University Name - Case Study: Pneumonia and Elderly Patient Care
VerifiedAdded on 2021/06/16
|16
|4725
|35
Case Study
AI Summary
This case study focuses on Mr. Hunter, an 89-year-old patient with pneumonia. It explores the specific considerations for registered nurses in understanding the clinical manifestations of pneumonia in the elderly, including antimicrobial selection, aetiology, and risk factors. The assignment outlines the pathophysiology of altered ventilation and diffusion, differentiates between community-acquired pneumonia (CAP), hospital-acquired pneumonia (HAP), and aspiration pneumonia. Furthermore, it details the required nursing care, providing rationales for all elements, and explains the rationale for monitoring specific parameters like heart rate, oxygen saturation, and body temperature. Finally, it addresses strategies for ensuring patient understanding of treatment implications, such as refusal of oxygen, and provides an overview of medication administration and patient education.

Case Study 1
CONTEXTS OF PRACTICE: HEALTH ALTERATION CASE STUDY
By (Name)
Course
Professor’s name
University name
City, State
Date of submission
CONTEXTS OF PRACTICE: HEALTH ALTERATION CASE STUDY
By (Name)
Course
Professor’s name
University name
City, State
Date of submission
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

CASE STUDY 2
Assignment
1) Mr Hunter is 89 years old. What are the specific considerations a Registered Nurse
should understand in relation to the clinical manifestations of pneumonia in the
older person?
Antimicrobial selection: A registered nurse should understand that for elderly patients
(in this case, Mr Hunter) with community-acquired pneumonia, the antimicrobial selection is
similar to that of all adults with confirmed community-acquired pneumonia (Williams et al.
2017). So, recommendations for influenza and pneumococcal vaccines in individuals with
advanced age are included as part of the recommendations provided on community-acquired
pneumonia prevention (Sader et al. 2014). According to Williams et al. (2017), in the United
States, of the major causes of demise in the elderly who are above 65 years, community-
acquired pneumonia is ranked 5th. A distinct subpopulation of elderly individuals and
residents of facilities that offer long-term care are at profoundly lofty level risk of developing
pneumonia (Blot et al. 2014).
Aetiology: In relation to Mr Hunter's case, a registered nurse should be able to
understand the aetiology of pneumonia, in connection with its clinical manifestation in an
elderly person. However, Troeger et al. (2017) note that determining the relative significance
of different aetiologies of this disease in the older subpopulation is rather challenging. S.
pneumoniae is the etiologic agent in approximately 48% of individuals above 60 years of age
according to a Finnish study which involved 345 episodes of community-acquired
pneumonia. In the same study, C. pneumoniae was responsible for 12% of the cases while M.
pneumoniae was detected in 10% of the cases. H. influenza was responsible for 4% of the
cases while respiratory viruses were detected in 10% of the cases (Lee et al. 2017). The
incidence of pneumonia caused by gram-negative bacteria in the elderly subpopulation is
Assignment
1) Mr Hunter is 89 years old. What are the specific considerations a Registered Nurse
should understand in relation to the clinical manifestations of pneumonia in the
older person?
Antimicrobial selection: A registered nurse should understand that for elderly patients
(in this case, Mr Hunter) with community-acquired pneumonia, the antimicrobial selection is
similar to that of all adults with confirmed community-acquired pneumonia (Williams et al.
2017). So, recommendations for influenza and pneumococcal vaccines in individuals with
advanced age are included as part of the recommendations provided on community-acquired
pneumonia prevention (Sader et al. 2014). According to Williams et al. (2017), in the United
States, of the major causes of demise in the elderly who are above 65 years, community-
acquired pneumonia is ranked 5th. A distinct subpopulation of elderly individuals and
residents of facilities that offer long-term care are at profoundly lofty level risk of developing
pneumonia (Blot et al. 2014).
Aetiology: In relation to Mr Hunter's case, a registered nurse should be able to
understand the aetiology of pneumonia, in connection with its clinical manifestation in an
elderly person. However, Troeger et al. (2017) note that determining the relative significance
of different aetiologies of this disease in the older subpopulation is rather challenging. S.
pneumoniae is the etiologic agent in approximately 48% of individuals above 60 years of age
according to a Finnish study which involved 345 episodes of community-acquired
pneumonia. In the same study, C. pneumoniae was responsible for 12% of the cases while M.
pneumoniae was detected in 10% of the cases. H. influenza was responsible for 4% of the
cases while respiratory viruses were detected in 10% of the cases (Lee et al. 2017). The
incidence of pneumonia caused by gram-negative bacteria in the elderly subpopulation is

CASE STUDY 3
rather uncertain and, information is scanty for nursing home residents. Usually, the detection
of Mycoplasma and Legionella species is infrequent (Song et al. 2016).
Risk factors: For pneumonia, according to Zhuge et al. (2018), independent risk
factors include alcoholism, immunosuppression, bronchial asthma, heart disease, lung disease
and advancing age. Other significant factors include difficulty swallowing and being male
(Prina et al. 2015).
2) Outline the pathophysiology of altered ventilation and diffusion in relation to Mr
Hunter's pneumonia.
According to Sa et al. (2017), the interrelation between ventilation and diffusion is a
balance between oxygen entry into the alveoli and subsequently into blood. Ventilation is the
process by which oxygen enters into the air sacks and the exit of carbon dioxide out of the
alveoli. Diffusion in itself is the process by which oxygen gets into the blood from the air
sacks as co2 replaces it in the alveoli (Sa et al. 2017). Thus, the carbon dioxide and oxygen
levels are altered by these two processes. An alteration in these processes arises when there is
a change in any of the two takes place (Liu et al. 2016).
