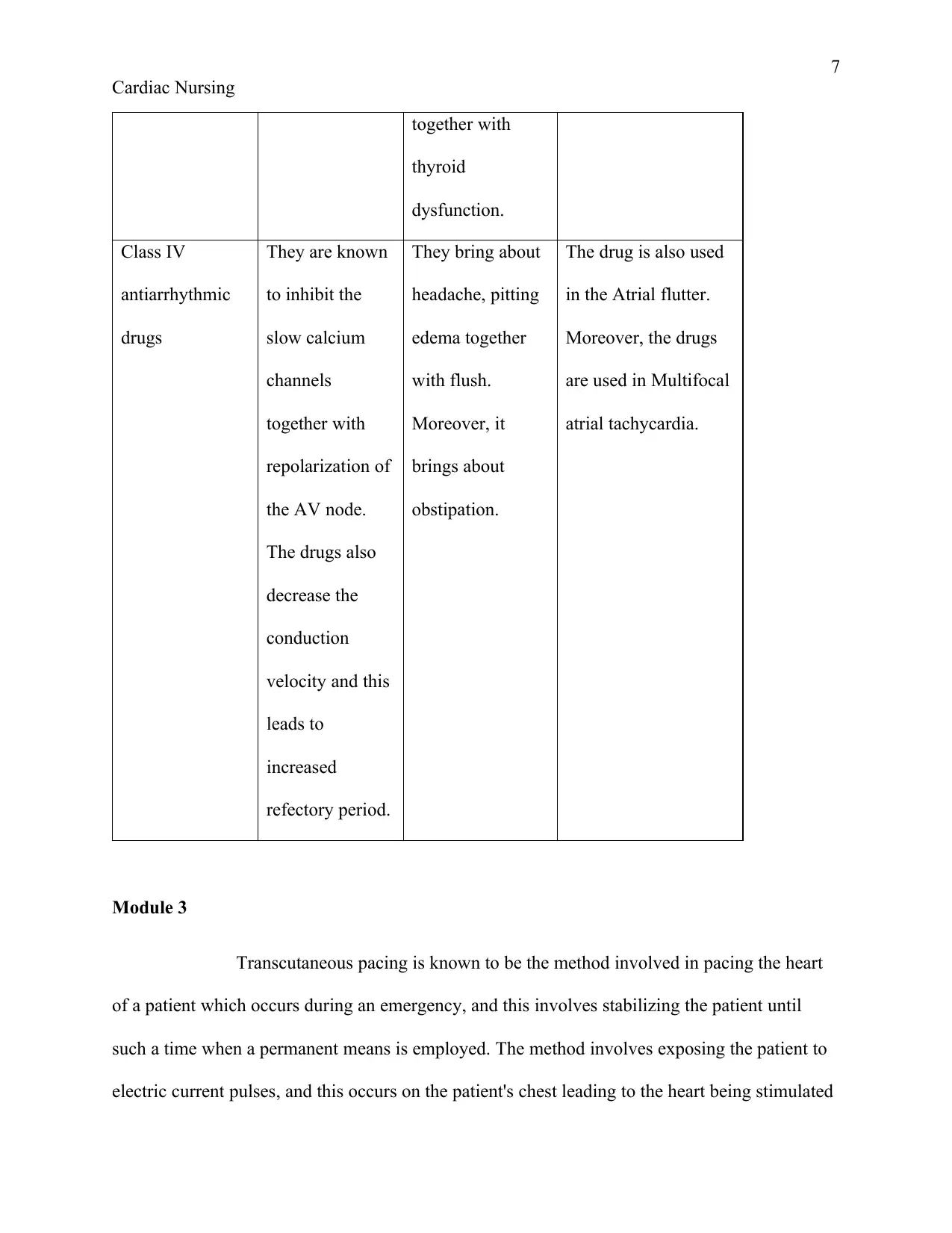
together with
thyroid
dysfunction.
Class IV
antiarrhythmic
drugs
They are known
to inhibit the
slow calcium
channels
together with
repolarization of
the AV node.
The drugs also
decrease the
conduction
velocity and this
leads to
increased
refectory period.
They bring about
headache, pitting
edema together
with flush.
Moreover, it
brings about
obstipation.
The drug is also used
in the Atrial flutter.
Moreover, the drugs
are used in Multifocal
atrial tachycardia.
Module 3
Transcutaneous pacing is known to be the method involved in pacing the heart
of a patient which occurs during an emergency, and this involves stabilizing the patient until
such a time when a permanent means is employed. The method involves exposing the patient to
electric current pulses, and this occurs on the patient's chest leading to the heart being stimulated
Cardiac Nursing
together with
thyroid
dysfunction.
