Comparative Analysis of Vaccine Mandates in US, Europe, and Australia
VerifiedAdded on 2022/09/14
|8
|9373
|13
Report
AI Summary
This report presents a comparative analysis of recent vaccine mandates implemented in the United States, Europe, and Australia. It examines the diverse forms these mandates take, including their structure, exemptions, target populations, consequences, and enforcement mechanisms. The study compares policies in California, Italy, France, Germany, Australia, and Washington, ranking them by restrictiveness and highlighting differences in their approach. The analysis considers the political and cultural contexts influencing policy decisions, emphasizing the importance of public trust and historical precedent. The report also discusses the mechanisms by which vaccine mandates are constructed and implemented, including the involvement of stakeholder groups. The report identifies key considerations for policymakers when implementing or reforming vaccine mandates, including the need to address both access and acceptance issues related to vaccination and provides insights into the effectiveness of different policy approaches in increasing immunization coverage and addressing vaccine hesitancy. The report also highlights unintended consequences and enforcement challenges associated with different mandate policies.

Recent vaccine mandates in the United States,Europe and Australia:
A comparative study
Katie Attwella,⇑
, Mark C. Navin b, Pier Luigi Lopalcoc, Christine Jestind, Sabine Reitere, Saad B.Omerf
a Political Science and International Relations,University of Western Australia,35 Stirling Highway,Crawley 6009,Australia
b Department of Philosophy,Oakland University,146 Library Drive,Rochester,MI 48309-4479,USA
c Department of Translational Research on New Technologies in Medicine and Surgery,University of Pisa,Lungarno Antonio Pacinotti,43, 56126 Pisa Pl,Italy
d Sante Publique France,12 rue du Val d’Osne,94415 Saint-Maurice Cedex,France
e Infectious Diseases,Antimicrobial Resistance,Hygiene,Vaccination Federal Ministry of Health,Bundesministerium für Gesundheit Referat,322 Friedrichstraße 108,10117
Berlin,Germany
f Rollins School of Public Health,Emory University,1518 Clifton Road NE,Atlanta,GA 20211,USA
a r t i c l e i n f o
Article history:
Received 18 June 2018
Received in revised form 3 October 2018
Accepted 4 October 2018
Available online xxxx
Keywords:
Vaccination
Immunization
Mandatory
Mandates
Policy
a b s t r a c t
Background:In response to recent outbreaks of vaccine-preventable diseases and concerns around vac-
cine refusal,several high-income countries have adopted or reformed vaccine mandate policies.While
all make it more difficult for parents to refuse vaccines, the nature and scope of ‘mandatory vaccination’
is heterogeneous,and there has been no attempt to develop a detailed,comparative systematic account
of the possible forms mandates can take.
Methods:We compare the construction, introduction/amendment, and operation of six new high profile
vaccine mandates in Australia, France, Germany, Italy, California, and Washington. We rank these policie
in order of their relative restrictiveness and analyze other differences between them.
Results:New mandate instruments differ in their effects on behavior, and with regard to their structure,
exemptions,target populations,consequences and enforcement.We identify diverse means by which
vaccine mandates can restrict behaviors, various degrees of severity, and different gradations of intensit
in enforcement.
Conclusion:We suggest that politico-cultural context and vaccine policy history are centrally important
factors for vaccine mandate policymakers to consider.It matters whether citizens trust their govern-
ments to limit individual freedom in the name of public health,and whether citizens have previously
been subjected to vaccine mandates.Furthermore,political communities mustconsider the diverse
mechanisms by which they may construct vaccine mandate policies;whether through emergency
decrees or ordinary statutes,and how (or whether) to involve various stakeholder groups in developing
and implementing new vaccine mandate policies.
Ó 2018 Elsevier Ltd.All rights reserved.
1. Introduction
Outbreaks of vaccine preventable diseases have recently
occurred in many countries,e.g.measles in France,mumps in Ire-
land, and pertussis in the US. Several governments have responded
by introducing or strengthening vaccine mandates; other jurisdic-
tions are considering similar policies.Mandate instruments are
heterogeneous in how they operate to organise and change behav-
ior, with regard to structure,exemptions,target populations,con-
sequences and enforcement. Yet the nature and scope of
‘mandatory vaccination’is indeterminate,and there has not yet
been a systematic comparative synthesis of mandate policy devel-
opment, implementation and structure.Debates about vaccine
mandates ought to be informed by accurate accounts of the diverse
aims and requirements that vaccine mandate policies involve.In
this article, we compare new vaccine mandate policies adopted
in four countries and two US states in the last two years. We have
chosen our case studies as high profile exemplars of policy changes
in response to vaccine rejection and/or disease outbreaks; policy-
makers within these jurisdictions reference each other’s policies
as trends or templates [1]. We outline these new mandatory
policies in order of their relative restrictiveness, based on how dif-
ficult they make it for parents to refuse vaccines for their children.
Our comparison yields clear lessons for jurisdictions considering
implementing or reforming vaccine mandates,including a need
https://doi.org/10.1016/j.vaccine.2018.10.019
0264-410X/Ó 2018 Elsevier Ltd.All rights reserved.
⇑ Corresponding author.
E-mail address: Katie.attwell@uwa.edu.au (K.Attwell).
Vaccine xxx (2018) xxx–xxx
Contents lists available at ScienceDirect
Vaccine
j o u r n a lhomepage: w w w . e l s e v i e r . c o m / l o c a t e / v a c c i n e
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
A comparative study
Katie Attwella,⇑
, Mark C. Navin b, Pier Luigi Lopalcoc, Christine Jestind, Sabine Reitere, Saad B.Omerf
a Political Science and International Relations,University of Western Australia,35 Stirling Highway,Crawley 6009,Australia
b Department of Philosophy,Oakland University,146 Library Drive,Rochester,MI 48309-4479,USA
c Department of Translational Research on New Technologies in Medicine and Surgery,University of Pisa,Lungarno Antonio Pacinotti,43, 56126 Pisa Pl,Italy
d Sante Publique France,12 rue du Val d’Osne,94415 Saint-Maurice Cedex,France
e Infectious Diseases,Antimicrobial Resistance,Hygiene,Vaccination Federal Ministry of Health,Bundesministerium für Gesundheit Referat,322 Friedrichstraße 108,10117
Berlin,Germany
f Rollins School of Public Health,Emory University,1518 Clifton Road NE,Atlanta,GA 20211,USA
a r t i c l e i n f o
Article history:
Received 18 June 2018
Received in revised form 3 October 2018
Accepted 4 October 2018
Available online xxxx
Keywords:
Vaccination
Immunization
Mandatory
Mandates
Policy
a b s t r a c t
Background:In response to recent outbreaks of vaccine-preventable diseases and concerns around vac-
cine refusal,several high-income countries have adopted or reformed vaccine mandate policies.While
all make it more difficult for parents to refuse vaccines, the nature and scope of ‘mandatory vaccination’
is heterogeneous,and there has been no attempt to develop a detailed,comparative systematic account
of the possible forms mandates can take.
Methods:We compare the construction, introduction/amendment, and operation of six new high profile
vaccine mandates in Australia, France, Germany, Italy, California, and Washington. We rank these policie
in order of their relative restrictiveness and analyze other differences between them.
Results:New mandate instruments differ in their effects on behavior, and with regard to their structure,
exemptions,target populations,consequences and enforcement.We identify diverse means by which
vaccine mandates can restrict behaviors, various degrees of severity, and different gradations of intensit
in enforcement.
Conclusion:We suggest that politico-cultural context and vaccine policy history are centrally important
factors for vaccine mandate policymakers to consider.It matters whether citizens trust their govern-
ments to limit individual freedom in the name of public health,and whether citizens have previously
been subjected to vaccine mandates.Furthermore,political communities mustconsider the diverse
mechanisms by which they may construct vaccine mandate policies;whether through emergency
decrees or ordinary statutes,and how (or whether) to involve various stakeholder groups in developing
and implementing new vaccine mandate policies.
Ó 2018 Elsevier Ltd.All rights reserved.
1. Introduction
Outbreaks of vaccine preventable diseases have recently
occurred in many countries,e.g.measles in France,mumps in Ire-
land, and pertussis in the US. Several governments have responded
by introducing or strengthening vaccine mandates; other jurisdic-
tions are considering similar policies.Mandate instruments are
heterogeneous in how they operate to organise and change behav-
ior, with regard to structure,exemptions,target populations,con-
sequences and enforcement. Yet the nature and scope of
‘mandatory vaccination’is indeterminate,and there has not yet
been a systematic comparative synthesis of mandate policy devel-
opment, implementation and structure.Debates about vaccine
mandates ought to be informed by accurate accounts of the diverse
aims and requirements that vaccine mandate policies involve.In
this article, we compare new vaccine mandate policies adopted
in four countries and two US states in the last two years. We have
chosen our case studies as high profile exemplars of policy changes
in response to vaccine rejection and/or disease outbreaks; policy-
makers within these jurisdictions reference each other’s policies
as trends or templates [1]. We outline these new mandatory
policies in order of their relative restrictiveness, based on how dif-
ficult they make it for parents to refuse vaccines for their children.
Our comparison yields clear lessons for jurisdictions considering
implementing or reforming vaccine mandates,including a need
https://doi.org/10.1016/j.vaccine.2018.10.019
0264-410X/Ó 2018 Elsevier Ltd.All rights reserved.
⇑ Corresponding author.
E-mail address: Katie.attwell@uwa.edu.au (K.Attwell).
Vaccine xxx (2018) xxx–xxx
Contents lists available at ScienceDirect
Vaccine
j o u r n a lhomepage: w w w . e l s e v i e r . c o m / l o c a t e / v a c c i n e
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

to pay attention to political and policy considerations of path
dependency.
2. Mandates come in different shapes and sizes
Courts in countries around the world have long recognized the
legitimacy of liberty-infringing public health efforts, in light of the
priority that communities place on avoiding disease [2,3].Such
efforts include vaccine mandates,which have only rarely been
overturned by courts [1]. When considering mandates, policymak-
ers must address divergentaccess and acceptance reasons that
populations may remain under-vaccinated.Access refers to the
availability, affordability and convenience of services; parental
complacency may also fit here.Acceptance,by contrast,relates to
vaccine hesitancy [4]. Parents fear ingredients, distrust authorities,
or do not regard vaccination as congruent with their parenting
practices [5]. Vaccine mandates can address acceptance by making
it harder – or more consequential – for parents to refuse vaccines.
However, mandates govern access (complacency)too, as we
explain below.
We can better understand jurisdictions’vaccine mandates by
locating them on an ideal-type continuum (Fig. 1). At one end, vac-
cination is voluntary, and state interventions merely nudge or per-
suade individuals to vaccinate.At the other end,vaccine refusers
are fined or imprisoned. Here, the state’s coercive power motivates
individuals to utilise available vaccination services.
Between these ends ofthe continuum are positively framed
requirements.The first links vaccine uptake to public goods such
as state-subsidised daycare and public schools,while the second
links uptake to financial incentives.Both function as ‘carrots’that
only the vaccinated can obtain;compliers are offered a benefit
which is denied to non-compliers.
We can then differentiate ‘carrot’ policies on the basis of
exemptions.Towards the voluntary end of the spectrum,compli-
ance means an individualattains the benefit,but non-compliers
can obtain it after performing specified actions.This overcomes
complacency,whilst constructing an exemption process for non-
compliers to follow. Towards the coercive end ofthe spectrum,
exemption processes are removed (except in the case of medical
contra-indications to vaccination).As ‘carrot’policies move along
the spectrum towards coercion, there is no change to the
governance of compliers,who might have access barriers or need
motivation.However,vaccine rejection meets consequences that
cannot be ‘worked around’with exemptions.In the next section,
we compare mandate policies in six jurisdictions that have
recently introduced or strengthened them,starting with what we
rank as the most restrictive and moving to the least restrictive poli-
cies. We note that while we use a terminology of restrictiveness,
other scholars have recently employed a terminology ofrigidity
(from hard to soft) [6].