Sa et al. (2017) contends that there is a little but substantive increase in the degree of
ventilation: diffusion mismatch which develops in pneumonia. The cause of this mismatch is
unknown but hypothesises have pointed out to interstitial oedema which develops as a result
of inflammation of the lung parenchyma, reduced gaseous exchange in large airways,
regional differences in the way blood flows in the lungs, pulmonary haemorrhage and airway
obstruction (Liu et al. 2016).
3) What are the differences between community-acquired pneumonia (CAP), hospital-
acquired pneumonia (HAP) and aspiration pneumonia?
rather uncertain and, information is scanty for nursing home residents. Usually, the detection
of Mycoplasma and Legionella species is infrequent (Song et al. 2016).
Risk factors: For pneumonia, according to Zhuge et al. (2018), independent risk
factors include alcoholism, immunosuppression, bronchial asthma, heart disease, lung disease
and advancing age. Other significant factors include difficulty swallowing and being male
(Prina et al. 2015).
2) Outline the pathophysiology of altered ventilation and diffusion in relation to Mr
Hunter's pneumonia.
According to Sa et al. (2017), the interrelation between ventilation and diffusion is a
balance between oxygen entry into the alveoli and subsequently into blood. Ventilation is the
process by which oxygen enters into the air sacks and the exit of carbon dioxide out of the
alveoli. Diffusion in itself is the process by which oxygen gets into the blood from the air
sacks as co2 replaces it in the alveoli (Sa et al. 2017). Thus, the carbon dioxide and oxygen
levels are altered by these two processes. An alteration in these processes arises when there is
a change in any of the two takes place (Liu et al. 2016).
Sa et al. (2017) contends that there is a little but substantive increase in the degree of
ventilation: diffusion mismatch which develops in pneumonia. The cause of this mismatch is
unknown but hypothesises have pointed out to interstitial oedema which develops as a result
of inflammation of the lung parenchyma, reduced gaseous exchange in large airways,
regional differences in the way blood flows in the lungs, pulmonary haemorrhage and airway
obstruction (Liu et al. 2016).
3) What are the differences between community-acquired pneumonia (CAP), hospital-
acquired pneumonia (HAP) and aspiration pneumonia?
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

CASE STUDY 4
HAP: Also, referred to as nosocomial pneumonia. This is pneumonia contracted in the
hospital by a patient, at least 48-72 hours after admission (Komiya, Ishii & Kadota).
According to Pugh et al. (2015), usually, it is caused by a bacterial infection and hardly by a
viral infection. Ewan et al. (2017) note that of all healthcare-associated pneumonia (HCAP),
nosocomial infection comes second after urinary tract infections, accounting for 15-20% of
the cases. Moreover, HAP is the major cause of demise of the nosocomial infections,
particularly in the intensive care units. The signs and symptoms of HAP, particularly for
elderly patients include confusion or mental changes, cough with greenish sputum, chills and
fever, malaise, nausea, vomiting, lack of appetite, chest pain that is sharp and often getting
worse with coughing and deep breathing, dyspnoea, fast heart rate and significant decrease in
blood pressure (Ewan et al. 2017). A diagnosis of hospital-acquired pneumonia is based on
the clinical presentation and the picture of the patient's x-ray film and, elevated leukocyte
count (El-Rabbany et al. 2015). The differential diagnosis for HAP includes atelectasis,
pulmonary embolism and congestive heart failure. Regarding its treatment, the initial therapy
is usually empirical (El-Rabbany et al. 2015).
CAP: This is a type of pneumonia contracted by persons with little or no direct
contact with healthcare settings, particularly medical institutions. S. pneumonia is the most
common etiologic agent identified with CAP. Other pathogens that are often responsible for
CAP include atypical bacteria (M. pneumoniae, C. pneumoniae, Legionella species), H.
influenza and viruses (Troeger et al. 2017). The signs and symptoms associated with this type
of pneumonia include a cough, fever, production of sputum, dyspnoea, pleuritic chest pain,
tachycardia and tachypnea (Marti & Esperatti 2016). In diagnosing CAP, the patient’s clinical
presentation and the picture of the patient's x-ray film are important. Antibiotics that have
been empirically chosen are used in the treatment of CAP. For relatively healthy or young
patients, this type of pneumonia has an excellent prognosis (Marti & Esperatti 2016).
HAP: Also, referred to as nosocomial pneumonia. This is pneumonia contracted in the
hospital by a patient, at least 48-72 hours after admission (Komiya, Ishii & Kadota).
According to Pugh et al. (2015), usually, it is caused by a bacterial infection and hardly by a
viral infection. Ewan et al. (2017) note that of all healthcare-associated pneumonia (HCAP),
nosocomial infection comes second after urinary tract infections, accounting for 15-20% of
the cases. Moreover, HAP is the major cause of demise of the nosocomial infections,
particularly in the intensive care units. The signs and symptoms of HAP, particularly for
elderly patients include confusion or mental changes, cough with greenish sputum, chills and
fever, malaise, nausea, vomiting, lack of appetite, chest pain that is sharp and often getting
worse with coughing and deep breathing, dyspnoea, fast heart rate and significant decrease in
blood pressure (Ewan et al. 2017). A diagnosis of hospital-acquired pneumonia is based on
the clinical presentation and the picture of the patient's x-ray film and, elevated leukocyte
count (El-Rabbany et al. 2015). The differential diagnosis for HAP includes atelectasis,
pulmonary embolism and congestive heart failure. Regarding its treatment, the initial therapy
is usually empirical (El-Rabbany et al. 2015).