Class IV
antiarrhythmic
drugs
They are known
to inhibit the
slow calcium
channels
together with
repolarization of
the AV node.
The drugs also
decrease the
conduction
velocity and this
leads to
increased
refectory period.
They bring about
headache, pitting
edema together
with flush.
Moreover, it
brings about
obstipation.
The drug is also used
in the Atrial flutter.
Moreover, the drugs
are used in Multifocal
atrial tachycardia.
Module 3
Transcutaneous pacing is known to be the method involved in pacing the heart
of a patient which occurs during an emergency, and this involves stabilizing the patient until
such a time when a permanent means is employed. The method involves exposing the patient to
electric current pulses, and this occurs on the patient's chest leading to the heart being stimulated
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

8
Cardiac Nursing
to contract. Some of the common indications when it comes to transcutaneous pacing include the
unstable bradycardias that are considered hemodynamical, and they are known to be
unresponsive when it comes to atropine. Moreover, cardiac arrest is another indicator, especially
when it comes to being bradycardia, and this occurs when it is used early. Other possible
indicators include the electrical activity that is known to be pulseless, and this happens due to the
occurrence of an overdose or even acidosis. Moreover, some of the contraindications when it
comes to TCD include severe hypothermia together with a prolonging bradyasystolic cardiac
arrest.
Some of the most crucial precautions that the nurses should put into
consideration include explaining the purpose of the TCP to the patient, and this involves telling
him or her about the discomfort that comes with it together with the need for medication. After
the whole exercise, the nurse will be in a position to go ahead and expose his chest before
positioning the electrodes on clean and even dry skin before setting the pacing current output
(Arnsdorf, 2016). There is a need for the nurse to keep an eye the heart rate of the patient and
even rhythm and even to assess the patient's response to pacing. Moreover, this is essential to
avoid the risk that might come across due to the use of the TCP on the patient. The nurse needs
to keep an eye on the pacing of the device. The nurse should be able to assess the hemodynamic
response of the patient when it comes to pacing, and this involves evaluating his or her central
pulses. There is a need for the nurse to monitor the patient's pain before administering the
patient's analgesia due to the lack to ease the chest wall muscle contractions.
Some of the critical occurrences that might occur in the process include pacing
threshold changing without any warning, and this may lead to the capture being lost. Moreover,
under sensing may occur whereby the pacemaker does not detect the intrinsic activity, and this
Cardiac Nursing
to contract. Some of the common indications when it comes to transcutaneous pacing include the
unstable bradycardias that are considered hemodynamical, and they are known to be
unresponsive when it comes to atropine. Moreover, cardiac arrest is another indicator, especially
when it comes to being bradycardia, and this occurs when it is used early. Other possible
indicators include the electrical activity that is known to be pulseless, and this happens due to the
occurrence of an overdose or even acidosis. Moreover, some of the contraindications when it
comes to TCD include severe hypothermia together with a prolonging bradyasystolic cardiac
arrest.
Some of the most crucial precautions that the nurses should put into
consideration include explaining the purpose of the TCP to the patient, and this involves telling
him or her about the discomfort that comes with it together with the need for medication. After
the whole exercise, the nurse will be in a position to go ahead and expose his chest before
positioning the electrodes on clean and even dry skin before setting the pacing current output
(Arnsdorf, 2016). There is a need for the nurse to keep an eye the heart rate of the patient and
even rhythm and even to assess the patient's response to pacing. Moreover, this is essential to
avoid the risk that might come across due to the use of the TCP on the patient. The nurse needs
to keep an eye on the pacing of the device. The nurse should be able to assess the hemodynamic
response of the patient when it comes to pacing, and this involves evaluating his or her central
pulses. There is a need for the nurse to monitor the patient's pain before administering the
patient's analgesia due to the lack to ease the chest wall muscle contractions.
Some of the critical occurrences that might occur in the process include pacing
threshold changing without any warning, and this may lead to the capture being lost. Moreover,
under sensing may occur whereby the pacemaker does not detect the intrinsic activity, and this

9
Cardiac Nursing
may lead to him or her delivering a pace pulse (Lerman, 2016). There is a need to be keen on
ensuring that the electric current is increased as much as possible to ensure electric capture takes
place in the best way possible. These are essential when it comes to reducing the risks that come
with the transcutaneous pacing. Furthermore, this is according to "Emergency department use of
transcutaneous pacing for cardiac arrests" in the topic "Critical care medicine".