3. Country case studies
3.1.California
All US states require children to receive vaccines to attend day-
care or school (specific vaccines for the states in this study are
listed in Table 1).Since September 23,2010,the Affordable Care
Act has required vaccines recommended by the Advisory Commit-
tee on Immunization Practices (ACIP) to be covered by insurance.
The Vaccines for Children Program (a federally-funded and state-
administered program)provides free vaccines for children who
are uninsured or Medicaid eligible.Most US states permit parents
and guardians to receive nonmedical exemptions (NMEs) to immu-
nization mandates [7]. A 2010 national survey of US parents found
that 77% of parents with children aged 1–6 had a vaccine concern,
which included beliefs that vaccine ingredients may be unsafe
(26%) and that vaccines may cause learning disabilities such as aut-
ism (30%). In light of rising NME rates in California, the state legis-
lature recently passed two laws to successively restrict parents’
access to them.
Assembly Bill 2109 (in effect January 1, 2014 to January 1, 2016)
made it more difficult for parents or guardians to receive NMEs by
requiring applicants to submit an officialstate form on which a
physician attested that they provided information regarding the
benefits/risks ofimmunization [8].At the time of Assembly Bill
2109’s introduction,90.2% ofentering Kindergarteners were up-
to-date on all required vaccines.The rate of nonmedicalexemp-
tions was 3.1% [9]. Assembly Bill 2109 aimed to reduce NME rates
by targeting the complacent;parents and guardians with only
moderate objections might decide to vaccinate rather than
complete burdensome paperwork,as previous research indicated
was likely [10]. Assembly Bill 2109 was associated with a 25%
reduction in California’s NME rates (from 3.1% to 2.3%), and signif-
icant increases up-to-date status for entering Kindergarteners,
Fig. 1. The conceptual continuum of options available to policymakers for vaccine mandates.
2 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
dependency.
2. Mandates come in different shapes and sizes
Courts in countries around the world have long recognized the
legitimacy of liberty-infringing public health efforts, in light of the
priority that communities place on avoiding disease [2,3].Such
efforts include vaccine mandates,which have only rarely been
overturned by courts [1]. When considering mandates, policymak-
ers must address divergentaccess and acceptance reasons that
populations may remain under-vaccinated.Access refers to the
availability, affordability and convenience of services; parental
complacency may also fit here.Acceptance,by contrast,relates to
vaccine hesitancy [4]. Parents fear ingredients, distrust authorities,
or do not regard vaccination as congruent with their parenting
practices [5]. Vaccine mandates can address acceptance by making
it harder – or more consequential – for parents to refuse vaccines.
However, mandates govern access (complacency)too, as we
explain below.
We can better understand jurisdictions’vaccine mandates by
locating them on an ideal-type continuum (Fig. 1). At one end, vac-
cination is voluntary, and state interventions merely nudge or per-
suade individuals to vaccinate.At the other end,vaccine refusers
are fined or imprisoned. Here, the state’s coercive power motivates
individuals to utilise available vaccination services.
Between these ends ofthe continuum are positively framed
requirements.The first links vaccine uptake to public goods such
as state-subsidised daycare and public schools,while the second
links uptake to financial incentives.Both function as ‘carrots’that
only the vaccinated can obtain;compliers are offered a benefit
which is denied to non-compliers.
We can then differentiate ‘carrot’ policies on the basis of
exemptions.Towards the voluntary end of the spectrum,compli-
ance means an individualattains the benefit,but non-compliers
can obtain it after performing specified actions.This overcomes
complacency,whilst constructing an exemption process for non-
compliers to follow. Towards the coercive end ofthe spectrum,
exemption processes are removed (except in the case of medical
contra-indications to vaccination).As ‘carrot’policies move along
the spectrum towards coercion, there is no change to the
governance of compliers,who might have access barriers or need
motivation.However,vaccine rejection meets consequences that
cannot be ‘worked around’with exemptions.In the next section,
we compare mandate policies in six jurisdictions that have
recently introduced or strengthened them,starting with what we
rank as the most restrictive and moving to the least restrictive poli-
cies. We note that while we use a terminology of restrictiveness,
other scholars have recently employed a terminology ofrigidity
(from hard to soft) [6].
3. Country case studies
3.1.California
All US states require children to receive vaccines to attend day-
care or school (specific vaccines for the states in this study are
listed in Table 1).Since September 23,2010,the Affordable Care
Act has required vaccines recommended by the Advisory Commit-
tee on Immunization Practices (ACIP) to be covered by insurance.
The Vaccines for Children Program (a federally-funded and state-
administered program)provides free vaccines for children who
are uninsured or Medicaid eligible.Most US states permit parents
and guardians to receive nonmedical exemptions (NMEs) to immu-
nization mandates [7]. A 2010 national survey of US parents found
that 77% of parents with children aged 1–6 had a vaccine concern,
which included beliefs that vaccine ingredients may be unsafe
(26%) and that vaccines may cause learning disabilities such as aut-
ism (30%). In light of rising NME rates in California, the state legis-
lature recently passed two laws to successively restrict parents’
access to them.
Assembly Bill 2109 (in effect January 1, 2014 to January 1, 2016)
made it more difficult for parents or guardians to receive NMEs by
requiring applicants to submit an officialstate form on which a
physician attested that they provided information regarding the
benefits/risks ofimmunization [8].At the time of Assembly Bill
2109’s introduction,90.2% ofentering Kindergarteners were up-
to-date on all required vaccines.The rate of nonmedicalexemp-
tions was 3.1% [9]. Assembly Bill 2109 aimed to reduce NME rates
by targeting the complacent;parents and guardians with only
moderate objections might decide to vaccinate rather than
complete burdensome paperwork,as previous research indicated
was likely [10]. Assembly Bill 2109 was associated with a 25%
reduction in California’s NME rates (from 3.1% to 2.3%), and signif-
icant increases up-to-date status for entering Kindergarteners,
Fig. 1. The conceptual continuum of options available to policymakers for vaccine mandates.
2 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
from 90.2% to 92.9% [9].However,this decline was not uniform,
and left major geographic exemptions clusters undisturbed [11].
Subsequently,Senate Bill 277 (enacted June 30,2015) elimi-
nated access to NMEs entirely in California [12].With this new
law, California joined West Virginia and Mississippias the only
US states not to provide NMEs [7]. Advocates argued that eliminat-
ing NMEs was necessary to further increase California’s immuniza-
tion coverage [13].However,it seems likely that they were also
motivated by the high-profile 2014–15 Disneyland measles out-
break [9,14],which may explain why the Bill’s authors (Richard
Pan and Ben Allen) were unwilling to wait to see the impact of
the earlier Assembly Bill 2109 on California’s NME rates (outlined
above) [9].
While there is some preliminary evidence that SB 277 has fur-
ther increased immunization coverage beyond the gains realized
by AB 2109,questions remain about enforcement and unintended
consequences.Financially vulnerable private schools may decide
not to enforce immunization requirements rather than risk school
closure due to declining tuition revenues from vaccine refusers
[15].Some physicians may support marginal or fraudulent claims
for medical exemptions, which likely explains why medical exemp-
tion rates in California have tripled since the passage of Senate Bill
277 [16].Also, Senate Bill 277 may cultivate political polarization
surrounding vaccination policy and science:most Democrats in
the California Senate voted for it,while most Republicans voted
against it,reversing a history of bipartisan vaccination policies in
the US [17].
3.2.Italy
Italy has a history of mandates for some vaccines for older chil-
dren, including diphtheria (1939), polio (1966), tetanus (1968), and
hepatitis B (1991). Mandated vaccines were offered at no cost, and
statutes authorized fines and school exclusion for children who did
not receive them.Persistent parents,however,could receive per-
mission for non-compliant children to enrol in school, after parents
attended meetings with public health officers or the Minors Court.
Fines were rarely applied. A suite of additional ‘recommended’ vac-
cines were also offered for free,notably MMR and pertussis.
Policy shifts occurred from 1999 onwards,with a Ministry of
Education decree that children who had not received mandatory
vaccinations should still be allowed to attend school. This was
based on Italy’s constitution, in which a right to education is equal
to the right to health. From here, mandates remained ‘on the
books’,but not enforced.
In 2007, the Veneto region piloted a mandate suspension,
reflecting popular opinion that the state ought to affirm the impor-
tance of vaccination,but not mandate it [18].However,in 2013,a
local court in Rimini ruled that vaccines caused a child’s autism,
which prompted significant media coverage and internet search
activity [19]. The subsequent2015 overturning of the case did
not receive the same media coverage [20].Starting from 2013,
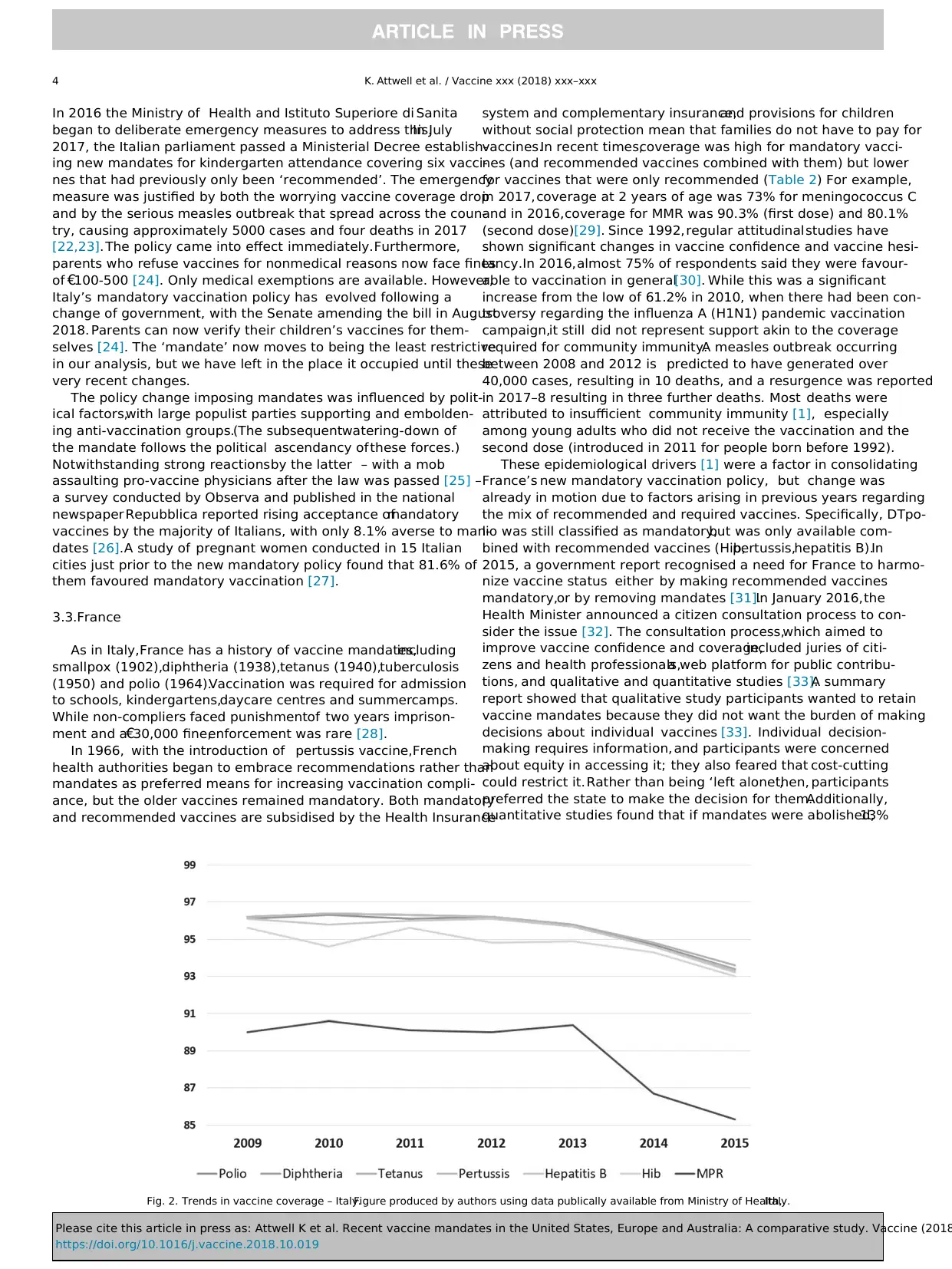
nation-wide vaccination coverage dropped significantly (Fig.2).