CAP: This is a type of pneumonia contracted by persons with little or no direct
contact with healthcare settings, particularly medical institutions. S. pneumonia is the most
common etiologic agent identified with CAP. Other pathogens that are often responsible for
CAP include atypical bacteria (M. pneumoniae, C. pneumoniae, Legionella species), H.
influenza and viruses (Troeger et al. 2017). The signs and symptoms associated with this type
of pneumonia include a cough, fever, production of sputum, dyspnoea, pleuritic chest pain,
tachycardia and tachypnea (Marti & Esperatti 2016). In diagnosing CAP, the patient’s clinical
presentation and the picture of the patient's x-ray film are important. Antibiotics that have
been empirically chosen are used in the treatment of CAP. For relatively healthy or young
patients, this type of pneumonia has an excellent prognosis (Marti & Esperatti 2016).
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

CASE STUDY 5
However, a good number of cases of pneumonia, particularly when the aetiological agent in
question is S. pneumonia, S. aureus, Legionella or influenza viruses, are much serious and
often fatal in sicker patients and the elderly subpopulation (Musher & Thorner 2014).
Aspiration pneumonia: This type occurs when saliva, vomit, liquids, food or liquid is
breathed via the air passages to the lungs, instead of being swallowed through the oesophagus
into the stomach (Dibardino & Wunderick 2015). The risk factors for aspirating these things
into the lungs include being comatose, alcoholism, being less alert because of illness, drugs
or other causes, old age, general anaesthesia, challenges with swallowing and poor gag reflex
in semi-conscious or unconscious people often after brain injury or stroke (Muller 2015).
Dibardino and Wunderink (2015) note that the symptoms for aspiration pneumonia include
chest pain, fatigue, coughing up dark/greenish and foul-smelling sputum, fever, wheezing,
shortness of breath, breath odour, problems swallowing and excessive sweating. Its treatment
depends on the severity of pneumonia itself and, how ill an individual was before the
aspiration (Dibardino & Wunderink 2015). As Muller (2015) notes, a ventilator is sometimes
needed to support breathing. The patients are given antibiotics and for the patients with
swallowing difficulties, other feeding methods are used to reduce the aspiration risks (Muller
2015).
4) Explain the nursing care required by a patient with pneumonia. Provide a rationale
for all elements of the care provided that reflects the particular needs of Mr Hunter.
For all patients with pneumonia, nursing care would include supportive measures to
eliminate hypoxemia like humidified oxygen therapy, ventilator support for respiratory
failure, adequate intake of fluids and a diet with high caloric content (Nuti et al. 2015).
According to Richards et al. (2017), nursing interventions such as bed rest and analgesic
administration to relieve sharp chest pain are included. Nuti et al. (2015) assert that the
However, a good number of cases of pneumonia, particularly when the aetiological agent in
question is S. pneumonia, S. aureus, Legionella or influenza viruses, are much serious and
often fatal in sicker patients and the elderly subpopulation (Musher & Thorner 2014).
Aspiration pneumonia: This type occurs when saliva, vomit, liquids, food or liquid is
breathed via the air passages to the lungs, instead of being swallowed through the oesophagus
into the stomach (Dibardino & Wunderick 2015). The risk factors for aspirating these things
into the lungs include being comatose, alcoholism, being less alert because of illness, drugs
or other causes, old age, general anaesthesia, challenges with swallowing and poor gag reflex
in semi-conscious or unconscious people often after brain injury or stroke (Muller 2015).
Dibardino and Wunderink (2015) note that the symptoms for aspiration pneumonia include
chest pain, fatigue, coughing up dark/greenish and foul-smelling sputum, fever, wheezing,
shortness of breath, breath odour, problems swallowing and excessive sweating. Its treatment
depends on the severity of pneumonia itself and, how ill an individual was before the
aspiration (Dibardino & Wunderink 2015). As Muller (2015) notes, a ventilator is sometimes
needed to support breathing. The patients are given antibiotics and for the patients with
swallowing difficulties, other feeding methods are used to reduce the aspiration risks (Muller
2015).
4) Explain the nursing care required by a patient with pneumonia. Provide a rationale
for all elements of the care provided that reflects the particular needs of Mr Hunter.
For all patients with pneumonia, nursing care would include supportive measures to
eliminate hypoxemia like humidified oxygen therapy, ventilator support for respiratory
failure, adequate intake of fluids and a diet with high caloric content (Nuti et al. 2015).
According to Richards et al. (2017), nursing interventions such as bed rest and analgesic
administration to relieve sharp chest pain are included. Nuti et al. (2015) assert that the
CASE STUDY 6
nursing care plans for pneumonia include impaired gas exchange, acute pain, ineffective
airway clearance, activity intolerance, deficient knowledge, hyperthermia, the risk for
imbalanced nutrition, risk for deficient fluid volume, risk for infection, ineffective breathing
patterns among others.