Module 4
Hypovolemic shock occurs when an individual loses more than twenty per cent
of his or her body's blood or even the fluid supply. Moreover, this situation makes it hard for the
heart to push enough blood to the organs, and this may lead to organ failure. The condition
always needs immediate medical attention. Some of its causes include bleeding that occurs due
to severe cuts or even wounds, and this leads to blood loss within the body. Moreover, there is
internal bleeding from the various abdominal organs, or there might be cases whereby the
ectopic pregnancy ruptures, leading to blood loss within the body. Furthermore, the shock can be
brought about by bleeding caused by the blunt traumatic injuries that occur due to injuries.
Bleeding that arises from the digestive tract can lead to higher chances of blood loss within the
body hence putting one's body at risk.
Virginal bleeding among the female can be a leading cause in some women, and
this has proven to be risky in most situations due to the massive amount of blood that someone
might lose in the process. The blood volume can be affected by the loss of body fluids. Excessive
sweating and even excessive vomiting can affect the fluid level in the body hence affecting the
blood volume at the end of the day, and this may lead to one developing the shock. Moreover,
some of the symptoms of the shock include headache at certain times together with profuse
sweating. Someone can be fatigued in one way or another, while others will start developing
Cardiac Nursing
may lead to him or her delivering a pace pulse (Lerman, 2016). There is a need to be keen on
ensuring that the electric current is increased as much as possible to ensure electric capture takes
place in the best way possible. These are essential when it comes to reducing the risks that come
with the transcutaneous pacing. Furthermore, this is according to "Emergency department use of
transcutaneous pacing for cardiac arrests" in the topic "Critical care medicine".
Module 4
Hypovolemic shock occurs when an individual loses more than twenty per cent
of his or her body's blood or even the fluid supply. Moreover, this situation makes it hard for the
heart to push enough blood to the organs, and this may lead to organ failure. The condition
always needs immediate medical attention. Some of its causes include bleeding that occurs due
to severe cuts or even wounds, and this leads to blood loss within the body. Moreover, there is
internal bleeding from the various abdominal organs, or there might be cases whereby the
ectopic pregnancy ruptures, leading to blood loss within the body. Furthermore, the shock can be
brought about by bleeding caused by the blunt traumatic injuries that occur due to injuries.
Bleeding that arises from the digestive tract can lead to higher chances of blood loss within the
body hence putting one's body at risk.
Virginal bleeding among the female can be a leading cause in some women, and
this has proven to be risky in most situations due to the massive amount of blood that someone
might lose in the process. The blood volume can be affected by the loss of body fluids. Excessive
sweating and even excessive vomiting can affect the fluid level in the body hence affecting the
blood volume at the end of the day, and this may lead to one developing the shock. Moreover,
some of the symptoms of the shock include headache at certain times together with profuse
sweating. Someone can be fatigued in one way or another, while others will start developing
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

10
Cardiac Nursing
nausea (Rackow, 2017). Some of the severe symptoms include losing consciousness by an
individual which may be dangerous in most situations, and the affected person should be rushed
to the hospital for immediate attention. Moreover, a rapid heart rate might occur during the
process, and this is a clear indication that all is not well, and there is a need to seek medication as
fast as possible.
Furthermore, an individual may start experiencing pale skin or even a weak
pulse. Others may be facing situations of less or even no urine output, which may be dangerous
to the body in one way or another; hence, there is a need for immediate checkup. Moreover, this
is according to "Fluid resuscitation in circulatory shock" in the topic "a comparison of the
cardiorespiratory effects of albumin". Some of the nursing care services that can be offered
include having the individual lie flat, and their feet should be elevated. Moreover, there is need
to avoid moving the patient if he or she develops some head, neck or even back injury and this
ensures no blood is lost in any way possible and that the body operates normally. The patient
should be as warm as possible in order to avoid hypothermia in the best way possible. Lastly,
there is a need to avoid offering the patient any fluids by mouth.
References
Willis, R., & Guyton, A. C. (2016). The Works of William Harvey. University of Pennsylvania
Press.
Hubble, M. A., Duncan, B. L., & Miller, S. D. (2016). The heart and soul of change: What
works in therapy (pp. xxiv-462). American Psychological Association.
Cardiac Nursing
nausea (Rackow, 2017). Some of the severe symptoms include losing consciousness by an
individual which may be dangerous in most situations, and the affected person should be rushed
to the hospital for immediate attention. Moreover, a rapid heart rate might occur during the
process, and this is a clear indication that all is not well, and there is a need to seek medication as
fast as possible.