In 2016 a cross-sectional survey showed that 15.6% of Italian par-
ents were vaccine hesitant and 0.7% strongly vaccine opposed [21].
Table 1
Characteristics of recent vaccine mandates.
Jurisdiction Implementation
date
Antigens covered Key reason for policy
change
Policy development
process
Exemptions Penalties/
enforcement
Gaps
California January 2016 Diphtheria,Hepatitis B,
Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
Large numbers of
personal belief
exemptions;
Disneyland measles
outbreak (2014–5)
Professional society
lobbying; participation
of State Senator Pan
(physician) produced
quick legislative
response
Medical only Exclusion from
daycare and
school
Children cared
for/schooled at
home
Italy Jul 2017 Diphtheria,Hepatitis B,
Hib, Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
Declining rates
following increasing
vaccine hesitancy
Ministry of Health
decision (Government
Decree)
Medical only Exclusion from
daycare and
pre-school (3–5
years); fines
€100-€500
Children cared
for at home. No
consequence
after initial fine
for children 6–
16 years
France Jan 2018 Diphtheria,Hepatitis B,
Hib, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcol,Polio,
Rubella,Tetanus
Coexistence of
mandatory and
recommended
vaccines; conclusion
of the consultation;
court case hastens
harmonisation
Comprehensive
consultation including
citizen’s juries; several
reports;Government
decision,parliament
hearing and vote
Medical only Exclusion from
daycare,school,
holiday camps.
Potential legal
proceedings for
damages
Children cared
for at home
Australia January 2016 Diphtheria,Hepatitis B,
Hib, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcal,Polio,
Rubella,Tetanus,
Varicella
Media lobbying;
Pertussis deaths
Parliamentary hearing,
including consultation
with experts/key
stakeholders and
consideration of
submissions from
general public
Medical; other
limited
exemptions
Loss of up to
$8350/year in
financial
assistance
High income
earners; but
annual
consequence
for others
Washington July 2011 Diphtheria,Hepatitis B,
Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
One of the highest
rates of personal
belief exemptions in
USA; Pertussis
outbreaks 2010
State Health
Department request;
stakeholder advocacy
Religious,
personal belief
after medical
counselling
Exclusion from
daycare and
school unless
exemption
obtained
Children cared
for/schooled at
home.Those
who claim
appropriate
religious
affiliation
Germany June 2017 Diphtheria,Hepatitis B,
Hib, HPV, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcal,Polio,
Rotavirus,Rubella,
Tetanus,Varicella
Measles outbreaks Government led action
plan involving key
stakeholders
Must provide
form at day
care entry; no
exemption for
form but vax
not required
Up to €2500
fine
Children cared
for at home. No
consequence
after initial fine
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 3
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
and left major geographic exemptions clusters undisturbed [11].
Subsequently,Senate Bill 277 (enacted June 30,2015) elimi-
nated access to NMEs entirely in California [12].With this new
law, California joined West Virginia and Mississippias the only
US states not to provide NMEs [7]. Advocates argued that eliminat-
ing NMEs was necessary to further increase California’s immuniza-
tion coverage [13].However,it seems likely that they were also
motivated by the high-profile 2014–15 Disneyland measles out-
break [9,14],which may explain why the Bill’s authors (Richard
Pan and Ben Allen) were unwilling to wait to see the impact of
the earlier Assembly Bill 2109 on California’s NME rates (outlined
above) [9].
While there is some preliminary evidence that SB 277 has fur-
ther increased immunization coverage beyond the gains realized
by AB 2109,questions remain about enforcement and unintended
consequences.Financially vulnerable private schools may decide
not to enforce immunization requirements rather than risk school
closure due to declining tuition revenues from vaccine refusers
[15].Some physicians may support marginal or fraudulent claims
for medical exemptions, which likely explains why medical exemp-
tion rates in California have tripled since the passage of Senate Bill
277 [16].Also, Senate Bill 277 may cultivate political polarization
surrounding vaccination policy and science:most Democrats in
the California Senate voted for it,while most Republicans voted
against it,reversing a history of bipartisan vaccination policies in
the US [17].
3.2.Italy
Italy has a history of mandates for some vaccines for older chil-
dren, including diphtheria (1939), polio (1966), tetanus (1968), and
hepatitis B (1991). Mandated vaccines were offered at no cost, and
statutes authorized fines and school exclusion for children who did
not receive them.Persistent parents,however,could receive per-
mission for non-compliant children to enrol in school, after parents
attended meetings with public health officers or the Minors Court.
Fines were rarely applied. A suite of additional ‘recommended’ vac-
cines were also offered for free,notably MMR and pertussis.
Policy shifts occurred from 1999 onwards,with a Ministry of
Education decree that children who had not received mandatory
vaccinations should still be allowed to attend school. This was
based on Italy’s constitution, in which a right to education is equal
to the right to health. From here, mandates remained ‘on the
books’,but not enforced.
In 2007, the Veneto region piloted a mandate suspension,
reflecting popular opinion that the state ought to affirm the impor-
tance of vaccination,but not mandate it [18].However,in 2013,a
local court in Rimini ruled that vaccines caused a child’s autism,
which prompted significant media coverage and internet search
activity [19]. The subsequent2015 overturning of the case did
not receive the same media coverage [20].Starting from 2013,
nation-wide vaccination coverage dropped significantly (Fig.2).
In 2016 a cross-sectional survey showed that 15.6% of Italian par-
ents were vaccine hesitant and 0.7% strongly vaccine opposed [21].
Table 1
Characteristics of recent vaccine mandates.
Jurisdiction Implementation
date
Antigens covered Key reason for policy
change
Policy development
process
Exemptions Penalties/
enforcement
Gaps
California January 2016 Diphtheria,Hepatitis B,
Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
Large numbers of
personal belief
exemptions;
Disneyland measles
outbreak (2014–5)
Professional society
lobbying; participation
of State Senator Pan
(physician) produced
quick legislative
response
Medical only Exclusion from
daycare and
school
Children cared
for/schooled at
home
Italy Jul 2017 Diphtheria,Hepatitis B,
Hib, Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
Declining rates
following increasing
vaccine hesitancy
Ministry of Health
decision (Government
Decree)
Medical only Exclusion from
daycare and
pre-school (3–5
years); fines
€100-€500
Children cared
for at home. No
consequence
after initial fine
for children 6–
16 years
France Jan 2018 Diphtheria,Hepatitis B,
Hib, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcol,Polio,
Rubella,Tetanus
Coexistence of
mandatory and
recommended
vaccines; conclusion
of the consultation;
court case hastens
harmonisation
Comprehensive
consultation including
citizen’s juries; several
reports;Government
decision,parliament
hearing and vote
Medical only Exclusion from
daycare,school,
holiday camps.
Potential legal
proceedings for
damages
Children cared
for at home
Australia January 2016 Diphtheria,Hepatitis B,
Hib, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcal,Polio,
Rubella,Tetanus,
Varicella
Media lobbying;
Pertussis deaths
Parliamentary hearing,
including consultation
with experts/key
stakeholders and
consideration of
submissions from
general public
Medical; other
limited
exemptions
Loss of up to
$8350/year in
financial
assistance
High income
earners; but
annual
consequence
for others
Washington July 2011 Diphtheria,Hepatitis B,
Measles,Mumps,
Pertussis,Polio, Rubella,
Tetanus,Varicella
One of the highest
rates of personal
belief exemptions in
USA; Pertussis
outbreaks 2010
State Health
Department request;
stakeholder advocacy
Religious,
personal belief
after medical
counselling
Exclusion from
daycare and
school unless
exemption
obtained
Children cared
for/schooled at
home.Those
who claim
appropriate
religious
affiliation
Germany June 2017 Diphtheria,Hepatitis B,
Hib, HPV, Measles,
Meningococcal C,
Mumps, Pertussis,
Pneumococcal,Polio,
Rotavirus,Rubella,
Tetanus,Varicella
Measles outbreaks Government led action
plan involving key
stakeholders
Must provide
form at day
care entry; no
exemption for
form but vax
not required
Up to €2500
fine
Children cared
for at home. No
consequence
after initial fine
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 3
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide
In 2016 the Ministry of Health and Istituto Superiore di Sanita
began to deliberate emergency measures to address this.In July
2017, the Italian parliament passed a Ministerial Decree establish-
ing new mandates for kindergarten attendance covering six vacci-
nes that had previously only been ‘recommended’. The emergency
measure was justified by both the worrying vaccine coverage drop
and by the serious measles outbreak that spread across the coun-
try, causing approximately 5000 cases and four deaths in 2017
[22,23].The policy came into effect immediately.Furthermore,
parents who refuse vaccines for nonmedical reasons now face fines
of €100-500 [24]. Only medical exemptions are available. However,
Italy’s mandatory vaccination policy has evolved following a
change of government, with the Senate amending the bill in August
2018. Parents can now verify their children’s vaccines for them-
selves [24]. The ‘mandate’ now moves to being the least restrictive
in our analysis, but we have left in the place it occupied until these
very recent changes.
The policy change imposing mandates was influenced by polit-
ical factors,with large populist parties supporting and embolden-
ing anti-vaccination groups.(The subsequentwatering-down of
the mandate follows the political ascendancy of these forces.)
Notwithstanding strong reactionsby the latter – with a mob
assaulting pro-vaccine physicians after the law was passed [25] –
a survey conducted by Observa and published in the national
newspaper Repubblica reported rising acceptance ofmandatory
vaccines by the majority of Italians, with only 8.1% averse to man-
dates [26].A study of pregnant women conducted in 15 Italian
cities just prior to the new mandatory policy found that 81.6% of
them favoured mandatory vaccination [27].
3.3.France
As in Italy,France has a history of vaccine mandates,including
smallpox (1902),diphtheria (1938),tetanus (1940),tuberculosis
(1950) and polio (1964).Vaccination was required for admission
to schools, kindergartens,daycare centres and summercamps.
While non-compliers faced punishmentof two years imprison-
ment and a€30,000 fine,enforcement was rare [28].
In 1966, with the introduction of pertussis vaccine,French
health authorities began to embrace recommendations rather than
mandates as preferred means for increasing vaccination compli-
ance, but the older vaccines remained mandatory. Both mandatory
and recommended vaccines are subsidised by the Health Insurance
system and complementary insurance,and provisions for children
without social protection mean that families do not have to pay for
vaccines.In recent times,coverage was high for mandatory vacci-
nes (and recommended vaccines combined with them) but lower
for vaccines that were only recommended (Table 2) For example,
in 2017,coverage at 2 years of age was 73% for meningococcus C
and in 2016,coverage for MMR was 90.3% (first dose) and 80.1%
(second dose)[29]. Since 1992,regular attitudinalstudies have
shown significant changes in vaccine confidence and vaccine hesi-
tancy.In 2016,almost 75% of respondents said they were favour-
able to vaccination in general[30]. While this was a significant
increase from the low of 61.2% in 2010, when there had been con-
troversy regarding the influenza A (H1N1) pandemic vaccination
campaign,it still did not represent support akin to the coverage
required for community immunity.A measles outbreak occurring
between 2008 and 2012 is predicted to have generated over
40,000 cases, resulting in 10 deaths, and a resurgence was reported
in 2017–8 resulting in three further deaths. Most deaths were
attributed to insufficient community immunity [1], especially
among young adults who did not receive the vaccination and the
second dose (introduced in 2011 for people born before 1992).