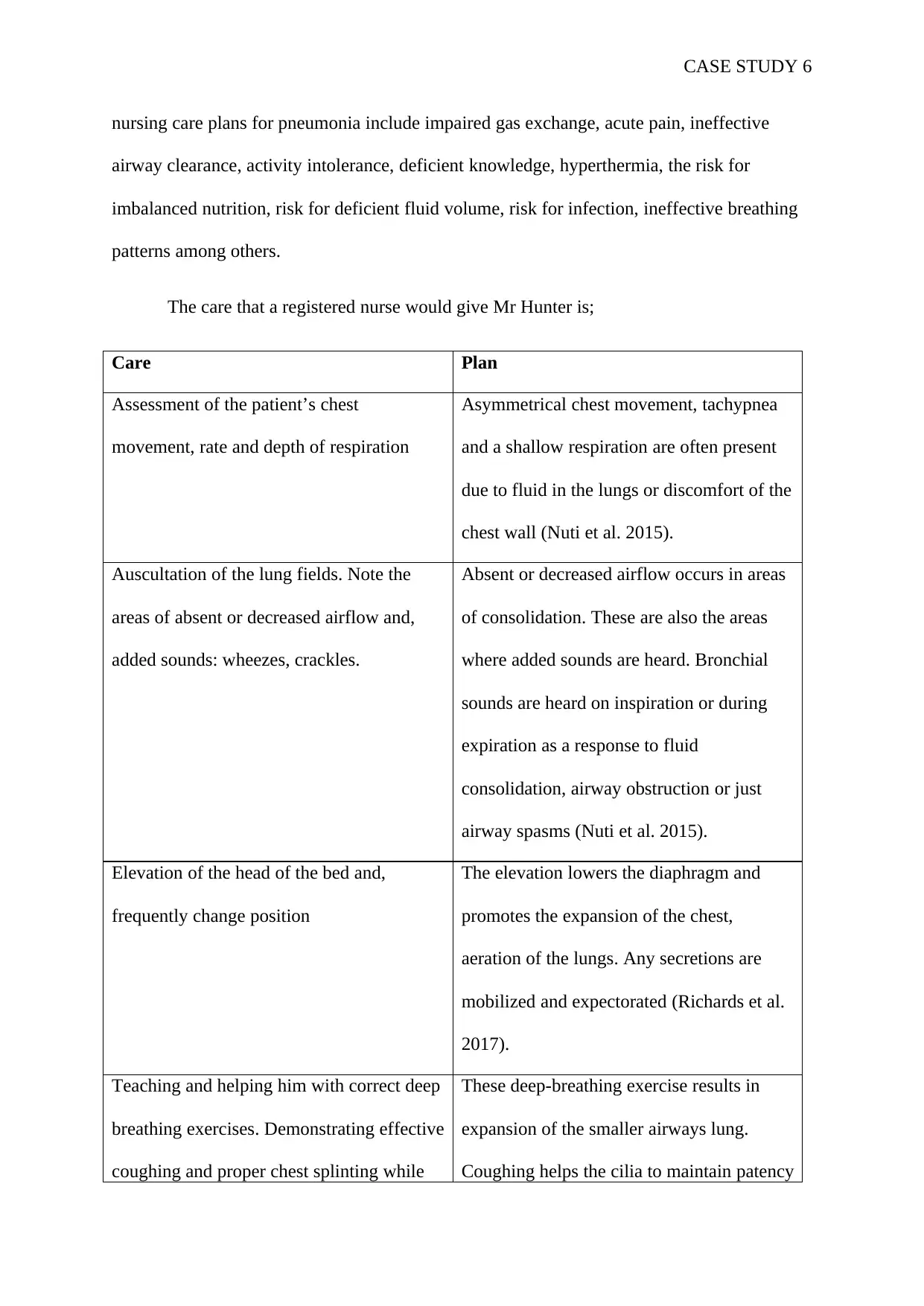
The care that a registered nurse would give Mr Hunter is;
Care Plan
Assessment of the patient’s chest
movement, rate and depth of respiration
Asymmetrical chest movement, tachypnea
and a shallow respiration are often present
due to fluid in the lungs or discomfort of the
chest wall (Nuti et al. 2015).
Auscultation of the lung fields. Note the
areas of absent or decreased airflow and,
added sounds: wheezes, crackles.
Absent or decreased airflow occurs in areas
of consolidation. These are also the areas
where added sounds are heard. Bronchial
sounds are heard on inspiration or during
expiration as a response to fluid
consolidation, airway obstruction or just
airway spasms (Nuti et al. 2015).
Elevation of the head of the bed and,
frequently change position
The elevation lowers the diaphragm and
promotes the expansion of the chest,
aeration of the lungs. Any secretions are
mobilized and expectorated (Richards et al.
2017).
Teaching and helping him with correct deep
breathing exercises. Demonstrating effective
coughing and proper chest splinting while
These deep-breathing exercise results in
expansion of the smaller airways lung.
Coughing helps the cilia to maintain patency
nursing care plans for pneumonia include impaired gas exchange, acute pain, ineffective
airway clearance, activity intolerance, deficient knowledge, hyperthermia, the risk for
imbalanced nutrition, risk for deficient fluid volume, risk for infection, ineffective breathing
patterns among others.
The care that a registered nurse would give Mr Hunter is;
Care Plan
Assessment of the patient’s chest
movement, rate and depth of respiration
Asymmetrical chest movement, tachypnea
and a shallow respiration are often present
due to fluid in the lungs or discomfort of the
chest wall (Nuti et al. 2015).
Auscultation of the lung fields. Note the
areas of absent or decreased airflow and,
added sounds: wheezes, crackles.
Absent or decreased airflow occurs in areas
of consolidation. These are also the areas
where added sounds are heard. Bronchial
sounds are heard on inspiration or during
expiration as a response to fluid
consolidation, airway obstruction or just
airway spasms (Nuti et al. 2015).