Furthermore, an individual may start experiencing pale skin or even a weak
pulse. Others may be facing situations of less or even no urine output, which may be dangerous
to the body in one way or another; hence, there is a need for immediate checkup. Moreover, this
is according to "Fluid resuscitation in circulatory shock" in the topic "a comparison of the
cardiorespiratory effects of albumin". Some of the nursing care services that can be offered
include having the individual lie flat, and their feet should be elevated. Moreover, there is need
to avoid moving the patient if he or she develops some head, neck or even back injury and this
ensures no blood is lost in any way possible and that the body operates normally. The patient
should be as warm as possible in order to avoid hypothermia in the best way possible. Lastly,
there is a need to avoid offering the patient any fluids by mouth.
References
Willis, R., & Guyton, A. C. (2016). The Works of William Harvey. University of Pennsylvania
Press.
Hubble, M. A., Duncan, B. L., & Miller, S. D. (2016). The heart and soul of change: What
works in therapy (pp. xxiv-462). American Psychological Association.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

11
Cardiac Nursing
Duncan, B. L., Miller, S. D., Wampold, B. E., & Hubble, M. A. (2016). The heart and soul of
change: Delivering what works in therapy (pp. xxix-455). American Psychological Association.
Therap, P. (2016). CLASSIFICATION OF ANTIDYSRHYTHMIC DRUGS EM VAUGHAN
WILLIAMS DM, D. Sc.
Van Durme, J. P., Bogaert, M. G., & Rosseel, M. T. (2016). Therapeutic effectivenss and plasma
levels of aprindine, a new antidysrhythmic drug. European journal of clinical
pharmacology, 7(5), 343-346.
Arnsdorf, M. F. (2016). Electrophysiologic properties of antidysrhythmic drugs as a rational
basis for therapy. Medical Clinics of North America, 60(2), 213-232.
Dalsey, W. C., Syverud, S. A., & Hedges, J. R. (2016). Emergency department use of
transcutaneous pacing for cardiac arrests. Critical care medicine, 13(5), 399-401.
Lerman, D. J., & Myers, R. C. (2016). U.S. Patent No. 5,782,882. Washington, DC: U.S. Patent
and Trademark Office.
Faden, A. I., & Holaday, J. W. (2017). Opiate antagonists: a role in the treatment of hypovolemic
shock. Science, 205(4403), 317-318.
Rackow, E. C., Falk, J. L., Fein, I. A., Siegel, J. S., Packman, M. I., Haupt, M. T., ... & Putnam,
D. A. V. I. D. (2017). Fluid resuscitation in circulatory shock: a comparison of the
cardiorespiratory effects of albumin, hetastarch, and saline solutions in patients with
hypovolemic and septic shock. Critical care medicine, 11(11), 839-850.
Cardiac Nursing
Duncan, B. L., Miller, S. D., Wampold, B. E., & Hubble, M. A. (2016). The heart and soul of
change: Delivering what works in therapy (pp. xxix-455). American Psychological Association.
Therap, P. (2016). CLASSIFICATION OF ANTIDYSRHYTHMIC DRUGS EM VAUGHAN
WILLIAMS DM, D. Sc.
Van Durme, J. P., Bogaert, M. G., & Rosseel, M. T. (2016). Therapeutic effectivenss and plasma
levels of aprindine, a new antidysrhythmic drug. European journal of clinical
pharmacology, 7(5), 343-346.
Arnsdorf, M. F. (2016). Electrophysiologic properties of antidysrhythmic drugs as a rational
basis for therapy. Medical Clinics of North America, 60(2), 213-232.
Dalsey, W. C., Syverud, S. A., & Hedges, J. R. (2016). Emergency department use of
transcutaneous pacing for cardiac arrests. Critical care medicine, 13(5), 399-401.
Lerman, D. J., & Myers, R. C. (2016). U.S. Patent No. 5,782,882. Washington, DC: U.S. Patent
and Trademark Office.
Faden, A. I., & Holaday, J. W. (2017). Opiate antagonists: a role in the treatment of hypovolemic
shock. Science, 205(4403), 317-318.
Rackow, E. C., Falk, J. L., Fein, I. A., Siegel, J. S., Packman, M. I., Haupt, M. T., ... & Putnam,
D. A. V. I. D. (2017). Fluid resuscitation in circulatory shock: a comparison of the
cardiorespiratory effects of albumin, hetastarch, and saline solutions in patients with
hypovolemic and septic shock. Critical care medicine, 11(11), 839-850.
1 out of 11
Related Documents
Your All-in-One AI-Powered Toolkit for Academic Success.
+13062052269
info@desklib.com
Available 24*7 on WhatsApp / Email
![[object Object]](/_next/static/media/star-bottom.7253800d.svg)
Unlock your academic potential
Copyright © 2020–2026 A2Z Services. All Rights Reserved. Developed and managed by ZUCOL.