These epidemiological drivers [1] were a factor in consolidating
France’s new mandatory vaccination policy, but change was
already in motion due to factors arising in previous years regarding
the mix of recommended and required vaccines. Specifically, DTpo-
lio was still classified as mandatory,but was only available com-
bined with recommended vaccines (Hib,pertussis,hepatitis B).In
2015, a government report recognised a need for France to harmo-
nize vaccine status either by making recommended vaccines
mandatory,or by removing mandates [31].In January 2016,the
Health Minister announced a citizen consultation process to con-
sider the issue [32]. The consultation process,which aimed to
improve vaccine confidence and coverage,included juries of citi-
zens and health professionals,a web platform for public contribu-
tions, and qualitative and quantitative studies [33].A summary
report showed that qualitative study participants wanted to retain
vaccine mandates because they did not want the burden of making
decisions about individual vaccines [33]. Individual decision-
making requires information, and participants were concerned
about equity in accessing it; they also feared that cost-cutting
could restrict it.Rather than being ‘left alone’,then, participants
preferred the state to make the decision for them.Additionally,
quantitative studies found that if mandates were abolished,13%
Fig. 2. Trends in vaccine coverage – Italy.Figure produced by authors using data publically available from Ministry of Health,Italy.
4 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
began to deliberate emergency measures to address this.In July
2017, the Italian parliament passed a Ministerial Decree establish-
ing new mandates for kindergarten attendance covering six vacci-
nes that had previously only been ‘recommended’. The emergency
measure was justified by both the worrying vaccine coverage drop
and by the serious measles outbreak that spread across the coun-
try, causing approximately 5000 cases and four deaths in 2017
[22,23].The policy came into effect immediately.Furthermore,
parents who refuse vaccines for nonmedical reasons now face fines
of €100-500 [24]. Only medical exemptions are available. However,
Italy’s mandatory vaccination policy has evolved following a
change of government, with the Senate amending the bill in August
2018. Parents can now verify their children’s vaccines for them-
selves [24]. The ‘mandate’ now moves to being the least restrictive
in our analysis, but we have left in the place it occupied until these
very recent changes.
The policy change imposing mandates was influenced by polit-
ical factors,with large populist parties supporting and embolden-
ing anti-vaccination groups.(The subsequentwatering-down of
the mandate follows the political ascendancy of these forces.)
Notwithstanding strong reactionsby the latter – with a mob
assaulting pro-vaccine physicians after the law was passed [25] –
a survey conducted by Observa and published in the national
newspaper Repubblica reported rising acceptance ofmandatory
vaccines by the majority of Italians, with only 8.1% averse to man-
dates [26].A study of pregnant women conducted in 15 Italian
cities just prior to the new mandatory policy found that 81.6% of
them favoured mandatory vaccination [27].
3.3.France
As in Italy,France has a history of vaccine mandates,including
smallpox (1902),diphtheria (1938),tetanus (1940),tuberculosis
(1950) and polio (1964).Vaccination was required for admission
to schools, kindergartens,daycare centres and summercamps.
While non-compliers faced punishmentof two years imprison-
ment and a€30,000 fine,enforcement was rare [28].
In 1966, with the introduction of pertussis vaccine,French
health authorities began to embrace recommendations rather than
mandates as preferred means for increasing vaccination compli-
ance, but the older vaccines remained mandatory. Both mandatory
and recommended vaccines are subsidised by the Health Insurance
system and complementary insurance,and provisions for children
without social protection mean that families do not have to pay for
vaccines.In recent times,coverage was high for mandatory vacci-
nes (and recommended vaccines combined with them) but lower
for vaccines that were only recommended (Table 2) For example,
in 2017,coverage at 2 years of age was 73% for meningococcus C
and in 2016,coverage for MMR was 90.3% (first dose) and 80.1%
(second dose)[29]. Since 1992,regular attitudinalstudies have
shown significant changes in vaccine confidence and vaccine hesi-
tancy.In 2016,almost 75% of respondents said they were favour-
able to vaccination in general[30]. While this was a significant
increase from the low of 61.2% in 2010, when there had been con-
troversy regarding the influenza A (H1N1) pandemic vaccination
campaign,it still did not represent support akin to the coverage
required for community immunity.A measles outbreak occurring
between 2008 and 2012 is predicted to have generated over
40,000 cases, resulting in 10 deaths, and a resurgence was reported
in 2017–8 resulting in three further deaths. Most deaths were
attributed to insufficient community immunity [1], especially
among young adults who did not receive the vaccination and the
second dose (introduced in 2011 for people born before 1992).
These epidemiological drivers [1] were a factor in consolidating
France’s new mandatory vaccination policy, but change was
already in motion due to factors arising in previous years regarding
the mix of recommended and required vaccines. Specifically, DTpo-
lio was still classified as mandatory,but was only available com-
bined with recommended vaccines (Hib,pertussis,hepatitis B).In
2015, a government report recognised a need for France to harmo-
nize vaccine status either by making recommended vaccines
mandatory,or by removing mandates [31].In January 2016,the
Health Minister announced a citizen consultation process to con-
sider the issue [32]. The consultation process,which aimed to
improve vaccine confidence and coverage,included juries of citi-
zens and health professionals,a web platform for public contribu-
tions, and qualitative and quantitative studies [33].A summary
report showed that qualitative study participants wanted to retain
vaccine mandates because they did not want the burden of making
decisions about individual vaccines [33]. Individual decision-
making requires information, and participants were concerned
about equity in accessing it; they also feared that cost-cutting
could restrict it.Rather than being ‘left alone’,then, participants
preferred the state to make the decision for them.Additionally,
quantitative studies found that if mandates were abolished,13%
Fig. 2. Trends in vaccine coverage – Italy.Figure produced by authors using data publically available from Ministry of Health,Italy.
4 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

of parents would no longer vaccinate their children for DTPolio,
and that socio-economically disadvantaged parentswould be
over-represented in that population [33].As a result,participants
favoured extending mandatory vaccination to allvaccines for a
limited period. In return,they required transparency,information,
listening and communication,an official website, education and
training for health professionals to enhance their commitment,
vaccine education at schools,simplification of access,and expan-
sion of a vaccine injury compensation scheme [33].
The issue came to a head in February 2017. Vaccine refusers had
contested the mix of mandatory/recommended vaccines,and the
Council of State advised that the state must make mandated vacci-
nes available without combined recommended vaccines within six
months [34].Thus,on 5 July 2017 the Health Minister announced
that all recommended vaccines for children under 18 months age
old would become mandatory in 2018 (see Table 1).While the
specific criminal sanction for refusing vaccines has been abolished
[1], parents can still be prosecuted for putting their children or
others at risk [35].The decision was made to focus on new birth
cohorts rather than catch up schemes for older children,for epi-
demiological and enforcement reasons. Regarding the latter,
excluding older children from school was regarded as socially
unacceptable and risked inflaming the anti-vaccination movement
[1]. Further detail and perspectives on the French policy response
and process can be found here [36,37].
3.4.Australia
Australian vaccination policy has linked vaccination compliance
to financial incentives since 1998. This started with a non-means-
tested designated vaccination payment at age-based milestones. In
2012 the financial incentive was instead linked to annual means
tested end of financial year supplements [38]. Since 1998 vaccina-
tion status has also determined eligibility for childcare subsidies,
including a non-means-tested annual rebate [39]. Vaccine refusers
could submit a Conscientious Objector Form following counselling
by an immunisation provider,and still access incentives and ben-
efits. All recommended vaccines were covered by these policies,
and were available free of charge. Vaccination coverage in Australia
sat around 91% but refusers clustered in regions with coverage as
low as 50% [40]. In 2012, a representative national study found that
over one-fifth of adult Australians believed were concerned that
vaccines were insufficiently safety-tested,could cause autism,or
would weaken their child’s immune system [41].
In 2013,the main newspaper in New South Wales began cam-
paigning to deny vaccine refusers access to uptake-linked benefits.
They mobilised a discourse of collective responsibility and utilised
the high profile pertussis deaths of Australian infants in low cover-
age areas [42]. The ‘No Jab, No Pay’ campaign achieved popular and
government support. The latter aligned with a discourse of ‘mutual
obligation’ linking benefits to responsibilities [43], and recognition
that budget savings ofover $500 million in five years could be
made by withdrawing resources from refusers [44].
The sole purpose of the policy change was to govern vaccine
refusal; access and complacency were already governed by existing
administrative procedures. The ‘No Jab, No Pay’law – named after
the Daily Telegraph’scampaign (to which the Prime Minister
explicitly alluded in his announcement) – came into effect on 1
January 2016 [45,46].In its journey through Parliament,it was
referred to the Senate Community Affairs Legislation Committee,
which invited submissions and held two 25 min public hearings
[47]. Experts, activists and members of the public presented a
range of views, but the legislation passed, removing Conscientious
Objection and leaving medical exemptions as the only way for the
unvaccinated to access entitlements [48]. Refusers stood to lose up
to approximately $8350 per year, which increased with changes to
childcare subsidies in 2018 [49]. Neither the old nor the new policy
delivered any consequences for medium-to-high income vaccine
refusers whose children were not in daycare,which is attended
by approximately one quarter of Australian children [50].
‘No Jab, No Pay’ met popular approval,although some public
intellectuals lamented the loss of parental choice [51]. The Govern-
ment claimed the policy’s success in a subsequent release of fig-
ures showing vaccination coverage had climbed to 92–93%
[52,53].State-based ‘No Jab,No Play’ policy changes,advocated
by the FederalGovernment,limit unvaccinated children’s access
to childcare centres [54].It is beyond the scope of this article to
analyze these additionalstate-levelpolicies, suffice to say that
they, like the other mandates explored here,vary with regard to
structure,severity and enforcement.
3.5.Washington
We have provided an overview ofUS vaccination policy and
national rates of vaccine hesitancy in the section on California,
above. Washington state was one state that made nonmedical
exemptions readily available,and historically had some of the
highest rates in the U.S [55].In the three years leading up to the
introduction of a new policy, exemption rates for schoolentry
mandates in Washington ranged from approximately 7–9%. (While
this figure includes medical exemptions,these made up a very
small fraction of the total number of exemptions.) [56]. In the con-
text of large pertussis outbreaks in multiple states in 2010 that
included Washington,the state health department submitted an
agency request to the legislature for a change in the state’s exemp-
tion law. They sought to ‘‘Reduce the convenience of nonmedical
exemptions only to the extent exempting is equalto the effort
required to vaccinate (or provide proof of vaccination)” and
‘‘Increase public education and awareness of the dangers of
vaccine-preventable disease and the benefits ofimmunization.”
[57].
Senate Bill 5005 (SB5005) was implemented in July 2011 and
required parents seeking an exemption to submit a ‘‘Certificate of
Exemption” or a letter signed by a licensed healthcare provider
(23) verifying that the provider has discussed the benefits/risks
of vaccines with the parent(s). However, parents who demonstrate
affiliation with a religious entity that does not permit medical
Table 2
French vaccination uptake figures for 2 years of age,2015 (Meningococus C 2016).Source: Sante Publique France,reproduced with permission.
Vaccine Introduction Status Coverage Rate Uptake and Compliance
DT Polio (3 doses) 1938; 1940; 1964 Required 98.9% Stable
Pertussis (3 doses) 1966 Recommended; vaccine combined with other antigens 98.6% Stable
Hib 1993 Recommended; vaccine combined with other antigens 98.0% Stable
Hepatitis B (3 doses) 1995 Recommended; vaccine combined with other antigens 88.1% 42% in 2007
Pneumococcal (3 doses) 2006 Recommended; not combined with other antigens 91.6% Increasing
MMR - 1st dose 1983 Recommended 90.5% Stable
MMR - 2nd dose 2005 Recommended 78.8% Increasing
Meningococcal C 2010 Recommended 70.90% Increasing
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 5
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
and that socio-economically disadvantaged parentswould be
over-represented in that population [33].As a result,participants
favoured extending mandatory vaccination to allvaccines for a
limited period. In return,they required transparency,information,
listening and communication,an official website, education and
training for health professionals to enhance their commitment,
vaccine education at schools,simplification of access,and expan-
sion of a vaccine injury compensation scheme [33].