Elevation of the head of the bed and,
frequently change position
The elevation lowers the diaphragm and
promotes the expansion of the chest,
aeration of the lungs. Any secretions are
mobilized and expectorated (Richards et al.
2017).
Teaching and helping him with correct deep
breathing exercises. Demonstrating effective
coughing and proper chest splinting while
These deep-breathing exercise results in
expansion of the smaller airways lung.
Coughing helps the cilia to maintain patency
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide
CASE STUDY 7
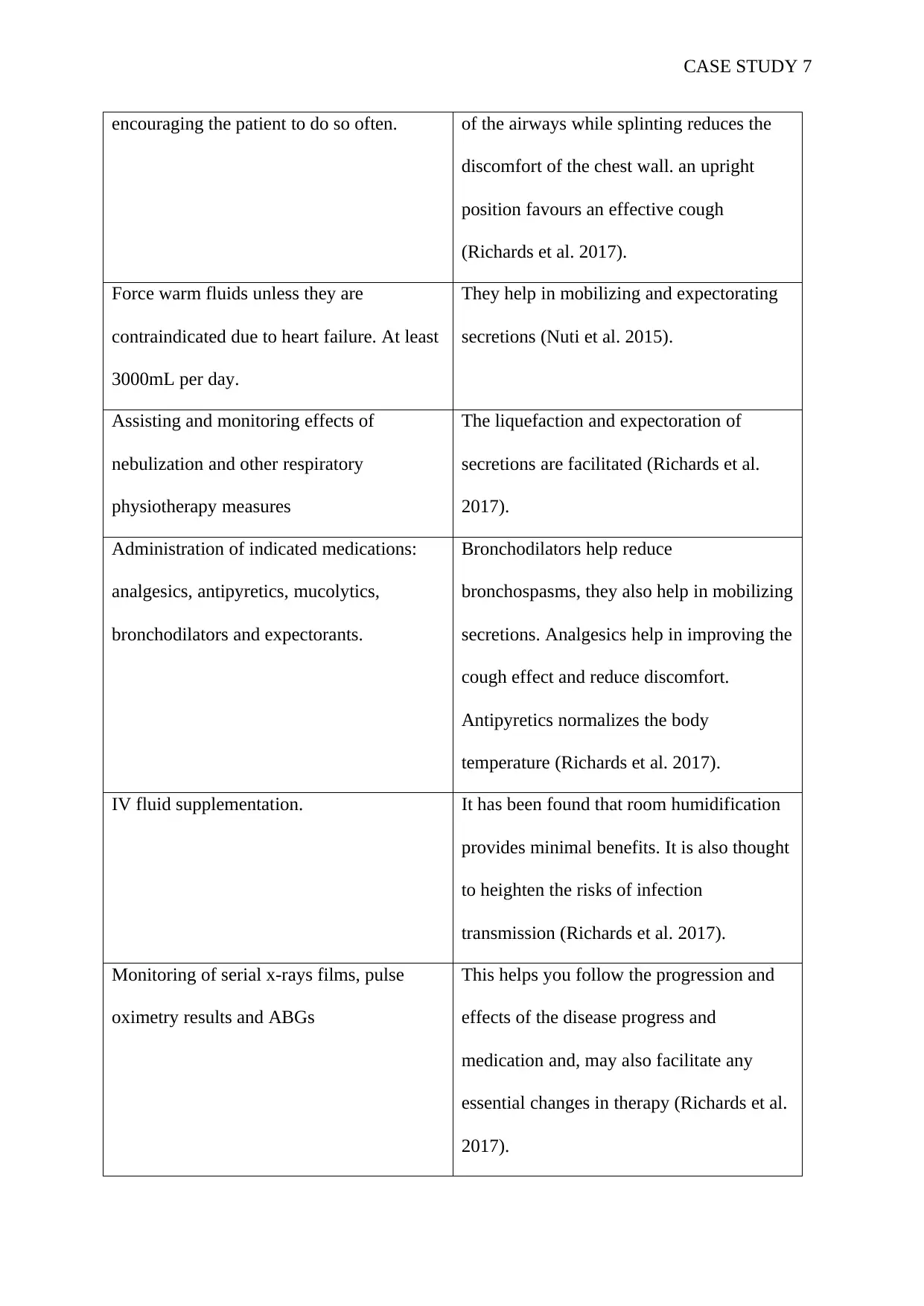
encouraging the patient to do so often. of the airways while splinting reduces the
discomfort of the chest wall. an upright
position favours an effective cough
(Richards et al. 2017).
Force warm fluids unless they are
contraindicated due to heart failure. At least
3000mL per day.
They help in mobilizing and expectorating
secretions (Nuti et al. 2015).
Assisting and monitoring effects of
nebulization and other respiratory
physiotherapy measures
The liquefaction and expectoration of
secretions are facilitated (Richards et al.
2017).
Administration of indicated medications:
analgesics, antipyretics, mucolytics,
bronchodilators and expectorants.
Bronchodilators help reduce
bronchospasms, they also help in mobilizing
secretions. Analgesics help in improving the
cough effect and reduce discomfort.
Antipyretics normalizes the body
temperature (Richards et al. 2017).
IV fluid supplementation. It has been found that room humidification
provides minimal benefits. It is also thought
to heighten the risks of infection
transmission (Richards et al. 2017).
Monitoring of serial x-rays films, pulse
oximetry results and ABGs
This helps you follow the progression and
effects of the disease progress and
medication and, may also facilitate any
essential changes in therapy (Richards et al.
2017).
encouraging the patient to do so often. of the airways while splinting reduces the
discomfort of the chest wall. an upright
position favours an effective cough
(Richards et al. 2017).
Force warm fluids unless they are
contraindicated due to heart failure. At least
3000mL per day.
They help in mobilizing and expectorating
secretions (Nuti et al. 2015).
Assisting and monitoring effects of
nebulization and other respiratory
physiotherapy measures
The liquefaction and expectoration of
secretions are facilitated (Richards et al.
2017).
Administration of indicated medications:
analgesics, antipyretics, mucolytics,
bronchodilators and expectorants.
Bronchodilators help reduce
bronchospasms, they also help in mobilizing
secretions. Analgesics help in improving the
cough effect and reduce discomfort.
Antipyretics normalizes the body
temperature (Richards et al. 2017).
IV fluid supplementation. It has been found that room humidification
provides minimal benefits. It is also thought
to heighten the risks of infection
transmission (Richards et al. 2017).
Monitoring of serial x-rays films, pulse
oximetry results and ABGs
This helps you follow the progression and
effects of the disease progress and
medication and, may also facilitate any
essential changes in therapy (Richards et al.
2017).
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

CASE STUDY 8
If indicated, assist with thoracentesis and/or
bronchoscopy.
Needed occasionally drain purulent
secretion and removal of mucus plugs.
Prevention of atelectasis (Richards et al.
2017).
Urging the patient to perform regular
coughing and deep-breathing exercises.
Promoting complete drainage of secretions
and full aeration (Nuti et al. 2015).
5) The consultant has asked to be informed if Mr Hunters heart rates rise above 100,
oxygen saturations fall below 90% and his temperature rises above 38.5c. in the context
of a patient with pneumonia, explain the rationale/s for monitoring the specific
parameters requested by the consultant.
Heart rate: Ponikowski et al. (2014) suggest that it is necessary to monitor this
parameter because the heart rate can rise in case of any significant disease of the lung.
Adrenaline levels surge as a result of the stress of being sick. Also, low oxygen levels in the
blood lead to an increased heartbeat. Furthermore, pneumonia is capable of pushing the heart
into rhythms that are abnormally fast including atrial fibrillation or atrial flutter (Restrepo &
Reyes 2017). The appearance of these two abnormalities is due to high pressure in the blood
vessel of the lungs causing dilation of the right side of the heart which possibly throws off the
electrical system of the heart (Ponikowski et al. 2014).
If indicated, assist with thoracentesis and/or
bronchoscopy.
Needed occasionally drain purulent
secretion and removal of mucus plugs.
Prevention of atelectasis (Richards et al.
2017).
Urging the patient to perform regular
coughing and deep-breathing exercises.
Promoting complete drainage of secretions
and full aeration (Nuti et al. 2015).
5) The consultant has asked to be informed if Mr Hunters heart rates rise above 100,
oxygen saturations fall below 90% and his temperature rises above 38.5c. in the context
of a patient with pneumonia, explain the rationale/s for monitoring the specific
parameters requested by the consultant.
Heart rate: Ponikowski et al. (2014) suggest that it is necessary to monitor this
parameter because the heart rate can rise in case of any significant disease of the lung.
Adrenaline levels surge as a result of the stress of being sick. Also, low oxygen levels in the
blood lead to an increased heartbeat. Furthermore, pneumonia is capable of pushing the heart
into rhythms that are abnormally fast including atrial fibrillation or atrial flutter (Restrepo &
Reyes 2017). The appearance of these two abnormalities is due to high pressure in the blood
vessel of the lungs causing dilation of the right side of the heart which possibly throws off the
electrical system of the heart (Ponikowski et al. 2014).

CASE STUDY 9
Oxygen saturation levels: Pneumonia can be described as an inflammation of the
parenchyma of the lung often caused by pathogens (Liu, Peng & Hua (2015). These
aetiological agents are mainly bacterial and viral agents. Liu, Peng and Hua (2015) contend
that these inflammatory alterations in the lungs impair the normal gaseous exchange process
leading to its clinical presentation. So, hypoxaemia is a major contributor to pneumonia
associated mortality
Body temperature: Monitoring body temperature in pneumonia is essential in the
sense that symptoms usually vary depending on whether the patient’s pneumonia is viral or
bacterial. In bacterial pneumonia, the patient’s body temperature rises as high as 105⁰F. This
pneumonia causes profuse sweating increase pulse rate and rapidly increasing breathing (Ota
et al. 2016).
6) Explain (1) strategy you would use to ensure Mr Hunter understands the implications
of his decisions to refuse the oxygen and (2) the actions you would take to manage the
situation.
Understand the Mr. hunter’s point of view: My first line of questioning Mr Hunter
will focus on what he thinks about oxygen therapy. I will try and understand where he comes
from and why he feels that the decision he has already made is the right one, putting in mind
that patients often baulk from treatment because of issues of communication as Pirinen et al.
(2015) suggest. Perhaps Mr Hunter does not understand why what is being done to him or
why he needs oxygen therapy. This will give me an opportunity to teach him about his
condition and how he would benefit from oxygen therapy.