The issue came to a head in February 2017. Vaccine refusers had
contested the mix of mandatory/recommended vaccines,and the
Council of State advised that the state must make mandated vacci-
nes available without combined recommended vaccines within six
months [34].Thus,on 5 July 2017 the Health Minister announced
that all recommended vaccines for children under 18 months age
old would become mandatory in 2018 (see Table 1).While the
specific criminal sanction for refusing vaccines has been abolished
[1], parents can still be prosecuted for putting their children or
others at risk [35].The decision was made to focus on new birth
cohorts rather than catch up schemes for older children,for epi-
demiological and enforcement reasons. Regarding the latter,
excluding older children from school was regarded as socially
unacceptable and risked inflaming the anti-vaccination movement
[1]. Further detail and perspectives on the French policy response
and process can be found here [36,37].
3.4.Australia
Australian vaccination policy has linked vaccination compliance
to financial incentives since 1998. This started with a non-means-
tested designated vaccination payment at age-based milestones. In
2012 the financial incentive was instead linked to annual means
tested end of financial year supplements [38]. Since 1998 vaccina-
tion status has also determined eligibility for childcare subsidies,
including a non-means-tested annual rebate [39]. Vaccine refusers
could submit a Conscientious Objector Form following counselling
by an immunisation provider,and still access incentives and ben-
efits. All recommended vaccines were covered by these policies,
and were available free of charge. Vaccination coverage in Australia
sat around 91% but refusers clustered in regions with coverage as
low as 50% [40]. In 2012, a representative national study found that
over one-fifth of adult Australians believed were concerned that
vaccines were insufficiently safety-tested,could cause autism,or
would weaken their child’s immune system [41].
In 2013,the main newspaper in New South Wales began cam-
paigning to deny vaccine refusers access to uptake-linked benefits.
They mobilised a discourse of collective responsibility and utilised
the high profile pertussis deaths of Australian infants in low cover-
age areas [42]. The ‘No Jab, No Pay’ campaign achieved popular and
government support. The latter aligned with a discourse of ‘mutual
obligation’ linking benefits to responsibilities [43], and recognition
that budget savings ofover $500 million in five years could be
made by withdrawing resources from refusers [44].
The sole purpose of the policy change was to govern vaccine
refusal; access and complacency were already governed by existing
administrative procedures. The ‘No Jab, No Pay’law – named after
the Daily Telegraph’scampaign (to which the Prime Minister
explicitly alluded in his announcement) – came into effect on 1
January 2016 [45,46].In its journey through Parliament,it was
referred to the Senate Community Affairs Legislation Committee,
which invited submissions and held two 25 min public hearings
[47]. Experts, activists and members of the public presented a
range of views, but the legislation passed, removing Conscientious
Objection and leaving medical exemptions as the only way for the
unvaccinated to access entitlements [48]. Refusers stood to lose up
to approximately $8350 per year, which increased with changes to
childcare subsidies in 2018 [49]. Neither the old nor the new policy
delivered any consequences for medium-to-high income vaccine
refusers whose children were not in daycare,which is attended
by approximately one quarter of Australian children [50].
‘No Jab, No Pay’ met popular approval,although some public
intellectuals lamented the loss of parental choice [51]. The Govern-
ment claimed the policy’s success in a subsequent release of fig-
ures showing vaccination coverage had climbed to 92–93%
[52,53].State-based ‘No Jab,No Play’ policy changes,advocated
by the FederalGovernment,limit unvaccinated children’s access
to childcare centres [54].It is beyond the scope of this article to
analyze these additionalstate-levelpolicies, suffice to say that
they, like the other mandates explored here,vary with regard to
structure,severity and enforcement.
3.5.Washington
We have provided an overview ofUS vaccination policy and
national rates of vaccine hesitancy in the section on California,
above. Washington state was one state that made nonmedical
exemptions readily available,and historically had some of the
highest rates in the U.S [55].In the three years leading up to the
introduction of a new policy, exemption rates for schoolentry
mandates in Washington ranged from approximately 7–9%. (While
this figure includes medical exemptions,these made up a very
small fraction of the total number of exemptions.) [56]. In the con-
text of large pertussis outbreaks in multiple states in 2010 that
included Washington,the state health department submitted an
agency request to the legislature for a change in the state’s exemp-
tion law. They sought to ‘‘Reduce the convenience of nonmedical
exemptions only to the extent exempting is equalto the effort
required to vaccinate (or provide proof of vaccination)” and
‘‘Increase public education and awareness of the dangers of
vaccine-preventable disease and the benefits ofimmunization.”
[57].
Senate Bill 5005 (SB5005) was implemented in July 2011 and
required parents seeking an exemption to submit a ‘‘Certificate of
Exemption” or a letter signed by a licensed healthcare provider
(23) verifying that the provider has discussed the benefits/risks
of vaccines with the parent(s). However, parents who demonstrate
affiliation with a religious entity that does not permit medical
Table 2
French vaccination uptake figures for 2 years of age,2015 (Meningococus C 2016).Source: Sante Publique France,reproduced with permission.
Vaccine Introduction Status Coverage Rate Uptake and Compliance
DT Polio (3 doses) 1938; 1940; 1964 Required 98.9% Stable
Pertussis (3 doses) 1966 Recommended; vaccine combined with other antigens 98.6% Stable
Hib 1993 Recommended; vaccine combined with other antigens 98.0% Stable
Hepatitis B (3 doses) 1995 Recommended; vaccine combined with other antigens 88.1% 42% in 2007
Pneumococcal (3 doses) 2006 Recommended; not combined with other antigens 91.6% Increasing
MMR - 1st dose 1983 Recommended 90.5% Stable
MMR - 2nd dose 2005 Recommended 78.8% Increasing
Meningococcal C 2010 Recommended 70.90% Increasing
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 5
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019

treatment to children are exempted. This bill passed with the sup-
port of a substantial majority of both houses of the state legisla-
ture. While a substantially higher proportion of Democratic
legislators voted for this bill compared to their Republican peers,
there was still significant Republican support [58,59].
Support from local immunization groups,and state affiliates of
professional medical associations, such as the Washington chapter
of American Academy of Pediatrics, played a major role in generat-
ing support for this legislation.Moreover,Washington’s Vaccine
Advisory Committee – an advisory body comprised of professional
organizations,government agencies,and other healthcare stake-
holders – and local health departments supported this legislation.
After SB5005 was implemented,there was a relative decline of
more than 40% in nonmedical exemptions [56]. Moreover, with the
exception of Hepatitis B vaccine, state-level vaccine coverage
increased for all vaccines required for schoolentrance.Equally
importantly,SB5005 was associated with a decline in geographic
clustering of children with vaccine exemptions [56].
3.6.Germany
In West Germany,smallpox vaccination was mandatory until
1982. In East Germany,all childhood vaccines were mandatory,
but a generous list of medical contraindications was generally
interpreted to include religious objections. Following reunification
in 1990, all vaccines became voluntary. Vaccines recommended by
Germany’s Standing Committee of Vaccination,its technical advi-
sory body,are free of charge since they are covered by a universal
health insurance scheme (Table 1).
German vaccine coverage at school entry has been high; over
90% for all vaccines except hepatitis B. However, coverage in
younger children has been lower and variable across Germany’s
decentralised federal regions,demonstrating that children are not
being vaccinated in accordance with the vaccine schedule [60].
Attitudinal studies show that up to 18% of people are undecided
about vaccines and are rejecting some,such as varicella [61]. Ger-
many has repeatedly faced outbreaks of measles, including
amongst poorly reached migrant communities. This led to an
update of the National Action Plan for the Elimination Measles
and Rubella Elimination (2015) with all important stakeholders
involved and legal initiatives to improve vaccination coverage.
In 2015 the Federal Government passed the National Preventa-
tive Healthcare Act to strengthen health promotion.Parents now
have to provide evidence of routine check-ups, which include
counselling by a physician about vaccination, before their children
can attend daycare. This provision was tightened in July 2017 with
a requirement that kindergartens notify public health authorities if
parents have not provided the required evidence.Public health
authorities can then invite non-compliant parents for consulta-
tions or fine them up to€2500.A similar policy had already been
employed in some Länder,where it was associated with increased
vaccination coverage [62].
It is noteworthy that,as in Washington,the policy instrument
governing uptake penalises non-compliance with administrative
process,rather than vaccination.The policy therefore permits par-
ental rejection of vaccines,but only following counselling.It gov-
erns access (parents must visit a physician either way) and
governs acceptance with a focus on informed refusal. It also resem-
bles the Australian policy prior to ‘No Jab,No Pay,’although non-
compliance in Germany attracts sanctions rather than the loss of
entitlements or benefits.However,93% of German children aged
3–6 and 32% of children aged 0–3 are enrolled in daycare, meaning
that the sanctions should have a wide reach [63].Germans con-
tinue to debate the merits and disadvantages of mandatory vacci-
nation [64]. However, at present the strategy remains one of
enhancing trust, improving service delivery, filling adult immunity
gaps and utilising the daycare certificates.
4. Discussion
The new mandate instruments adopted by governments come
in a variety of shapes and sizes.Some govern vaccination itself;
others merely require rejecters to comply with administrative bur-
dens, which themselves can vary. Mandate instruments also oper-
ate across several dimensions that cannot be captured by merely
analysing written laws or regulations.The simplified continuum
we introduced earlier could be supplemented with additional axes,
relating to the severity of consequences for non-compliance,and
the intensity of enforcement.This would help us to consider the
complexity of how mandates operate.For example,fines for non-
compliance might seem like a severe outcome of refusal, but if they
are low and only applied once, then that particular mandate instru-
ment may prove less consequentialthan one which excludes
unvaccinated children from school for the duration of their educa-
tion. Likewise, a mandate that is not enforced (as was the case with
some European regimes prior to recent changes) might not really
‘exist’,although its presence likely affects social norms.
Politico-cultural context and vaccine policy history are also rel-
evant to governments’ decisions about vaccine mandates. East Ger-
many’s history ofoppressive state controlmay inform a unified
Germany’s current commitment to voluntarism.Meanwhile, the
phenomenon of path dependency can help to explain why other
jurisdictions in this study implemented mandatory systems build-
ing upon and modifying earlier regimes, and hence retaining differ-
ences with regard to target populations and instruments.Path
dependency illuminates how earlier decisions inform later ones,
directing decision-makers to continue down established pathways
[65].For example,Australia has a decades-old policy of providing
financial incentives to parents for their children’s vaccination sta-
tus from birth, which is one reason why its recent reforms focused
on this system of incentives,and therefore had impact on even
very young children.Meanwhile,the practice in the US of linking
vaccination to primary school entry is a primary reason why school
immunization requirements are the ‘obvious’site for mandatory
policy tightening in jurisdictions there,which results in policies
that cannot effect mass change on the vaccination coverage rates
of infants and toddlers.Path dependency can also inform publics’
levels of familiarity or comfort with mandates,emboldening poli-
cymakers to institute them.For example,the uncontroversial his-
tory of selective (and largely unenforced)vaccine mandates in
Italy and France may have primed the populace for their reinvigo-
ration in the face of measles outbreaks [1], even if this did generate
some vocalopposition.Australia also has compulsory voting for
Federal and State elections,suggesting some level of comfort with
compulsion that serves the collective there. Finally, it is also note-
worthy that public commitments to promote equality and eradi-
cate disadvantageinformed citizen consultation participants’
support for mandates in France, a country whose nationalist myths
centre on collective action and solidarity.
There are also distinctions in enforcementmechanisms and
agents responsible for enforcement between the mandate models
explored here. There is a comprehensive research program evident
even just focusing on the latter.Do health-care workers responsi-
ble for signing exemption forms work directly for the state or
receive arms-length subsidies? How does the state regulate their
actions with regard to reporting non-compliance? What about
the administrators of schools and daycare centres,now co-opted
as enforcement agents in some jurisdictions and required to pass
information about non-compliance to authorities? Clearly,there
are far greater level of complexity than we have the opportunity
6 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
port of a substantial majority of both houses of the state legisla-
ture. While a substantially higher proportion of Democratic
legislators voted for this bill compared to their Republican peers,
there was still significant Republican support [58,59].
Support from local immunization groups,and state affiliates of
professional medical associations, such as the Washington chapter
of American Academy of Pediatrics, played a major role in generat-
ing support for this legislation.Moreover,Washington’s Vaccine
Advisory Committee – an advisory body comprised of professional
organizations,government agencies,and other healthcare stake-
holders – and local health departments supported this legislation.
After SB5005 was implemented,there was a relative decline of
more than 40% in nonmedical exemptions [56]. Moreover, with the
exception of Hepatitis B vaccine, state-level vaccine coverage
increased for all vaccines required for schoolentrance.Equally
importantly,SB5005 was associated with a decline in geographic
clustering of children with vaccine exemptions [56].
3.6.Germany
In West Germany,smallpox vaccination was mandatory until
1982. In East Germany,all childhood vaccines were mandatory,
but a generous list of medical contraindications was generally
interpreted to include religious objections. Following reunification
in 1990, all vaccines became voluntary. Vaccines recommended by
Germany’s Standing Committee of Vaccination,its technical advi-
sory body,are free of charge since they are covered by a universal
health insurance scheme (Table 1).
German vaccine coverage at school entry has been high; over
90% for all vaccines except hepatitis B. However, coverage in
younger children has been lower and variable across Germany’s
decentralised federal regions,demonstrating that children are not
being vaccinated in accordance with the vaccine schedule [60].
Attitudinal studies show that up to 18% of people are undecided
about vaccines and are rejecting some,such as varicella [61]. Ger-
many has repeatedly faced outbreaks of measles, including
amongst poorly reached migrant communities. This led to an
update of the National Action Plan for the Elimination Measles
and Rubella Elimination (2015) with all important stakeholders
involved and legal initiatives to improve vaccination coverage.
In 2015 the Federal Government passed the National Preventa-
tive Healthcare Act to strengthen health promotion.Parents now
have to provide evidence of routine check-ups, which include
counselling by a physician about vaccination, before their children
can attend daycare. This provision was tightened in July 2017 with
a requirement that kindergartens notify public health authorities if
parents have not provided the required evidence.Public health
authorities can then invite non-compliant parents for consulta-
tions or fine them up to€2500.A similar policy had already been
employed in some Länder,where it was associated with increased
vaccination coverage [62].
It is noteworthy that,as in Washington,the policy instrument
governing uptake penalises non-compliance with administrative
process,rather than vaccination.The policy therefore permits par-
ental rejection of vaccines,but only following counselling.It gov-
erns access (parents must visit a physician either way) and
governs acceptance with a focus on informed refusal. It also resem-
bles the Australian policy prior to ‘No Jab,No Pay,’although non-
compliance in Germany attracts sanctions rather than the loss of
entitlements or benefits.However,93% of German children aged
3–6 and 32% of children aged 0–3 are enrolled in daycare, meaning
that the sanctions should have a wide reach [63].Germans con-
tinue to debate the merits and disadvantages of mandatory vacci-
nation [64]. However, at present the strategy remains one of
enhancing trust, improving service delivery, filling adult immunity
gaps and utilising the daycare certificates.
4. Discussion
The new mandate instruments adopted by governments come
in a variety of shapes and sizes.Some govern vaccination itself;
others merely require rejecters to comply with administrative bur-
dens, which themselves can vary. Mandate instruments also oper-
ate across several dimensions that cannot be captured by merely
analysing written laws or regulations.The simplified continuum
we introduced earlier could be supplemented with additional axes,
relating to the severity of consequences for non-compliance,and
the intensity of enforcement.This would help us to consider the
complexity of how mandates operate.For example,fines for non-
compliance might seem like a severe outcome of refusal, but if they
are low and only applied once, then that particular mandate instru-
ment may prove less consequentialthan one which excludes
unvaccinated children from school for the duration of their educa-
tion. Likewise, a mandate that is not enforced (as was the case with
some European regimes prior to recent changes) might not really
‘exist’,although its presence likely affects social norms.
Politico-cultural context and vaccine policy history are also rel-
evant to governments’ decisions about vaccine mandates. East Ger-
many’s history ofoppressive state controlmay inform a unified
Germany’s current commitment to voluntarism.Meanwhile, the
phenomenon of path dependency can help to explain why other
jurisdictions in this study implemented mandatory systems build-
ing upon and modifying earlier regimes, and hence retaining differ-
ences with regard to target populations and instruments.Path
dependency illuminates how earlier decisions inform later ones,
directing decision-makers to continue down established pathways
[65].For example,Australia has a decades-old policy of providing
financial incentives to parents for their children’s vaccination sta-
tus from birth, which is one reason why its recent reforms focused
on this system of incentives,and therefore had impact on even
very young children.Meanwhile,the practice in the US of linking
vaccination to primary school entry is a primary reason why school
immunization requirements are the ‘obvious’site for mandatory
policy tightening in jurisdictions there,which results in policies
that cannot effect mass change on the vaccination coverage rates
of infants and toddlers.Path dependency can also inform publics’
levels of familiarity or comfort with mandates,emboldening poli-
cymakers to institute them.For example,the uncontroversial his-
tory of selective (and largely unenforced)vaccine mandates in
Italy and France may have primed the populace for their reinvigo-
ration in the face of measles outbreaks [1], even if this did generate
some vocalopposition.Australia also has compulsory voting for
Federal and State elections,suggesting some level of comfort with
compulsion that serves the collective there. Finally, it is also note-
worthy that public commitments to promote equality and eradi-
cate disadvantageinformed citizen consultation participants’
support for mandates in France, a country whose nationalist myths
centre on collective action and solidarity.
There are also distinctions in enforcementmechanisms and
agents responsible for enforcement between the mandate models
explored here. There is a comprehensive research program evident
even just focusing on the latter.Do health-care workers responsi-
ble for signing exemption forms work directly for the state or
receive arms-length subsidies? How does the state regulate their
actions with regard to reporting non-compliance? What about
the administrators of schools and daycare centres,now co-opted
as enforcement agents in some jurisdictions and required to pass
information about non-compliance to authorities? Clearly,there
are far greater level of complexity than we have the opportunity
6 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

to elaborate here,demonstrating mandates’contextual specificity
and the need for further research in order to compare and contrast
their operation.
The stated driver for new mandates in every jurisdiction
explored in this article was concerns regarding vaccine refusal.
However,the mechanisms by which mandates became law varied
considerably.They ranged from a hastily executed emergency
decree (Italy) to a comprehensively designed consultation process
(France).Process matters for the ultimate legitimacy of mandates
policies to the broad populace (we recognise that there will always
be an element within society that remains vehemently opposed to
both vaccination and mandatory vaccination). French citizens were
prepared to relinquish their choice to the state (with a suite of pro-
tections),their trust likely enhanced by the state’s inclusion of
them in decision-making.
Further distinctions apparent here,such as the role of elected
officials versus bureaucrats as policy instigators, will be the subject
of future research.In their global overview of mandatory vaccina-
tion policies, MacDonald et al also draw attention to differences in
government level (evident here in our analyses of state and sub-
state units) and the question ofwhich vaccines are included in
the mandatory policy [6].Clearly,there are many more questions
to be asked and answered about mandatory vaccination policies.
5. Conclusion
Vaccine mandate instruments presenta variety of strategic
choices for policy makers. While vaccination social scientists worry
about the impact of mandates on public trust and attitudes [66],
mandates may be suitable for some scenarios. It is hard to critique
the consultative process that led to their temporary implementa-
tion in France, for example, nor to dispute states’ long-
established legitimacy to limit individualliberty for the benefit
of increased community health [1–3,67–70].However, whether
mandates are wise is a different question.
This question can be answered in part by considering whether
mandates work,and whether more restrictive mandates are more
effective than less restrictive mandates.We are not specifically
measuring effectiveness here – indeed it is too early in most cases
to do so. While studies of US school entry mandates indicate a
‘sweet spot’ in which stricter mandates with less accessible
exemptions result in improved coverage and reduced outbreaks
[10], it does not necessarily follow that restrictive mandates in
all jurisdictions will produce better coverage rates than less restric-
tive alternatives. Specifically, results may be confounded by differ-
ences (such as the severity of consequencesor strictness of
enforcement) which are only evident through forensic policy anal-
ysis and comparison.
This is closely related to the question ofnecessity.Although
mandates that impose negative consequences on vaccine refusers
are associated with lower refusal rates [10],it may be possible to
increase vaccination without imposing the most restrictive vaccine
mandate policies. For example, California’s AB 2109 was associated
with dramatic increases in immunization,though it did not elimi-
nate nonmedical exemptions, as did the later SB 277. Policymakers
may be subject to a ‘diligence heuristic’,believing that ‘tougher’
mandates deliver the goods [14],but more minimalist mandates
can avert social conflict and avoid unnecessary coercion.We sug-
gest that vaccine mandates should be accompanied by broader
efforts to increase public trust and support,and they should be
as minimally coercive as is necessary,otherwise they risk being
repealed,with significant harms to public health.
Another factor to consider is the importance of preventing
exemptions or punishments from becoming commodities. Analysts
are often concerned that mandates inordinately affect those with
less economic and socialcapital to get around or absorb them
[66]. If mandates enhance social inequality or do not change the
behavior of the wealthy, then they fail to achieve public health
goals and their legitimacy is undermined. It would be unfortunate
if poorly designed mandate instruments became embroiled in
ongoing debates about rising inequality occurring in many devel-
oped world jurisdictions.
It matters whether vaccine mandates work,but political and
ethical considerations matter,too; and these broader considera-
tions are not reducible to data about vaccination coverage. Vaccine
mandates are not only a population health instrument, but a polit-
ical one.We must study their continued evolution closely.
6. Declaration of interest
This research did not receive any specific grant from funding
agencies in the public,commercial,or not-for-profit sectors.KA
has previously received traveland accommodation funding from
GSK. She was previously employed by the Immunisation Alliance
of Western Australia to conduct vaccination social science research
funded by an unrestricted grant from Sanofi. PL reports grants from
Shionogi,grants and personal fees from GSK,grants and personal
fees from Pfizer, grants and personal fees from Sanofi, personal fees
from MSD, outside the submitted work.The other authors have
nothing to disclose.
References
[1] Lévy-Bruhl D et al. Extension of French vaccination mandates:from the
recommendation ofthe Steering Committee ofthe Citizen Consultation on
Vaccination to the law.Eurosurveillance 2018;23(17):18–00048.
[2] Gostin L, Wiley L. Public health law: power, duty, restraint. 3rd
ed. Oakland: California University of California Press; 2016.
[3] Goodman R. Law in public health practice. 2nd ed. New York: Oxford
University Press; 2007.
[4] Bedford H et al. Vaccine hesitancy,refusal and access barriers: the need for
clarity in terminology.Vaccine 2017.
[5] Dube E et al. Vaccine hesitancy: an overview.Human Vaccines Immunother
2013;9(8):1763–73.
[6] MacDonald NE et al.Mandatory infant & childhood immunization: rationales,
issues and knowledge gaps.Vaccine 2018.
[7] Legislators.N.c.o.S.States with religious and philosophicalexemptions from
school immunization requirements 2017 20/10/2017. Available from: <http://
www.ncsl.org/research/health/school-immunization-exemption-state-laws.
aspx> [cited 2017 23/11/2017].
[8] Assembly Bill 2109. Communicable disease: immunization exemption.
California Legislative Information California; 2012 [chapter 821].
[9] Buttenheim AM et al. Conditional admission,religious exemption type,and
nonmedicalvaccine exemptions in California before and after a state policy
change.Vaccine 2018;36(26):3789–93.