I will find out why Mr. Hunter does not want the procedure. I will explore his thought
process on the decision he is making and try to clarify the consequences of his decision. I will
discuss with him these concerns, ranging from him not thinking that oxygen therapy is
Oxygen saturation levels: Pneumonia can be described as an inflammation of the
parenchyma of the lung often caused by pathogens (Liu, Peng & Hua (2015). These
aetiological agents are mainly bacterial and viral agents. Liu, Peng and Hua (2015) contend
that these inflammatory alterations in the lungs impair the normal gaseous exchange process
leading to its clinical presentation. So, hypoxaemia is a major contributor to pneumonia
associated mortality
Body temperature: Monitoring body temperature in pneumonia is essential in the
sense that symptoms usually vary depending on whether the patient’s pneumonia is viral or
bacterial. In bacterial pneumonia, the patient’s body temperature rises as high as 105⁰F. This
pneumonia causes profuse sweating increase pulse rate and rapidly increasing breathing (Ota
et al. 2016).
6) Explain (1) strategy you would use to ensure Mr Hunter understands the implications
of his decisions to refuse the oxygen and (2) the actions you would take to manage the
situation.
Understand the Mr. hunter’s point of view: My first line of questioning Mr Hunter
will focus on what he thinks about oxygen therapy. I will try and understand where he comes
from and why he feels that the decision he has already made is the right one, putting in mind
that patients often baulk from treatment because of issues of communication as Pirinen et al.
(2015) suggest. Perhaps Mr Hunter does not understand why what is being done to him or
why he needs oxygen therapy. This will give me an opportunity to teach him about his
condition and how he would benefit from oxygen therapy.
I will find out why Mr. Hunter does not want the procedure. I will explore his thought
process on the decision he is making and try to clarify the consequences of his decision. I will
discuss with him these concerns, ranging from him not thinking that oxygen therapy is
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide

CASE STUDY 10
necessary to his underlying fears. I will bring them to light and talk to Mr Hunter about them
and make sure that his decision is informed and negotiate a solution that is acceptable.
7a) What are the two most important things that you have learned from this scenario
and why?
First and foremost, I have learnt that none of us should be subject to the kind of
treatment that we do not at all wish to receive even though there is a lot more to story that just
saying no to treatment. Secondly, I have learnt that by trying to see the patient's side of view
about a situation and using my communication skills, I can help my patients to overcome any
fright; I can assist them to make the best possible decisions for their care. I have learnt that if
the patient’s decision involves refusing care, then I as a nurse must come to an acceptance of
the patient’s decision, regardless of how much I would disagree with the patient.
b) What actions will you take in your future practice because of what you have learned
from this scenario?
From this scenario, I have learnt that as a nurse, communication is the most
fundamental thing to consider when a patient refuses care. In my future practice, as much as
we need to respect the wishes of our patients, I will take every necessary step to save the life
of my patients. In case I will encounter such a scenario in my future practice, I will need to
assure my patient that they understand the decisions they are making and what the
consequences of their choice mean. I believe that this will give me an opportunity to teach the
patient. Also, this will give me a chance to learn to accept patients’ wishes which go against
my training.
c) In your reflection identify which of the NMBA Registered Nurse Standards for
practice relate to what you have learnt and how your practice will change.
necessary to his underlying fears. I will bring them to light and talk to Mr Hunter about them
and make sure that his decision is informed and negotiate a solution that is acceptable.
7a) What are the two most important things that you have learned from this scenario
and why?
First and foremost, I have learnt that none of us should be subject to the kind of
treatment that we do not at all wish to receive even though there is a lot more to story that just
saying no to treatment. Secondly, I have learnt that by trying to see the patient's side of view
about a situation and using my communication skills, I can help my patients to overcome any
fright; I can assist them to make the best possible decisions for their care. I have learnt that if
the patient’s decision involves refusing care, then I as a nurse must come to an acceptance of
the patient’s decision, regardless of how much I would disagree with the patient.
b) What actions will you take in your future practice because of what you have learned
from this scenario?
From this scenario, I have learnt that as a nurse, communication is the most
fundamental thing to consider when a patient refuses care. In my future practice, as much as
we need to respect the wishes of our patients, I will take every necessary step to save the life
of my patients. In case I will encounter such a scenario in my future practice, I will need to
assure my patient that they understand the decisions they are making and what the
consequences of their choice mean. I believe that this will give me an opportunity to teach the
patient. Also, this will give me a chance to learn to accept patients’ wishes which go against
my training.
c) In your reflection identify which of the NMBA Registered Nurse Standards for
practice relate to what you have learnt and how your practice will change.
Paraphrase This Document
Need a fresh take? Get an instant paraphrase of this document with our AI Paraphraser

CASE STUDY 11
Standard 2; A registered nurse takes part in professional and therapeutic
relationships: I have learnt that the practice of registered nursing is grounded on positive
engagement in effectual professional and therapeutic relations including shared generosity in
terms of mutual respect and trust in professional relations (Birks et al. 2016). As a nurse, I
will establish, sustain and conclude relations in a way that will differentiate the barriers
between personal and professional relationships. In my practice, I will communicate
effectively and respectively; upholding individual dignities, cultures, values, rights and
beliefs. I will offer support and direct persons to resources with the aim of optimising
healthcare-related decisions. I will actively foster a learning and safety culture that would
include engaging not only the healthcare professionals but also others, in order to exchange
knowledge and skills which support person-centred care and I will lead or take part in a
collaborative practice.
Bibliography
Standard 2; A registered nurse takes part in professional and therapeutic
relationships: I have learnt that the practice of registered nursing is grounded on positive
engagement in effectual professional and therapeutic relations including shared generosity in
terms of mutual respect and trust in professional relations (Birks et al. 2016). As a nurse, I
will establish, sustain and conclude relations in a way that will differentiate the barriers
between personal and professional relationships. In my practice, I will communicate
effectively and respectively; upholding individual dignities, cultures, values, rights and
beliefs. I will offer support and direct persons to resources with the aim of optimising
healthcare-related decisions. I will actively foster a learning and safety culture that would
include engaging not only the healthcare professionals but also others, in order to exchange
knowledge and skills which support person-centred care and I will lead or take part in a
collaborative practice.