[10] Omer SB et al. Vaccination policies and rates of exemption from immunization,
2005–2011.New Eng J Med 2012;367(12):1170–1.
[11] Jones M et al.Mandatory health care provider counseling for parents led to a
decline in vaccine exemptions in California. Health Aff 2018;37(9):1494–502.
[12] Senate Bill 277 Public health: vaccinations.California Legislative Information
California; 2015.
[13] Pan R, Senate bill 277 introduced to end California’s vaccine exemption
loophole; 2015.
[14] Pan RJ.Restoring community immunity in America.Pediatrics 2018;141:1.
[15] EdSource.Schools consider impact of ending vaccination opt-outs; 2015.
[16] Anti-vaxxers have found a way around California’s strict new immunization
law. They need to be stopped in Los Angeles Times 2017.Los Angeles,United
States
[17] Legiscan.Roll Call: CA SB277 | 2015–2016 | California Senate Bill 277; 2015.
[18] Martinelli D et al. Are we ready to abrogate compulsory vaccinations for
children? Human Vaccines Immunother 2015;11(1):146–9.
[19] Aquino F et al. The web and public confidence in MMR vaccination in Italy.
Vaccine 2017;35(35):4494–8.
[20] Health, I.M.o. Vaccino e autismo,nessuna correlazione.I giudici ribaltano in
appello la sentenza del 2012; 2015.
[21] Giambi C et al. Parentalvaccine hesitancy in Italy – results from a national
survey.Vaccine 2018;36(6):779–87.
[22] Signorelli C et al. Childhood vaccine coverage in Italy after the new law on
mandatory immunization. Annali di igiene : medicina preventiva e di
comunità 2018;30(4 Supple 1):1–10.
[23] Istituto Superiore di Sanita.Morbillo e Rosolio News – Report n.37. Istituto
Superiore di Sanita; 2018
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 7
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
and the need for further research in order to compare and contrast
their operation.
The stated driver for new mandates in every jurisdiction
explored in this article was concerns regarding vaccine refusal.
However,the mechanisms by which mandates became law varied
considerably.They ranged from a hastily executed emergency
decree (Italy) to a comprehensively designed consultation process
(France).Process matters for the ultimate legitimacy of mandates
policies to the broad populace (we recognise that there will always
be an element within society that remains vehemently opposed to
both vaccination and mandatory vaccination). French citizens were
prepared to relinquish their choice to the state (with a suite of pro-
tections),their trust likely enhanced by the state’s inclusion of
them in decision-making.
Further distinctions apparent here,such as the role of elected
officials versus bureaucrats as policy instigators, will be the subject
of future research.In their global overview of mandatory vaccina-
tion policies, MacDonald et al also draw attention to differences in
government level (evident here in our analyses of state and sub-
state units) and the question ofwhich vaccines are included in
the mandatory policy [6].Clearly,there are many more questions
to be asked and answered about mandatory vaccination policies.
5. Conclusion
Vaccine mandate instruments presenta variety of strategic
choices for policy makers. While vaccination social scientists worry
about the impact of mandates on public trust and attitudes [66],
mandates may be suitable for some scenarios. It is hard to critique
the consultative process that led to their temporary implementa-
tion in France, for example, nor to dispute states’ long-
established legitimacy to limit individualliberty for the benefit
of increased community health [1–3,67–70].However, whether
mandates are wise is a different question.
This question can be answered in part by considering whether
mandates work,and whether more restrictive mandates are more
effective than less restrictive mandates.We are not specifically
measuring effectiveness here – indeed it is too early in most cases
to do so. While studies of US school entry mandates indicate a
‘sweet spot’ in which stricter mandates with less accessible
exemptions result in improved coverage and reduced outbreaks
[10], it does not necessarily follow that restrictive mandates in
all jurisdictions will produce better coverage rates than less restric-
tive alternatives. Specifically, results may be confounded by differ-
ences (such as the severity of consequencesor strictness of
enforcement) which are only evident through forensic policy anal-
ysis and comparison.
This is closely related to the question ofnecessity.Although
mandates that impose negative consequences on vaccine refusers
are associated with lower refusal rates [10],it may be possible to
increase vaccination without imposing the most restrictive vaccine
mandate policies. For example, California’s AB 2109 was associated
with dramatic increases in immunization,though it did not elimi-
nate nonmedical exemptions, as did the later SB 277. Policymakers
may be subject to a ‘diligence heuristic’,believing that ‘tougher’
mandates deliver the goods [14],but more minimalist mandates
can avert social conflict and avoid unnecessary coercion.We sug-
gest that vaccine mandates should be accompanied by broader
efforts to increase public trust and support,and they should be
as minimally coercive as is necessary,otherwise they risk being
repealed,with significant harms to public health.
Another factor to consider is the importance of preventing
exemptions or punishments from becoming commodities. Analysts
are often concerned that mandates inordinately affect those with
less economic and socialcapital to get around or absorb them
[66]. If mandates enhance social inequality or do not change the
behavior of the wealthy, then they fail to achieve public health
goals and their legitimacy is undermined. It would be unfortunate
if poorly designed mandate instruments became embroiled in
ongoing debates about rising inequality occurring in many devel-
oped world jurisdictions.
It matters whether vaccine mandates work,but political and
ethical considerations matter,too; and these broader considera-
tions are not reducible to data about vaccination coverage. Vaccine
mandates are not only a population health instrument, but a polit-
ical one.We must study their continued evolution closely.
6. Declaration of interest
This research did not receive any specific grant from funding
agencies in the public,commercial,or not-for-profit sectors.KA
has previously received traveland accommodation funding from
GSK. She was previously employed by the Immunisation Alliance
of Western Australia to conduct vaccination social science research
funded by an unrestricted grant from Sanofi. PL reports grants from
Shionogi,grants and personal fees from GSK,grants and personal
fees from Pfizer, grants and personal fees from Sanofi, personal fees
from MSD, outside the submitted work.The other authors have
nothing to disclose.
References
[1] Lévy-Bruhl D et al. Extension of French vaccination mandates:from the
recommendation ofthe Steering Committee ofthe Citizen Consultation on
Vaccination to the law.Eurosurveillance 2018;23(17):18–00048.
[2] Gostin L, Wiley L. Public health law: power, duty, restraint. 3rd
ed. Oakland: California University of California Press; 2016.
[3] Goodman R. Law in public health practice. 2nd ed. New York: Oxford
University Press; 2007.
[4] Bedford H et al. Vaccine hesitancy,refusal and access barriers: the need for
clarity in terminology.Vaccine 2017.
[5] Dube E et al. Vaccine hesitancy: an overview.Human Vaccines Immunother
2013;9(8):1763–73.
[6] MacDonald NE et al.Mandatory infant & childhood immunization: rationales,
issues and knowledge gaps.Vaccine 2018.
[7] Legislators.N.c.o.S.States with religious and philosophicalexemptions from
school immunization requirements 2017 20/10/2017. Available from: <http://
www.ncsl.org/research/health/school-immunization-exemption-state-laws.
aspx> [cited 2017 23/11/2017].
[8] Assembly Bill 2109. Communicable disease: immunization exemption.
California Legislative Information California; 2012 [chapter 821].
[9] Buttenheim AM et al. Conditional admission,religious exemption type,and
nonmedicalvaccine exemptions in California before and after a state policy
change.Vaccine 2018;36(26):3789–93.
[10] Omer SB et al. Vaccination policies and rates of exemption from immunization,
2005–2011.New Eng J Med 2012;367(12):1170–1.
[11] Jones M et al.Mandatory health care provider counseling for parents led to a
decline in vaccine exemptions in California. Health Aff 2018;37(9):1494–502.
[12] Senate Bill 277 Public health: vaccinations.California Legislative Information
California; 2015.
[13] Pan R, Senate bill 277 introduced to end California’s vaccine exemption
loophole; 2015.
[14] Pan RJ.Restoring community immunity in America.Pediatrics 2018;141:1.
[15] EdSource.Schools consider impact of ending vaccination opt-outs; 2015.
[16] Anti-vaxxers have found a way around California’s strict new immunization
law. They need to be stopped in Los Angeles Times 2017.Los Angeles,United
States
[17] Legiscan.Roll Call: CA SB277 | 2015–2016 | California Senate Bill 277; 2015.
[18] Martinelli D et al. Are we ready to abrogate compulsory vaccinations for
children? Human Vaccines Immunother 2015;11(1):146–9.
[19] Aquino F et al. The web and public confidence in MMR vaccination in Italy.
Vaccine 2017;35(35):4494–8.
[20] Health, I.M.o. Vaccino e autismo,nessuna correlazione.I giudici ribaltano in
appello la sentenza del 2012; 2015.
[21] Giambi C et al. Parentalvaccine hesitancy in Italy – results from a national
survey.Vaccine 2018;36(6):779–87.
[22] Signorelli C et al. Childhood vaccine coverage in Italy after the new law on
mandatory immunization. Annali di igiene : medicina preventiva e di
comunità 2018;30(4 Supple 1):1–10.
[23] Istituto Superiore di Sanita.Morbillo e Rosolio News – Report n.37. Istituto
Superiore di Sanita; 2018
K. Attwell et al. / Vaccine xxx (2018) xxx–xxx 7
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (20
https://doi.org/10.1016/j.vaccine.2018.10.019
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

[24] Paterlini M. Italy suspends mandatory vaccination of nursery children after
Senate vote.BMJ 2018;362.
[25] Day M. Doctor and MPs in Italy are assaulted after vaccination law is passed.
BMJ: British Med J (Online) 2017:358.
[26] Bucchi M. La vittoria dei pro-vax: raddoppiati gli italiani che credono alla
scienza 2017,<http://www.repubblica.it/scienze>.
[27] Gualano MR et al.Attitudes towards compulsory vaccination in Italy: results
from the NAVIDAD multicentre study.Vaccine 2018;36(23):3368–74.
[28] LegiFrance.Loi n 2007-293 du 5 mars 2007 Réformant la Protection de
l’Enfance – Missions de la Protection de l’Enfance.2007: France
[29] Sante Publique. Synthèse des couvertures vaccinales chez l’enfant de 2 ans. N.
D. [cited 2018 1 October]; Available from: http://invs.santepubliquefrance.fr/
Dossiers-thematiques/Maladies-infectieuses/Maladies-a-prevention-
vaccinale/Couverture-vaccinale/Donnees/Synthese-des-couvertures-
vaccinales-chez-l-enfant-de-2-ans.
[30] Gautier A, Chemlal K, Jestin C. Adhesion à la vaccination en France: résultats du
Baromètre santé 2016 [Acceptance of Immunization in France: results from
the 2016 Health Barometer]. Bull Epidemiologique Hebdomadaire 2017;
October 19:21–7.
[31] Ministère des affaires sociales de la santé et des droits des femmes France,
Rapport sur la politique vaccinale.France; 2016.
[32] Citizen Consultation on Vaccination, F. Présentation du plan d’action pour une
rénovation de la politique vaccinale en France 2016 30/11/2017]; Available
from: http://concertation-vaccination.fr/.
[33] Santé publique France,Vaccination des jeunes enfants – des données pour
mieux comprendre.2017: France
[34] Le Conseil D’Etat et la Juridiction Administrative, Vaccination obligatoire.
2017.
[35] Assemblée Nationale France, Projet de loi de financement de la sécurité sociale
pour 2018 (Texte définitif).2017: France
[36] Ward JK, Colgrove J, Verger P. Why France is making eight new vaccines
mandatory.Vaccine 2018;36(14):1801–3.
[37] Yang YT, Reiss DR. French mandatory vaccine policy. Vaccine 2018;36
(11):1323–5.
[38] Department of Health Australia,National Immunisation Strategy for Australia
2013–2018.Australia; 2013.
[39] Ward K, Hull B, Leask J.Financial incentives for childhood immunisation – a
unique but changing Australian initiative.Med J Aust 2013.198(11)..
[40] National Health Performance Authority,Healthy Communities.Immunisation
rates for children in 2012–13. Australia: National Health Performance
Authority; 2014.
[41] Chow MYK et al.Parental attitudes,beliefs,behaviours and concerns towards
childhood vaccinations in Australia: a national online survey. Aust Fam
Physician 2017;46(3):145–51.
[42] Hansen J. No jab, no play campaign reveals vaccination refusals high as babies
die, in Daily Telegraph 2013.
[43] ABC Radio,No-jab, no pay laws to be strengthened if new bill passes; 2017.
[44] Parliament of Australia,Social Services Legislation Amendment (No Jab,No
Pay) Bill 2015 Explanatory Memorandum 2015.
[45] Abbott T.Prime Minister Tony Abbott announces ‘no jab,no play and no pay’
policy for child vaccination,in The Daily Telegraph 2015.
[46] Department of Health Australia. No Jab No Pay Factsheet – New Immunisation
Requirements for Family Assistance Payments; 2015.
[47] Senate Community Affairs Legislation Committee. Official Committee Hansard
Senate Community Affairs Legislation Committee – Social Services Legislation
Amendment (No Jab No Pay) Bill 2015.Australia
[48] Parliament of Australia.Social Services Legislation Amendment (No Jab,No
Pay) Bill 2015: Australia.p. 7.
[49] Department of Education Australia, The new child care package brochure. 2017.
[50] Statistics A.B.o.4402.0 – Childhood Education and Care in Australia; 2014.
[51] Aly W, In opposing the anti-vaccination movement,a sledgehammer cannot
win battle of the needle,in The Sydney Morning Herald 2015.
[52] National Health Performance Authority, Healthy Communities: Immunisation
Rates for Children in 2015–16.2017,National Health Performance Authority:
Sydney,NSW.
[53] Porter C. No Jab, No Pay lifts immunisation rates [Media Release],Human
Services,Editor. Canberra: Commonwealth of Australia; 2016.
[54] National Centre for Immunisation Research and Surveillance.No Jab No Play,
No Jab No Pay Policies – national and state legislation 2017 30/11/2017];
Available from: http://www.ncirs.edu.au/consumer-resources/no-jab-no-
play-no-jab-no-pay-policies/.
[55] Omer SB et al. Nonmedical exemptions to school immunization requirements:
secular trends and association of state policies with pertussis incidence. JAMA
2006;296(14):1757–63.
[56] Omer S et al. Exemptions from mandatory immunization after legally
mandated parental counseling.Pediatrics 2018;141:1.
[57] Department of Health. Agency Request Legislation Proposal: Exemptions from
immunizations required for schools and childcare centers, D.o. Health,
Editor. Washington (US): Department of Health; 2011.
[58] Washington State Legislature.House Roll Call on 2011 Senate Bill 5005:
Certification of exemption from immunization.
[59] Washington State Legislature,Senate Roll Call on 2011 Senate Bill 5005:
Certification of exemption from immunization.2011..
[60] VacMap- Measles Vaccination Coverage in Germany G. Federal Health
Ministry, editor; 2017.
[61] Horstkötter N.,et al. Einstellungen,Wissen und Verhalten von Erwachsenen
und Eltern gegenüber Impfungen – Ergebnisse der Repräsentativbefragung
2016 zum Infektionsschutz. 2017, BZgA-Forschungsbericht. Köln:
Bundeszentrale für gesundheitliche Aufklärung 2017: Germany
[62] Robert Koch Institut. Epidemiologisches Bulletin. Robert Koch Institut; 2011. p.
49–53.
[63] Statistisches Bundesamt (destatis). Statistisches Jahrbuch 2017 2017,
Statistisches Bundesamt (destatis).
[64] Online, Z. Wer die Eltern entscheiden lässt,riskiert Menschenleben in Zeit
Online 2017.
[65] Pierson P.Increasing returns,path dependence,and the study of politics.Am
Political Sci Rev 2000;94(2):251–67.
[66] Leask J,Danchin M. Imposing penalties for vaccine rejection requires strong
scrutiny.J Paediatr Child Health 2017;53(5):439–44.
[67] Zeigler K.E.Cicero: De Legibus 1963,Heidelberg
[68] Locke J. Second treatise of government and a letter concerning
toleration.United Kingdom: Oxford University Press; 2016.
[69] United Nations Universal Declaration Human Rights U. Nations, editor.
Geneva; 1948
[70] International Covenant Civiland Political Rights U. Nations, editor. Geneva;
1966.
8 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
Senate vote.BMJ 2018;362.
[25] Day M. Doctor and MPs in Italy are assaulted after vaccination law is passed.
BMJ: British Med J (Online) 2017:358.
[26] Bucchi M. La vittoria dei pro-vax: raddoppiati gli italiani che credono alla
scienza 2017,<http://www.repubblica.it/scienze>.
[27] Gualano MR et al.Attitudes towards compulsory vaccination in Italy: results
from the NAVIDAD multicentre study.Vaccine 2018;36(23):3368–74.
[28] LegiFrance.Loi n 2007-293 du 5 mars 2007 Réformant la Protection de
l’Enfance – Missions de la Protection de l’Enfance.2007: France
[29] Sante Publique. Synthèse des couvertures vaccinales chez l’enfant de 2 ans. N.
D. [cited 2018 1 October]; Available from: http://invs.santepubliquefrance.fr/
Dossiers-thematiques/Maladies-infectieuses/Maladies-a-prevention-
vaccinale/Couverture-vaccinale/Donnees/Synthese-des-couvertures-
vaccinales-chez-l-enfant-de-2-ans.
[30] Gautier A, Chemlal K, Jestin C. Adhesion à la vaccination en France: résultats du
Baromètre santé 2016 [Acceptance of Immunization in France: results from
the 2016 Health Barometer]. Bull Epidemiologique Hebdomadaire 2017;
October 19:21–7.
[31] Ministère des affaires sociales de la santé et des droits des femmes France,
Rapport sur la politique vaccinale.France; 2016.
[32] Citizen Consultation on Vaccination, F. Présentation du plan d’action pour une
rénovation de la politique vaccinale en France 2016 30/11/2017]; Available
from: http://concertation-vaccination.fr/.
[33] Santé publique France,Vaccination des jeunes enfants – des données pour
mieux comprendre.2017: France
[34] Le Conseil D’Etat et la Juridiction Administrative, Vaccination obligatoire.
2017.
[35] Assemblée Nationale France, Projet de loi de financement de la sécurité sociale
pour 2018 (Texte définitif).2017: France
[36] Ward JK, Colgrove J, Verger P. Why France is making eight new vaccines
mandatory.Vaccine 2018;36(14):1801–3.
[37] Yang YT, Reiss DR. French mandatory vaccine policy. Vaccine 2018;36
(11):1323–5.
[38] Department of Health Australia,National Immunisation Strategy for Australia
2013–2018.Australia; 2013.
[39] Ward K, Hull B, Leask J.Financial incentives for childhood immunisation – a
unique but changing Australian initiative.Med J Aust 2013.198(11)..
[40] National Health Performance Authority,Healthy Communities.Immunisation
rates for children in 2012–13. Australia: National Health Performance
Authority; 2014.
[41] Chow MYK et al.Parental attitudes,beliefs,behaviours and concerns towards
childhood vaccinations in Australia: a national online survey. Aust Fam
Physician 2017;46(3):145–51.
[42] Hansen J. No jab, no play campaign reveals vaccination refusals high as babies
die, in Daily Telegraph 2013.
[43] ABC Radio,No-jab, no pay laws to be strengthened if new bill passes; 2017.
[44] Parliament of Australia,Social Services Legislation Amendment (No Jab,No
Pay) Bill 2015 Explanatory Memorandum 2015.
[45] Abbott T.Prime Minister Tony Abbott announces ‘no jab,no play and no pay’
policy for child vaccination,in The Daily Telegraph 2015.
[46] Department of Health Australia. No Jab No Pay Factsheet – New Immunisation
Requirements for Family Assistance Payments; 2015.
[47] Senate Community Affairs Legislation Committee. Official Committee Hansard
Senate Community Affairs Legislation Committee – Social Services Legislation
Amendment (No Jab No Pay) Bill 2015.Australia
[48] Parliament of Australia.Social Services Legislation Amendment (No Jab,No
Pay) Bill 2015: Australia.p. 7.
[49] Department of Education Australia, The new child care package brochure. 2017.
[50] Statistics A.B.o.4402.0 – Childhood Education and Care in Australia; 2014.
[51] Aly W, In opposing the anti-vaccination movement,a sledgehammer cannot
win battle of the needle,in The Sydney Morning Herald 2015.
[52] National Health Performance Authority, Healthy Communities: Immunisation
Rates for Children in 2015–16.2017,National Health Performance Authority:
Sydney,NSW.
[53] Porter C. No Jab, No Pay lifts immunisation rates [Media Release],Human
Services,Editor. Canberra: Commonwealth of Australia; 2016.
[54] National Centre for Immunisation Research and Surveillance.No Jab No Play,
No Jab No Pay Policies – national and state legislation 2017 30/11/2017];
Available from: http://www.ncirs.edu.au/consumer-resources/no-jab-no-
play-no-jab-no-pay-policies/.
[55] Omer SB et al. Nonmedical exemptions to school immunization requirements:
secular trends and association of state policies with pertussis incidence. JAMA
2006;296(14):1757–63.
[56] Omer S et al. Exemptions from mandatory immunization after legally
mandated parental counseling.Pediatrics 2018;141:1.
[57] Department of Health. Agency Request Legislation Proposal: Exemptions from
immunizations required for schools and childcare centers, D.o. Health,
Editor. Washington (US): Department of Health; 2011.
[58] Washington State Legislature.House Roll Call on 2011 Senate Bill 5005:
Certification of exemption from immunization.
[59] Washington State Legislature,Senate Roll Call on 2011 Senate Bill 5005:
Certification of exemption from immunization.2011..
[60] VacMap- Measles Vaccination Coverage in Germany G. Federal Health
Ministry, editor; 2017.
[61] Horstkötter N.,et al. Einstellungen,Wissen und Verhalten von Erwachsenen
und Eltern gegenüber Impfungen – Ergebnisse der Repräsentativbefragung
2016 zum Infektionsschutz. 2017, BZgA-Forschungsbericht. Köln:
Bundeszentrale für gesundheitliche Aufklärung 2017: Germany
[62] Robert Koch Institut. Epidemiologisches Bulletin. Robert Koch Institut; 2011. p.
49–53.
[63] Statistisches Bundesamt (destatis). Statistisches Jahrbuch 2017 2017,
Statistisches Bundesamt (destatis).
[64] Online, Z. Wer die Eltern entscheiden lässt,riskiert Menschenleben in Zeit
Online 2017.
[65] Pierson P.Increasing returns,path dependence,and the study of politics.Am
Political Sci Rev 2000;94(2):251–67.
[66] Leask J,Danchin M. Imposing penalties for vaccine rejection requires strong
scrutiny.J Paediatr Child Health 2017;53(5):439–44.
[67] Zeigler K.E.Cicero: De Legibus 1963,Heidelberg
[68] Locke J. Second treatise of government and a letter concerning
toleration.United Kingdom: Oxford University Press; 2016.
[69] United Nations Universal Declaration Human Rights U. Nations, editor.
Geneva; 1948
[70] International Covenant Civiland Political Rights U. Nations, editor. Geneva;
1966.
8 K. Attwell et al. / Vaccine xxx (2018) xxx–xxx
Please cite this article in press as: Attwell K et al. Recent vaccine mandates in the United States, Europe and Australia: A comparative study. Vaccine (2018
https://doi.org/10.1016/j.vaccine.2018.10.019
1 out of 8
Your All-in-One AI-Powered Toolkit for Academic Success.
+13062052269
info@desklib.com
Available 24*7 on WhatsApp / Email
![[object Object]](/_next/static/media/star-bottom.7253800d.svg)
Unlock your academic potential
Copyright © 2020–2026 A2Z Services. All Rights Reserved. Developed and managed by ZUCOL.