Bibliography

CASE STUDY 12
Birks, M, Davis, J, Smithson, J, & Cant, R 2016, ‘Registered nurse scope of practice in
Australia: an integrative review of the literature’, Contemporary Nurse, vol. 52, no. 5,
pp.522-543, doi: 10.1080/10376178.2016.1238773
Blot, S, Koulenti, D, Dimopoulos, G, Martin, C, Komnos, A, Krueger, WA, Spina, G,
Armaganidis, A & Rello, J 2014, ‘Prevalence, risk factors, and mortality for ventilator-
associated pneumonia in middle-aged, old, and very old critically ill patients’, Critical care
medicine, vol. 42, no. 3, pp.601-609, doi: 10.1097/01.ccm.0000435665.07446.50
El-Rabbany, M, Zaghlol, N, Bhandari, M & Azarpazhooh, A 2015, ‘Prophylactic oral health
procedures to prevent hospital-acquired and ventilator-associated pneumonia: a systematic
review’, International journal of nursing studies, vol. 52, no. 1, pp. 452-464, doi:
10.1016/j.ijnurstu.2014.07.010
Ewan, V, Hellyer, T, Newton, J & Simpson, J 2017, ‘New horizons in hospital acquired
pneumonia in older people’, Age and ageing, vol. 46, no.3, pp.352-358, doi:
10.1177/205064061773505
Kalil, AC, Metersky, ML, Klompas, M, Muscedere, J, Sweeney, DA, Palmer, LB,
Napolitano, LM, O'grady, NP, Bartlett, JG, Carratalà, J & El Solh, AA 2016, ‘Management
of adults with hospital-acquired and ventilator-associated pneumonia: 2016 clinical practice
guidelines by the Infectious Diseases Society of America and the American Thoracic
Society’, Clinical Infectious Diseases, vol. 63, no. 5, pp.e61-e111, doi: 10.1093/cid/ciw353
Komiya, K, Ishii, H & Kadota, JI 2015, ‘Healthcare-associated pneumonia and aspiration
pneumonia’, Aging and disease, vol. 6, no. 1, p.27, doi: 10.14336/AD.2014.0127
Lee, N, Walsh, E, Sander, I, Stolper, R, Zakar, J, Rosa, GDL, Wyffels, V, Myers, D &
Fleischhackl, R 2017, ‘October. Impact of Timing of Diagnosis of Respiratory Syncytial
Birks, M, Davis, J, Smithson, J, & Cant, R 2016, ‘Registered nurse scope of practice in
Australia: an integrative review of the literature’, Contemporary Nurse, vol. 52, no. 5,
pp.522-543, doi: 10.1080/10376178.2016.1238773
Blot, S, Koulenti, D, Dimopoulos, G, Martin, C, Komnos, A, Krueger, WA, Spina, G,
Armaganidis, A & Rello, J 2014, ‘Prevalence, risk factors, and mortality for ventilator-
associated pneumonia in middle-aged, old, and very old critically ill patients’, Critical care
medicine, vol. 42, no. 3, pp.601-609, doi: 10.1097/01.ccm.0000435665.07446.50
El-Rabbany, M, Zaghlol, N, Bhandari, M & Azarpazhooh, A 2015, ‘Prophylactic oral health
procedures to prevent hospital-acquired and ventilator-associated pneumonia: a systematic
review’, International journal of nursing studies, vol. 52, no. 1, pp. 452-464, doi:
10.1016/j.ijnurstu.2014.07.010
Ewan, V, Hellyer, T, Newton, J & Simpson, J 2017, ‘New horizons in hospital acquired
pneumonia in older people’, Age and ageing, vol. 46, no.3, pp.352-358, doi:
10.1177/205064061773505
Kalil, AC, Metersky, ML, Klompas, M, Muscedere, J, Sweeney, DA, Palmer, LB,
Napolitano, LM, O'grady, NP, Bartlett, JG, Carratalà, J & El Solh, AA 2016, ‘Management
of adults with hospital-acquired and ventilator-associated pneumonia: 2016 clinical practice
guidelines by the Infectious Diseases Society of America and the American Thoracic
Society’, Clinical Infectious Diseases, vol. 63, no. 5, pp.e61-e111, doi: 10.1093/cid/ciw353
Komiya, K, Ishii, H & Kadota, JI 2015, ‘Healthcare-associated pneumonia and aspiration
pneumonia’, Aging and disease, vol. 6, no. 1, p.27, doi: 10.14336/AD.2014.0127
Lee, N, Walsh, E, Sander, I, Stolper, R, Zakar, J, Rosa, GDL, Wyffels, V, Myers, D &
Fleischhackl, R 2017, ‘October. Impact of Timing of Diagnosis of Respiratory Syncytial
⊘ This is a preview!⊘
Do you want full access?
Subscribe today to unlock all pages.

Trusted by 1+ million students worldwide
1 out of 16
Your All-in-One AI-Powered Toolkit for Academic Success.
+13062052269
info@desklib.com
Available 24*7 on WhatsApp / Email
![[object Object]](/_next/static/media/star-bottom.7253800d.svg)
Unlock your academic potential
Copyright © 2020–2026 A2Z Services. All Rights Reserved. Developed and managed by ZUCOL.

